DSM-III AND THE REVOLUTION IN THE CLASSIFICATION OF MENTAL ILLNESS
Journal of the History of the Behavioral Sciences
by Rick Mayes and Allan V. Horwitz
Summer 2005… With the DSM-III, biomedical investigators replaced clinicians as the most influential voices in the field. Even though few of those involved in Spitzer’s task force were associated with work on psychopharmacology or the biology of mental disorders, the biological default in what they proposed came about as one of the assumptions of neo- Kraepelinians—that the core symptoms of mental disorders stemmed from some form of brain malfunctioning. Consequently, psychotherapy became the primary domain of clinical psychologists, counselors, and social workers, who appeared to practice it as effectively as psychiatrists but who charged less. Psychopharmacological therapy became the private “turf ” of medically trained psychiatrists.
CONCLUSIONThe publication of the DSM-III in 1980 caused a revolution in psychiatry. It also triggered a paradigm shift in how society came to view mental health. Prior to the DSM-III, psychiatrists primarily targeted the underlying psychological causes of mental illness and disorder with psychotherapy. Alternative approaches, such as behavioral therapy, were subordinated to the dominance of psychodynamic theory and practice. With the DSM-III, they gradually shifted to primarily targeting the symptoms of mental illness and disorder with psychopharmacology, the use of drugs to treat mental ills. The direct and indirect institutional change the new manual produced extended far beyond psychiatry, because the DSM is used by clinicians, the courts, researchers, insurance companies, managed care organizations, and the government (NIMH, FDA, Medicaid, Medicare). As a classificatory scheme, it categorizes people as normal or disabled, healthy or sick. And as the definitive manual for measuring and defining illness and disorders, it operates as mental health care’s official language for clinical research, financial reimbursement, and professional expertise. Few professional documents compare to the DSM in terms of affecting the welfare of so many people.The DSM-III’s creation was not the result of a carefully orchestrated conspiracy, but neither was it an accident or “chance-like sequence” of events as some have argued. It did not stem from any new knowledge about the causes of mental illnesses nor their treatments. In addition, it did not enlarge the realm of behaviors that the psychiatric profession was to treat. Instead, its symptom-based focus stemmed from the efforts of research-oriented psychiatrists who wanted to standardize diagnostic criteria and focus attention on the symptoms of mental disorders, rather than on their underlying causes…
The struggle over the drafting and publication of the DSM-III appeared to be a clinical debate among psychiatrists, but underlying it all was a vehement political struggle for professional status and direction. “DSM-III is a political document in many ways,” observed Gerald Klerman. “It appeared in response to some of the ideological and theoretical tensions within the profession of psychiatry. It also has been caught up in the rivalries and tensions among the various mental health professions—psychiatrists, social work, psychology”.
Finally, while the DSM-III standardized the diagnostic classification scheme for mental illnesses and disorders, it did not include treatment guidelines. By virtue of its Kraepelinian orientation, however, it allowed pharmaceutical companies to market their products for a growing number of specific, symptom-based disease entities. The DSM-III unintentionally positioned psychopharmacology on a growth trajectory that various institutions—insurance companies, managed care organizations, pharmaceutical companies, and the government—propelled significantly in subsequent years as they responded to the DSM-III’s new diagnostic guidelines and the research incentives that it fostered.
At the time the DSM III came out, I didn’t know the things the article clarifies. What I knew was that it was a symptom listing that seemed arbitrary that neither helped me nor the patients I saw very much. It was intended to be atheoretical, but it implied the theory that patients with mental illness could be grouped into syndromes based on symptom lists, that those groupings were known and represented in the DSM III, and that those groups had a group treatment. Since then, it has been through revisions [DSM III, DSM III-R, DSM IV, DSM IV-R, DSM V], but to my eyes, it hasn’t changed very much. I think my initial reaction was not far off the mark – that some mentally ill people can be grouped by symptoms, but many can’t. The DSM has created a world that is the way a lot of people want things to be, not how they are – wishful fantasy mingled in with some facts.
And that’s how things have played out. The groupings became entities. The entities became the objects of study [eg drug treatments, CBT, etc.]. And now we have this – evidence-based medicine:
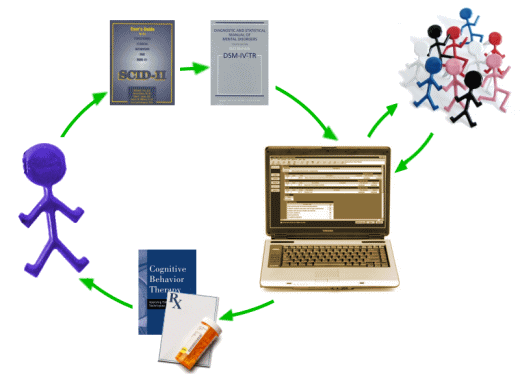
We are to use a structured interview to precisely locate the patient in the groupings defined by the DSM IV-TR. That allows the computer’s alogorithic to decide on treatment to be matched with the research and clinical trials done on the specific group. Treatment recommendations are then made using modalities proven to be statistically helpful to the identified group. Meaning: The only valid treatments are those that can be validated by clinical trials on a group. If you believe that the  DSM IV-TR or its coming soon successor contains groups that adequately define your patient, it makes perfect sense. Unfortunately, I don’t believe that for all of the groups, so it’s hard for me to get with the program. I’m particularly wary of the grouping of depressed people – some of whom I would gladly accept fit the medical model, but others who definitely don’t [and , by the way, I’m still back in the days where Manic-Depressive made sense and the modern Bipolar "mania" doesn’t].
DSM IV-TR or its coming soon successor contains groups that adequately define your patient, it makes perfect sense. Unfortunately, I don’t believe that for all of the groups, so it’s hard for me to get with the program. I’m particularly wary of the grouping of depressed people – some of whom I would gladly accept fit the medical model, but others who definitely don’t [and , by the way, I’m still back in the days where Manic-Depressive made sense and the modern Bipolar "mania" doesn’t].
If the point of the DSM system is to say that Insurance Companies are only going to pay for treating patients who can be treated with group-validated modalities, that could be said openly without hiding the message behind a diagnostic classification of mental disorders. And if the point of the DSM system was to say to the Freudians and post-Freudians that their paradigm had been overblown and was not cost-effective, that could also be said openly without hiding the message behind a diagnostic classification of mental disorders. But if the DSM III and later was to be a scientific classification of Mental Illnesses, it was a failure in my book because it hasn’t helped the mentally ill very much, it didn’t help me treat them, and it hasn’t lead to much in the way of scientific advancement – in fact, it created some new problems. I can and did live with the fact that Insurance companies didn’t want to pay people like me to take on patients as individual research projects. In my private practice life, I only saw one patient the whole time that hadn’t been in a number of other treatments who then came and found me wanting to be an n=1. And I agree that dynamic psychiatrists are a niche rather than an umbrella for Psychiatrists. But I don’t agree that medical economics, turf wars within and between specialties, competition between theoretical orientations, etc. are a basis for a scientific classification of diseases. I call foul! Conflict of Interests! And I don’t believe that symptom lists will ever adequately underpin a complete classification of Mental Illness [a point I will pursue further]. I wish the DSM V would classify mental illnesses that do fit the symptom list model validated by some evidence-based methodology, and have another category [a big one] called Mental·Illness.Person·Specific.NOS or just Mental·Illness.NOS [I can’t help it that sometimes I get sort of silly]. On a more serious note, this model advertised as evidence-based medicine has done some real harm – and I’ll proceed with that thought in my next post.
Your research and blogs on this topic are clarifying for me, here at the end of a long career, as to what it’s all been about. I was a few years ahead of you, but we both had our psychiatry residences at Emory at a time when the department was still run by psychoanalysts, and being an analyst was the aspiration of most of us.
Our natural inclinations toward patient-centered treatment, not symptom-based treatment, were fostered further by what we were taught and by whom. That’s very different from the experience residents have had in the past 30 years, increasingly so.
In 1980, I was already long gone from general psychiatry, having left the department for private practice of psychotherapy and psychoanalytic training in the mid-1960s. I never paid that much attention to DSM — never thought much about making a diagnosis unless I had to fill out an insurance form. If patient John Smith asked me what his diagnosis was, I would say: “Your diagnosis is John Smith.”
I think, if DSM and all the ensuing changes had occurred 20 years earlier, I probably wouldn’t have gone into psychiatry. It just wouldn’t have interested me as it has evolved today — except for the psychoanalytic influences that are still there at Emory and a few other places.