In the last post, I reviewed Drs. Rush and Trivedi’s studies on the TMAP patients. They were buoyed up by the fact that the clinics using their algorithms [ALGO] outperformed their clinics where the docs were left to their own devices [TAU], even though their reanalysis of the data when they eliminated the psychotic patients and the milder cases wasn’t very exciting in its own right. But where there’s an algorithm, can a computer be far behind? In 2003, Dr. Trevidi received an NIMH grant [5 year] to implement the TMAP algorithm in a software system and test it:
| COMPUTERIZED DECISION SUPPORT SYSTEM FOR DEPRESSION | ||||
| PROJECT | PRINCIPLE INVESTIGATOR | YEAR | FUNDING | AMOUNT |
| 1R01MH064062-01A2 | TRIVEDI, MADHUKAR H | 2003 | NIMH | $604,135 |
| 5R01MH064062-02 | TRIVEDI, MADHUKAR H | 2004 | NIMH | $698,180 |
| 5R01MH064062-03 | TRIVEDI, MADHUKAR H | 2005 | NIMH | $717,974 |
| 5R01MH064062-04 | TRIVEDI, MADHUKAR H | 2006 | NIMH | $718,293 |
| 5R01MH064062-05 | TRIVEDI, MADHUKAR H | 2007 | NIMH | $605,420 |
| TOTAL |
$3,344,002 | |||
Background: Despite wide promotion, clinical practice guidelines have had limited effect in changing physician behavior. Effective implementation strategies to date have included: multifaceted interventions involving audit and feedback, local consensus processes, marketing; reminder systems, either manual or computerized; and interactive educational meetings. In addition, there is now growing evidence that contextual factors affecting implementation must be addressed such as organizational support (leadership procedures and resources) for the change and strategies to implement and maintain new systems.
Methods: To examine the feasibility and effectiveness of implementation of a computerized decision support system for depression (CDSS-D) in routine public mental health care in Texas, fifteen study clinicians (thirteen physicians and two advanced nurse practitioners) participated across five sites, accruing over 300 outpatient visits on 168 patients.
Results: Issues regarding computer literacy and hardware/software requirements were identified as initial barriers. Clinicians also reported concerns about negative impact on workflow and the potential need for duplication during the transition from paper to electronic systems of medical record keeping.
Conclusion: The following narrative report based on observations obtained during the initial testing and use of a CDSS-D in clinical settings further emphasizes the importance of taking into account organizational factors when planning implementation of evidence-based guidelines or decision support within a system.
OBJECTIVE: In 2004, results from The Texas Medication Algorithm Project (TMAP) showed better clinical outcomes for patients whose physicians adhered to a paper-and-pencil algorithm compared to patients who received standard clinical treatment for major depressive disorder (MDD). However, implementation of and fidelity to the treatment algorithm among various providers was observed to be inadequate. A computerized decision support system (CDSS) for the implementation of the TMAP algorithm for depression has since been developed to improve fidelity and adherence to the algorithm.
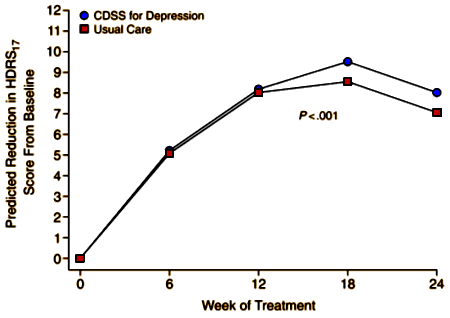
METHOD: This was a 2-group, parallel design, clinical trial (one patient group receiving MDD treatment from physicians using the CDSS and the other patient group receiving usual care) conducted at 2 separate primary care clinics in Texas from March 2005 through June 2006. Fifty-five patients with MDD (DSM-IV criteria) with no significant difference in disease characteristics were enrolled, 32 of whom were treated by physicians using CDSS and 23 were treated by physicians using usual care. The study’s objective was to evaluate the feasibility and efficacy of implementing a CDSS to assist physicians acutely treating patients with MDD compared to usual care in primary care. Primary efficacy outcomes for depression symptom severity were based on the 17-item Hamilton Depression Rating Scale (HDRS(17)) evaluated by an independent rater.
RESULTS: Patients treated by physicians employing CDSS had significantly greater symptom reduction, based on the HDRS(17), than patients treated with usual care (P < .001).
CONCLUSIONS: The CDSS algorithm, utilizing measurement-based care, was superior to usual care for patients with MDD in primary care settings. Larger randomized controlled trials are needed to confirm these findings.
“And Rush had left Trivedi to mop up CO-MED [another dud].â€
I chuckled at this one. Seriously though, who will mop up the mess in the scientific literature?
One wonders if there is any “scientific” literature out there any more. Medicine has become so corrupted by Pharma payouts and buyouts that “scientific literature” may now be an oxymoron. In this regard, I just finished reading a NY Times article about how older diabetes drugs are now considered to be “best.” What has gone on over the past 25 years in “academic medicine” (another oxymoron) is criminal. But the perps (e.g KOL’s) have no shame. Sadly, we do indeed live in a “post superego” age.