The other day, I encountered two things almost simultaneously. The first was a 2007 Journal Supplement on Melancholia that I found compelling. As I was reading through the articles, someone sent me a link to an abstract I hadn’t seen from Drs. Rush and Trivedi – a policy piece about Measurement Based Care. There was a striking contrast between articles in the Supplement and the later Abstract, and they lingered in my mind together through several busy days.
The 2007 Supplement in the Acta Psychiatrica Scandinavica was called Melancholia: Beyond DSM, Beyond Neurotransmitters [I liked both "beyonds"]. It was from a conference in Copenhagen in 2006. I felt nostalgia as I read through the various articles. They were like journals used to be before they got filled up with clinical trials. The Preface set the stage for the conference:
Resurrecting melancholia
by M. Fink & M. A. Taylor
Acta Psychiatrica Scandinavica 115[s433]:14–20, 2007.
AbstractObjective: To define melancholia as a distinct mood disorder, identified by unremitting depressed mood, vegetative dysfunction, and psychomotor disturbances, verifiable by neuroendocrine tests, and treatable by electroconvulsive therapy and tricyclic antidepressants.Method: A review of the literature of two centuries finds descriptions of severe mood disorders, either depression or mania or circular, defined as ‘melancholia.’ In the 1980 diagnostic revision (DSM-III), melancholia was relegated to a features specifier only.Results: DSM classification criteria develop heterogeneous patient samples that are neither guides to prognosis nor to treatment response, and confound studies of pathophysiology. Within the large population of mood disorders, a syndrome of melancholia is identifiable by specific behaviors, vegetative signs, and validated by neuroendocrine abnormalities (cortisolemia). Populations so identified are clinically homogeneous and have improved treatment responses. Patients meeting criteria for melancholia are now identified as psychotic depressed, geriatric depressed, postpartum psychosis, and pharmacotherapy resistant.Conclusion: The review supports the establishment of melancholia by empirically derived criteria rather than by a checklist is an alternative to the major depression choice and offers an improved model for psychiatric classification.

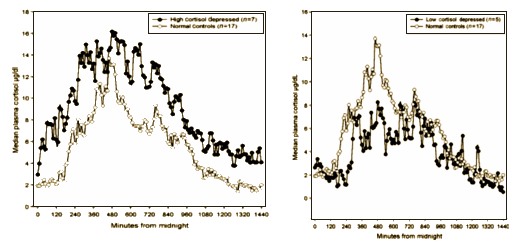
Pathophysiology of hypercortisolism in depression
by B. J. Carroll, F. Cassidy, D. Naftolowitz, N. E. Tatham, W. H. Wilson, A. Iranmanesh, P. Y. Liu, and J. D. Veldhuis
Acta Psychiatrica Scandinavica 115[s433]:90–103,2007.
AbstractObjective: The mechanisms mediating hypercortisolemia in depression remain controversial. Adopting the biomarker strategy, we studied adrenocorticotropin (ACTH) and cortisol dynamics in hypercortisolemic and non-hypercortisolemic depressed in-patients, and in normal volunteers.Method: Deconvolution analysis of 24-h pulsatile secretion, approximate entropy (ApEn) estimation of secretory regularity, cross-ApEn quantitation of forward and reverse ACTH–cortisol synchrony, and cosine regression of 24-h rhythmicity.Results: Hypercortisolemia was strongly associated with melancholic and psychotic depressive subtypes. Hypercortisolemic patients had elevated ACTH and cortisol secretion, mediated chiefly by increased burst masses. Basal ACTH secretion was increased, ACTH half-life was reduced, and mean 24-h ACTH concentration was normal. Cortisol secretion was increased in a highly irregular pattern (high ApEn), with high ACTH → cortisol cross-ApEn (impaired feedforward coupling). Cortisol-mediated feedback on the secretory pattern of ACTH was normal. Hypercortisolemic depressed patients had normal programming of the central hypothalamo–pituitary–adrenal (HPA) axis pulse generator: ACTH pulse frequency, cortisol pulse frequency, circadian acrophases, and ApEn of ACTH secretion were normal. Responsiveness of the adrenal cortex to endogenous ACTH was normal. Non-hypercortisolemic patients resembled hypercortisolemic patients on ACTH regulatory parameters but had low total cortisol secretion.Conclusion: Increased ACTH secretion occurs in depressed in-patients regardless of cortisolemic status, confirming central HPA axis overdrive in severe depression. Depressive hypercortisolemia results from an additional change in the adrenal cortex that causes ACTH-independent, disorderly basal cortisol release, a sign of physiological stress in melancholic/psychotic depression.
The doctrine of the two depressions in historical perspective
by E. Shorter
Acta Psychiatrica Scandinavica 115[s433]:5–13,2007.
AbstractObjective: To determine if the concept of two separate depressions – melancholia and non-melancholia – has existed in writings of the main previous thinkers about mood disorders.Method: Representative contributions to writing on mood disorders over the past hundred years have been systematically evaluated.Results: The concept of two separate depressions does indeed emerge in the psychiatric literature from the very beginning of modern writing about the concept of ‘melancholia’. For the principal nosologists of psychiatry, melancholic depression has always meant something quite different from non-melancholic depression. Exceptions to this include Aubrey Lewis and Karl Leonhard. Yet the balance of opinion among the chief theorists overwhelmingly favors the existence of two quite different illnesses.Conclusion: The concept of ‘major depression’ popularized in DSM-III in 1980 is a historical anomaly. It mixes together psychopathologic entities that previous generations of experienced clinicians and thoughtful nosologists had been at pains to keep separate. Recently, there has been a tendency to return to the concept of two depressions: melancholic and non-melancholic illness. ‘Major depression’ is coming into increasing disfavor. In the next edition of DSM (DSM-V), major depression should be abolished; melancholic mood disorder (MMD) and non-melancholic mood disorder (NMMD) should become two of the principle entities in the mood disorder section.
In those early days of the DSM-III, one frequently heard the argument against "n = 1" science. It was, of course, aimed at psychoanalysis which focused on one case at a time, then generalized to groups. They were saying that was backwards, it should be group findings generalized to individuals. The point has been duly noted and taken. But there’s another way to think about that discussion. For clinicians, it’s always an "n = 1" situation – the one case before you at the moment. It’s how all of medicine is practiced. As such, a meeting of a clinician and a patient should be an encounter between a person with "ill-ness" and the history of medicine’s experience – with an eye on diagnosis, treatment, and management.
Besides the fact that I’m sympathetic to the conclusions in these articles, the things that struck me were their transparency and the fact that they seemed to be written to be read by colleagues. I’ve been reading clinical trial articles for months, and I’m always looking for what’s being buried and what spin is being put on the results – where I’m being lead. I found these articles a refreshing change of pace.
Then this abstract popped up in the middle of my reading:
Measurement-based care in psychiatric practice: a policy framework for implementation.
by Harding KJ, Rush AJ, Arbuckle M, Trivedi MH, Pincus HA.
Journal of Clinical Psychiatry. Jan 11, 2011 [Epub ahead of print]
AbstractThis article describes the need for measurement-based care (MBC) in psychiatric practice and defines a policy framework for implementation. Although measurement in psychiatric treatment is not new, it is not standard clinical practice. Thus a gap exists between research and practice outcomes. The current standards of psychiatric clinical care are reviewed and illustrated by a case example, along with MBC improvements. Measurement-based care is defined for clinical practice along with limitations and recommendations. This article provides a policy top 10 list for implementing MBC into standard practice, including establishing clear expectations and guidelines, fostering practice-based implementation capacities, altering financial incentives, helping practicing doctors adapt to MBC, developing and expanding the MBC science base, and engaging consumers and their families. Measurement-based care as the standard of care could transform psychiatric practice, move psychiatry into the mainstream of medicine, and improve the quality of care for patients with psychiatric illness.
But beyond their presumptuousness, I’ve realized that it’s the way they write. They’re not writing to colleagues, they’re selling a product. In this offering, they’re thinking up ways to get us all to do their measurement-based care thing and proposing a campaign to bring us around – including "financial incentives." Their track record is so lackluster that it’s hard to see why they think we’d want to follow their lead. The last time they did this was TMAP, the now defunct program that was mostly oriented towards getting people to use expensive in patent drugs – drugs made by companies that financed their initiatives and paid them to be consultants and speakers.They haven’t figured out that we read their articles with one eye trained on "what are they trying to get us to do this time?"
]’m going to show this to my doctor – there’s no telling how differently treatment and outcomes could be…I am one of the terminally stressed.
Thanks for noticing our Supplement on melancholia.
The sad thing about much of current clinical research is that it has an agenda, which may be promoting a drug (like experimercials for second generation antipsychotic drugs in depression) or showcasing a programmatic initiative (STAR*D and its cousins) or undisciplined but profitable blue skying (hyperbole about translational research, as in the pitifully unproductive Emory-GlaxoSmithKline-NIMH Mood Disorders Initiative) or data mining for evidence, any evidence, to support a favored theoretical model (combined psychosocial and drug treatment of disorder X).
The price paid for such agenda driven research is steep: The really hard clinical research questions don’t get asked; precious infrastructure resources are squandered in support of misbegotten studies; and young investigators see their mentors preoccupied with scoring points in the grants game instead of dispassionately addressing the important questions.
NIMH under its recent Directors has been an enabler of these perverse trends.
“perverse trends” is a perfect name for it. It’s like the Myth of Sisyphus on purpose. They don’t seem to notice that they never move up the hill…
Despite the impressive scientific EVIDENCE supporting the classification of melancholia as a distinct mood disorder, my read is that the DSM-V committee (AKA the Council of Nicaea) will VOTE to maintain the staus quo as to the major depression classification. In so doing, the conflict of interest-ridden committee will vote the interests of Big Pharma and unethical biological psychiatrists (note I did not say all biological psychiatrists) so as to continue the “push product at all costs to the masses” mind set of current psychiatry. I am just waiting for the inclusion of a “prodromal major depression” category to surface soon.