This post takes a look at what others have found using the idea of an "ultra high risk" group of people that may develop ouvert Schizophrenia. The first study is from The University of Manchester, UK. They looked at the effect of Cognitive Therapy in the high risk group [four articles]:
Randomised controlled trial of early detection and cognitive therapy for preventing transition to psychosis in high-risk individuals. Study design and interim analysis of transition rate and psychological risk factors.
by Morrison AP, Bentall RP, French P, Walford L, Kilcommons A, Knight A, Kreutz M, and Lewis SW.
British Journal of Psychiatry Supplement 2002 43:s78-84.
BACKGROUND: There is interest in the possibility of indicated prevention of psychosis. There is a strong case for using psychological approaches to prevent transition to psychosis in high-risk patients.
AIMS: To identify individuals at high risk of transition to psychosis, and psychological characteristics relevant to the development of psychosis in this group.
METHOD: The design of a randomised controlled trial of cognitive therapy for the prevention of psychosis in people at high risk (meeting operational criteria of brief or attenuated psychotic symptoms, or first-degree family history with functional decline) is outlined. The first patients recruited are compared with non-patient samples on cognitive and personality factors; an interim analysis of transition rate is reported.
RESULTS: Cases (n = 31) were recruited mainly from primary care. Of the 23 high-risk patients monitored for 6-12 months, 5 (22%) made the transition to psychosis. The high-risk group scored significantly higher than non-patients on measures of schizotypy, metacognitive beliefs and dysfunctional self-schemas (sociotropy).
CONCLUSIONS: The findings validate the methods of identifying individuals at high risk of experiencing a psychotic episode. Compared with non-patient controls, the cases showed dysfunctional metacognitive beliefs and self-schemas.
Cognitive therapy for the prevention of psychosis in people at ultra-high risk: randomised controlled trial.
by Morrison AP, French P, Walford L, Lewis SW, Kilcommons A, Green J, Parker S, and Bentall RP.
British Journal of Psychiatry . 2004 185:291-7.
BACKGROUND: Advances in the ability to identify people at high risk of developing psychosis have generated interest in the possibility of preventing psychosis.
AIMS: To evaluate the efficacy of cognitive therapy for the prevention of transition to psychosis.
METHOD: A randomised controlled trial compared cognitive therapy with treatment as usual in 58 patients at ultra-high risk of developing a first episode of psychosis. Therapy was provided over 6 months, and all patients were monitored on a monthly basis for 12 months.
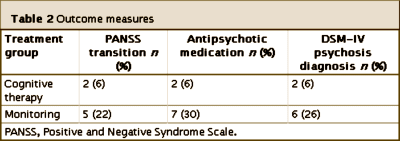
RESULTS: Logistic regression demonstrated that cognitive therapy significantly reduced the likelihood of making progression to psychosis as defined on the Positive and Negative Syndrome Scale over 12 months. In addition, it significantly reduced the likelihood of being prescribed antipsychotic medication and of meeting criteria for a DSM-IV diagnosis of a psychotic disorder. Analysis of covariance showed that the intervention also significantly improved positive symptoms of psychosis in this population over the 12-month period
CONCLUSIONS: Cognitive therapy appears to be an acceptable and efficacious intervention for people at high risk of developing psychosis.
Three-year follow-up of a randomized controlled trial of cognitive therapy for the prevention of psychosis in people at ultrahigh risk.
by Morrison AP, French P, Parker S, Roberts M, Stevens H, Bentall RP, and Lewis SW.
Schizophrenia Bulletin. 2007 33(3):682-7.
There have been recent advances in the ability to identify people at high risk of developing psychosis. This has led to interest in the possibility of preventing the development of psychosis. A randomized controlled trial compared cognitive therapy (CT) over 6 months with monthly monitoring in 58 patients meeting criteria for ultrahigh risk of developing a first episode of psychosis. Participants were followed up over a 3-year period. Logistic regression demonstrated that CT significantly reduced likelihood of being prescribed antipsychotic medication over a 3-year period, but it did not affect transition to psychosis defined using the Positive and Negative Syndrome Scale (PANSS) or probable Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition diagnosis. However, exploratory analyses revealed that CT significantly reduced the likelihood of making progression to psychosis as defined on the PANSS over 3 years after controlling for baseline cognitive factors. Follow-up rate at 3 years was 47%. There appear to be enduring benefits of CT over the long term, suggesting that it is an efficacious intervention for people at high risk of developing psychosis.
Effects of cognitive therapy on the longitudinal development of psychotic experiences in people at high risk of developing psychosis.
by French P, Shryane N, Bentall RP, Lewis SW, and Morrison AP.
British Journal of Psychiatry Supplement 2007 51:s82-7.
BACKGROUND: There have been recent advances in the identification of people at high risk of psychosis and psychological treatments have shown promise for prevention.
AIMS: To compare the longitudinal course of psychotic experiences and emotional dysfunction in high-risk participants receiving cognitive therapy with those receiving treatment as usual.
METHOD: Data from a recent randomised controlled trial of cognitive therapy for people at risk of developing psychosis were utilised to examine three different statistical models that were based on 432 measurements of psychotic experiences and 421 of emotional dysfunction (anxiety-depression) contributed by 57 participants across the 13 measurement occasions (monthly monitoring for a year).
RESULTS: Psychotic experiences and emotional dysfunction were correlated and decreased significantly over the course of the study, with most improvement in the early months. The reduction in positive symptoms, but not emotional dysfunction, was enhanced by allocation to cognitive therapy.
CONCLUSIONS: Psychotic experiences and emotional dysfunction appear to interact in people at risk of developing psychosis. There appears to be a specific benefit of cognitive therapy.
The focus of the Manchester Group seems to be to use Cognitive Therapy as an alternative to medication in this high risk population.Their study confirmed the ability of the "ultra high risk" criteria predictiong coming Schizophrenia, though at a lower transition rate that McGorry [22%]. Their intervention had a statistically significant and clinically relevant effect on the transition rate. For anyone interested, their full text papers have a lot more information of interest than I mention here. The links are included above.
The next study is a collaborative North American clinical trial funded by Eli Lilly, maker of Olanzapine – the study drug. This study addressed only the drug intervention – Olanzapine vs Placebo:
Randomized, double-blind trial of olanzapine versus placebo in patients prodromally symptomatic for psychosis.
by by McGlashan TH, Zipursky RB, Perkins D, Addington J, Miller T, Woods SW, Hawkins KA, Hoffman RE, Preda A, Epstein I, Addington D, Lindborg S, Trzaskoma Q, Tohen M, and Breier A.
American Journal of Psychiatry. 2006 163(5):790-9.
[full text online]
OBJECTIVE: This study assessed the efficacy of olanzapine in delaying or preventing conversion to psychosis and reducing symptoms in people with prodromal symptoms of schizophrenia.
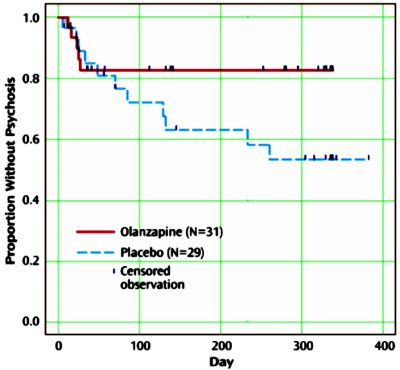
METHOD: This randomized trial occurred at four North American clinics in the Prevention Through Risk Identification, Management, and Education project. Outpatients received olanzapine (5-15 mg/day, N=31) or placebo (N=29) during a 1-year double-blind treatment period and no treatment during a 1-year follow-up period. Efficacy measures included the conversion-to-psychosis rate and Scale of Prodromal Symptoms scores.
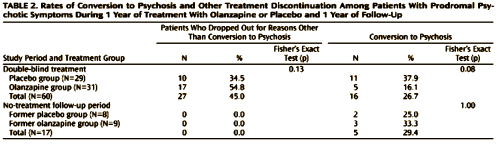
RESULTS: During the treatment year, 16.1% of olanzapine patients and 37.9% of placebo patients experienced a conversion to psychosis, a nearly significant difference. The hazard of conversion among placebo patients was about 2.5 times that among olanzapine-treated patients, which also approached significance. In the follow-up year, the conversion rate did not differ significantly between groups. During treatment, the mean score for prodromal positive symptoms improved more in the olanzapine group than in the placebo group, and the mixed-model repeated-measures least-squares mean score showed significantly greater improvement between weeks 8 and 28 with olanzapine. The olanzapine patients gained significantly more weight (mean=8.79 kg, SD=9.05, versus mean=0.30 kg, SD=4.24).
CONCLUSIONS: A significant treatment difference in the conversion-to-psychosis rate was not demonstrated. However, these results may be influenced by low power. The nearly significant differences suggest that olanzapine might reduce the conversion rate and delay onset of psychosis. Olanzapine was efficacious for positive prodromal symptoms but induced weight gain. Further treatment research in this phase of illness is warranted.
This study had many of the characteristics of industry-funded studies of the era. There were no conflict of interest declarations and it’s unknown if any of the authors were Eli Lilly employees. There were high drop-out rates in both groups and the correction methodology was opaque.
A greater proportion of placebo treated subjects developed ouvert psychosis, but the differences were not significant, though the authors suggested the "nearly significant" values might be meaningful.
One useful take-away from the study was that 21/60 developed psychosis, seeming to validate the reported criteria and transition rate [35%].
The final study is from Copenhagen:
Transition rates from schizotypal disorder to psychotic disorder for first-contact patients included in the OPUS trial.
A randomized clinical trial of integrated treatment and standard treatment.
by Nordentoft M, Thorup A, Petersen L, Ohlenschlaeger J, Melau M, Christensen TØ, Krarup G, Jørgensen P, and Jeppesen P.
Schizophrenia Research. 2006 83(1):29-40.
BACKGROUND: Only a few randomized clinical trials have tested the effect on transition rates of intervention programs for patients with sub-threshold psychosis-like symptoms.
AIM: To examine whether integrated treatment reduced transition to psychosis for first-contact patients diagnosed with schizotypal disorder.
METHODS: Seventy-nine patients were randomized to integrated treatment or standard treatment. Survival analysis with multivariate Cox-regression was used to identify factors determinant for transition to psychotic disorder.
RESULTS: In the multivariate model, male gender increased risk for transition to psychotic disorder (relative risk=4.47, (confidence interval 1.30-15.33)), while integrated treatment reduced the risk (relative risk=0.36 (confidence interval 0.16-0.85)). At two-year follow-up, the proportion diagnosed with a psychotic disorder was 25.0% for patients randomized to integrated treatment compared to 48.3% for patients randomized to standard treatment.
CONCLUSION: Integrated treatment postponed or inhibited onset of psychosis in significantly more cases than standard treatment.
While the abstract is terse, this is a solid study with thoughtful comments on the other studies reviewed above. Their intervention did not control all variables in that all subjects had treating physicians delivering treatment as usual including medications. Their integrated treatment was "borrowed" from their approach to first episode Schizophrenic patients rather than a specific CBT therapy. It involved the intensive application of more traditional methodologies:
Integrated treatment
The intervention period was two years. Elements in integrated treatment were:
(a) A modified Assertive Community Treatment model (Stein and Test, 1980) focusing on young, first-episode psychotic patients, and provided by a multidisciplinary team (psychiatrist, psychologist, psychiatric nurse, occupational therapist and social worker). Case load was 1: 10; home visits were an integrated part of the treatment model. The team member with primary responsibility for the patient provided regular assessment of symptoms (weekly) and, for patients with comorbid drug abuse, focused on helping the patient to reduce abuse of drugs.
(b) Social skills training either in groups or individually (Liberman et al., 1986).
(c) Psycho-education in multiple-family groups was offered to patients and their family members or friends (McFarlane et al., 1995; Jeppesen et al., 2005).
This table summarizes their findings:
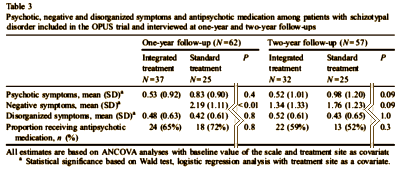
[abbreviated for readability]
They provide a useful tabulation of most of the studies to date reproduced below:
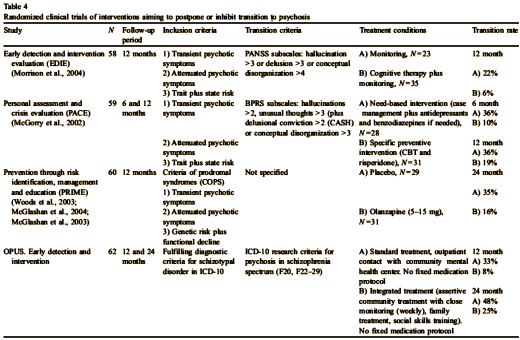
I was going to end this with a table comparing the different studies, but the Danish paper already did that for us. I’ll save my comments for the next post…
Regarding the authors of the 2006 paper in American Journal of Psychiatry, at least 2 indeed were Lilly employees – Mauricio Tohen and Alan Breier. Both were at the time psychiatrists with major responsibility for the Zyprexa (olanzapine) account. Back in January 2007 I challenged Dr. Breier, whom I have known for years, about Lilly’s statements concerning whether Zyprexa causes diabetes. Here is my message to him:
Dear Alan,
A week or two after our annual ACNP meeting the New York Times ran a series on Lilly’s drug olanzapine (Zyprexa). I realize there are major legal issues concerning the publishing of internal documents, and that you have been involved on behalf of the company in responding to statements that are circulating.
Without wishing to add to your tasks, and in a constructive spirit, I would like to ask you and the company to reconsider one of the statements from Lilly that was cited in the NYT, namely, “In summary, there is no scientific evidence establishing that Zyprexa causes diabetes.â€
To my reading, this resembles the mantra of the tobacco industry for 30 years through the 1960s – 1980s that there is no scientific evidence establishing that smoking cigarettes causes lung cancer. I suppose it all depends what the word cause is intended to mean. Whatever, I suggest to you that such a statement is certainly counterproductive from a public relations point of view, while being a puzzlement to your scientific friends.
Cordially, Barney.
Dr. Breier never responded. Subsequently, Lilly was obliged to settle up big time over this issue.
As for the results given in the 2006 prevention study, one cannot conclude much from intent to treat analyses when the dropout rate is as high as 45%. One would like to know the comparative results in those who actually completed the 12 month prevention period. Those can be derived from the published article and they are even less impressive – the P value is clearly nonsignificant at 0.30. Rates of conversion to psychosis were 11 of 19 on placebo and 5 of 14 on Zyprexa. The authors did not reveal this analysis, however.
Overall, this article is a good example of the hand waving and special pleading around nonsignificant results that litter our scientific journals in service of wishful thinking and commercial aspirations.