It’s my ‘season’ – ragweed – so I watch this part of the Fall through a window. So my nose around the computer time is increased. In the process of looking into the McGorry Controversy in Australia, I had looked at the criteria he used to select his patients. His criteria were based on the Prodromal or Residual Symptoms in the DSM-IIIR which was the contemporary version back when he was first looking into his ultra high risk group:
| Prodromal or Residual Symptoms – DSM-IIIR |
|
| [1] | marked social isolation or withdrawal |
| [2] | marked impairment in role functioning as wage-earner, student, or home-maker |
| [3] | markedly peculiar behavior [eg collecting garbage, talking to self in public, hoarding food |
| [4] | marked impairment in personal hygiene or grooming |
| [5] | blunted or inappropriate affect |
| [6] | digressive, vague, overelaborate, or circumstantial speech, or poverty of speech, or poverty of content of speech |
| [7] | odd beliefs or magical thinking, influencing behavior and inconsistent with cultural norms, e.g., superstitiousness, belief in clarovoyance, telepathy, "sixthe sense," "others can feel my feelings," overvalued ideas, ideas of reference |
| [8] | unusual perceptual experiences,e.g., recurrent illusions, sensing the presence of a force or person not actually present |
| [9] | marked lack of initiative, interests, or energy |
So here’s Yung and McGorry’s 1996 version:
| Monitoring and Care of Young People at Incipient Risk of Psychosis by Alison Yung, Patrick D. McGorry, Colleen A. McFarlane, Henry J. Jackson, George C. Patton, and Arun Rakkar Schizophrenia Bulletin 1996 22:283-303. |
|
| In 1994 we set up a specialized outpatient service to monitor and care for young people thought to be at high risk for psychosis. The specific inclusion criteria for the clinic, based on the above considerations, were intended to minimize false positives so the young people most at risk could be served. Targeted patients belonged to one of three groups, and ranged in age from 16 to 30 years. | |
| Group 1 consisted of those with a combination of trait risk factors and state risk factors, that is, a first- or second-degree relative with a history of any psychotic disorder or a schizotypal personality disorder, both as defined by DSM-III-R, combined with a change in mental state or functioning indicating development of a probable prodromal state as defined by the presence of two or more of the nine criteria for DSM- III-R schizophrenic prodrome. Although problems in using this DSM-III-R definition of prodrome were recognized, no other operationalized criteria for this phase were available | |
| Group 2 consisted of those who had developed attenuated or subthreshold psychotic symptoms, that is, who had one or more of the positive prodromal features from the DSM-III-R criteria for schizophrenia prodrome: markedly peculiar behavior; digressive, vague, overelaborate, or metaphorical speech; odd or bizarre ideation or magical thinking; or unusual perceptual experiences. | |
| Group 3 consisted of young people with a history of fleeting psychotic experiences that spontaneously resolved (called brief limited intermittent psychotic symptoms, or BLIP’S) within 1 week. The exclusion criteria were the presence of a known organic brain disorder or a history of previous psychosis lasting longer than 1 week (treated or untreated). | |
| Having defined the inclusion and exclusion criteria for the clinic, we then faced the issues of how to identify these high-risk individuals in the community and how to deliver appropriate clinical services to them. | |
There’s something of an paradox in these criteria. Back in 1980 when the DSM-III was introduced, there was a feeling that psychiatrists, particularly American psychiatrists, were too quick to diagnose Schizophrenia. The concerns at the time were that the diagnosis of Bipolar Disorder was not being adequately considered and there was the concern of stigmatizing patients by the diagnosis. So to diagnose Schizophrenia, one needed evidence of six months of continuous signs of the disturbance. That six months included at least one week of active psychosis, and the Prodromal or Residual Symptoms which we took to mean the continuous signs of the disturbance they were referring to. In addition, the DSM-III added the Schizotypal Personality to define those people who were ‘Schizophrenic-like,’ but never developed a full blown psychosis.
The paradox? Dr. McGorry’s group was essentially undoing the changes in the DSM-III. His criteria took us back to where we were before the coming of the DSM-III, as his ultra high risk group were close to the same people that Spitzer’s DSM-III had excluded in their revision. In an earlier day [pre-1980], they would probably have been diagnosed as having Schizophrenia or Incipient Schizophrenia. I guess "what goes around, comes around" after all.
Flashing forward a decade, there was a large NIMH funded collaborative study [North American Prodrome Longitudinal Study] designed to quantify outcome. It’s a difficult study to follow because there was some variability in a variety of parameter at different study sites [the full text is on-line if you’re interested in those details].
Validity of the prodromal risk syndrome for first psychosis:
findings from the North American Prodrome Longitudinal Study
by Woods SW, Addington J, Cadenhead KS, Cannon TD, Cornblatt BA, Heinssen R, Perkins DO, Seidman LJ, Tsuang MT, Walker EF, McGlashan TH.
Schizophrenia Bulletin. 2009 35(5):894-908.
[full text on-Line]
Treatment and prevention studies over the past decade have enrolled patients believed to be at risk for future psychosis. These patients were considered at risk for psychosis by virtue of meeting research criteria derived from retrospective accounts of the psychosis prodrome. This study evaluated the diagnostic validity of the prospective "prodromal risk syndrome" construct. Patients assessed by the Structured Interview for Prodromal Syndromes as meeting criteria of prodromal syndromes (n = 377) from the North American Prodrome Longitudinal Study were compared with normal comparison (NC, n = 196), help-seeking comparison (HSC, n = 198), familial high-risk (FHR, n = 40), and schizotypal personality disorder (SPD, n = 49) groups. Comparisons were made on variables from cross-sectional demographic, symptom, functional, comorbid diagnostic, and family history domains of assessment as well as on follow-up outcome. Prodromal risk syndrome patients as a group were robustly distinguished from NC subjects across all domains and distinguished from HSC subjects and from FHR subjects on most measures in many of these domains. Adolescent and young adult SPD patients, while distinct from prodromal patients on definitional grounds, were similar to prodromals on multiple measures, consistent with SPD in young patients possibly being an independent risk syndrome for psychosis. The strong evidence of diagnostic validity for the prodromal risk syndrome for first psychosis raises the question of its evaluation for inclusion in Diagnostic and Statistical Manual of Mental Disorders (Fifth Edition).
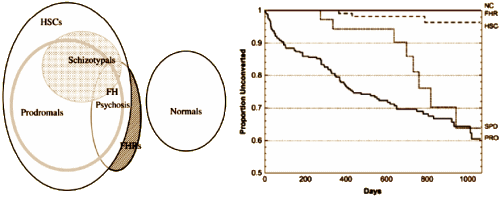
| NC | Normal Comparison Subjects | SPD | Schizotypal Personality Disorder |
| HSC | Help Seeking Comparison Subjects |
FH | Family History |
| PRO | Prodromals | FHR | Family History – not referred |
Because they made their overlapping categories mutually exclusive in the data analysis, here’s a recolored version of what the graph means in hopes of clarity:
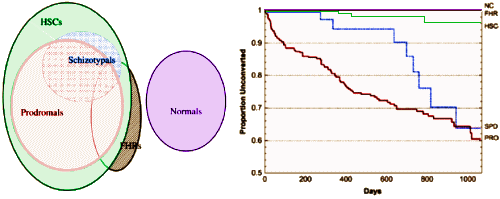
They used the SIPS [Structured Interview for Prodromal Syndromes full text on-line] to evaluate the prodromal state. In spite of some of the confusing internals, I thought this was a fairly decent study. They used a standardized instrument, and found that they could identify a prodromal cohort that went on to develop outright psychosis in over a third of the patients over a three year follow-up. I find that impressive. I would still see this as a research finding, because its clinical ramifications remain unclear. But it adds a solidity to McGorry’s research direction that his own data seems to lack. I think it’s kind of humorous that it is leading us back to a pre-DSM-III view of things [but I never much liked the DSM-III the first time around].
Now we arrive at my reason for reviewing all of this stuff. Here’s what the DSM-5 group has posted as the proposed criteria for an Attenuated Psychosis Syndrome:
| Attenuated Psychosis Syndrome |
|||
| The work group is recommending that this be included in DSM-5 but is still examining the evidence as to whether inclusion is merited in the main manual or in an Appendix for Further Research. As such, the work group strongly encourages feedback regarding this disorder. |
|||
| All six of the following: | |||
| [a] | Characteristic symptoms: at least one of the following in attenuated form with intact reality testing, but of sufficient severity and/or frequency that it is not discounted or ignored; | ||
| [i] | delusions | ||
| [ii] | hallucinations | ||
| [iii] | disorganized speech | ||
| [b] | Frequency/Currency: symptoms meeting criterion [a] must be present in the past month and occur at an average frequency of at least once per week in past month | ||
| [c] | Progression: symptoms meeting criterion [a] must have begun in or significantly worsened in the past year; | ||
| [d] | Distress/Disability/Treatment Seeking: symptoms meeting criterion [a] are sufficiently distressing and disabling to the patient and/or parent/guardian to lead them to seek help | ||
| [e] | Symptoms meeting criterion [a] are not better explained by any DSM-5 diagnosis, including substance-related disorder. | ||
| [f] | Clinical criteria for any DSM-V psychotic disorder have never been met | ||
On the web-page along with these criteria they have a rationale and a severity scale [unexplained]. I hope there’s a more elaborate version out there somewhere, but I haven’t been able to find it. Dr. Woods of the NAPLS study [above] and colleagues published a supporting article in November last year in the Schizophrenia Bulletin. Two of the Workgroup members wrote a supporting commentary in the May issue of the American Journal of Psychiatry, but the criteria are no more elaborate than what you read above.
I may think all of this effort to take us back to where we started is kind of ironic, but I don’t think this is a light topic. There’s a serious research effort underway to clarify the lead-in to the major mental illness that afflicts mankind. That’s a really big deal – long overdue. I’ve had plenty to say along with others cautioning patience until we know what we’re doing and what to do with what we’re learning. But I find these DSM-5 proposed criteria not only weak, but counterproductive, independent of whether the diagnosis ought to be there or not. They might as well just say "kind of crazy" and leave it at that – maybe add "for a while."
Whether you like the DSMs and the premises on which they rest or not, they’re what we have and they are relied on throughout the realm. It would be the height of naiveté to ignore how they’ve been used in the past – as a rationalization to prescribe medicine whether it makes scientific sense or not. "kind of crazy … for a while" isn’t a reason to make a diagnosis or medicate anybody, but if that makes it into the DSM-5, that’s exactly what will happen. Worse than that, it emphasizes the symptoms of Schizophrenia known as the positive symptoms, the noisy things, the things that impress novices when they first encounter this illness. They leave out the more subtle deteriorations in function present in the Prodromal or Residual Symptoms and the Structured Interview for Prodromal Syndromes – things many [of us] think are closer to the heart of Schizophrenia than the flamboyant symptoms. It’s possible that Schizophrenia as we know it [psychosis] is something that only happens in a percentage of vulnerable people, and this version of the criteria potentially eliminates an important segment of the afflicted that we need to know about long term.
Sorry, the comment form is closed at this time.