|
inertia [ɪnˈɜËʃə,-ʃɪə]
|
||
| — noun | ||
| 1. | the state of being inert; disinclination to move or act | |
| 2. |
the tendency of a body to preserve its state of rest or uniform motion unless acted upon by an external force
|
|
Inertia isn’t just a property of physical bodies. It’s applicable as a concept in a wide range of circumstances. Things in place tend to stay as they are. There are plenty of psychological examples: a substance use that self perpetuates as an addiction; a character trait that endures no matter how maladaptive; a child who ‘takes things’ who grows up to be a thief. Things that repeat or endure are the bedrock of our personae – sometimes the essential structures that support our growth, but at other times, the mechanism of our downfall. In a psychotherapy, it’s not terribly hard to identify what repetitive pattern of living is causing the patient’s discordant life. The hard part is figuring out how to change the pattern – to interrupt the inertia. And when I look back over the medical errors I’ve seen, mine and others, they’re almost always the same – categorical errors. They’re situations where the initial diagnostic category was wrongly chosen and by the time that became clear, it was too late. An anxiety attack that turned out to be a pulmonary embolus; a ruptured retroflexed appendix that eroded through the diaphragm or a ruptured esophagus both presenting as pneumonia; a hysteria that was, in fact, a brain tumor; an alcoholic whose D.T.s were really a symptom of fungal meningitis. Once the wrong categorical diagnosis is made, that initial mistake has an an inertia as strong as that of a resting boulder or an avalanche – a powerful resistance to change.
Primary Affective Disorders.
Depression.
—For a diagnosis of depression, A through C are required.A. Dysphoric mood characterized by symptoms such as the following: depressed, sad, blue, despondent, hopeless, "down in the dumps," irritable, fearful, worried, or discouraged.B. At least five of the following criteria are required for "definite" depression; four are required for "probable" depression.
—For a diagnosis of mania, A through C are required.A. Euphoria or irritability.B. At least three of the following symptom categories must also be present.
…we have made no effort to subclassify these illnesses. [For example, we have presented criteria to define primary affective disorders, unipolar type, without suggestions for further subdivision into forms of early and late onset, psychotic or nonpsychotic forms, agitated or retarded forms, and so forth. It is clear that primary affective disorder, unipolar type, is a reasonable major classification. The data to support its subclassification are still tentative.] We and other investigators will continue to work toward modification and subclassification. What we now present is our synthesis of existing information, a synthesis based on data rather than opinion or tradition. We hope that such a presentation will help to promote useful communication among investigators.
I’m not trying to be cryptic here and I hope I’m not being trivial, but I’m playing with the hypothesis that it’s possible that the unitary class, Major Depressive Disorder, was not rooted in either some scientific idea or theoretical position, but was rather just a way of thinking about classification in those early days that got carried along by inertia – something that came to have a meaning well beyond its meaningless or perhaps grammatical origins. It sure developed a massive meaning when the new antidepressants came along because it offered the clinical trial world a huge, unified, diagnostic cohort for testing the cascades of SSRIs that came from the pharmaceutical industry – a ready-made market extraordinaire. But I’m wondering if its beginning was mere convenience.
In Dr. Spitzer’s first article about reliability in 1974, he did put all the older depressive syndromes under one heading after the style of Feighner – Affective Disorders:
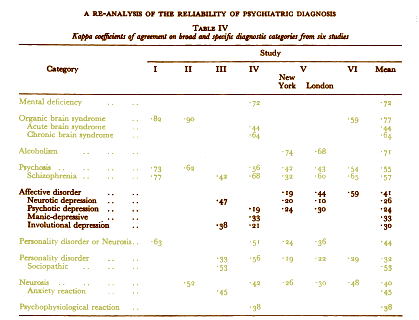
[recolored for emphasis]

[reformatted to fit]
fyi
From psychobabble to biobabble?
http://www.commonwealmagazine.org/blog/?p=19121
“If psychiatrists’ inability to agree among themselves on a diagnosis threatened to make them a laughing stock in the 1970s, the relabelling of a host of ordinary life events as psychiatric pathology now seems to promise more of the same”
it’s ironic that you’re raising questions in 2012 that should have been asked all along, throughout the last 40 years. It doesn’t take a rocket scientist or master clinician (or maybe it does?) to recognize that there are “varieties” or “subclasses” of depression. Nine symptoms does not a person make.
Anyone who thinks major depression is a “unitary diagnosis” either fails to listen to his/her patients, takes the DSM as Gospel, or is running a clinical trial.
Interestingly, Robert Spitzer coauthored an article in the AJP in 2010 advocating the designation of melancholia as a distinct disorder in DSM-5:
http://ajp.psychiatryonline.org/article.aspx?articleid=102363&journalid=13
His ability to acknowledge past mistakes is admirable.
Gad
Thanks for the link.
Yes, thanks, Gad, and it sure does seem to support what Mickey has been saying all along. Wonder how many people with melancholia could have been helped if their condition hadn’t been so mired down in MDD? Wonder what treatments could have been developed?
Aside from a whole host of bodily imbalances like iron deficiency, B-12 deficiency, thyroid problems, and sleeping problems; their are a host of ways to feel down and defeated that can be called “depression” but are not particularly endogenous. Feelings of grief, helplessness, hopelessness and defeat can be perfectly rational feelings to have in the face of seemingly unmanageable adversity and/or loss in our reductive atomized society.
Life can be really hard sometimes. The fact that our culture’s view of “mental health” often serves business to the detriment of self, family, friends, and community has led to individuals being expected to behave and emote in unnatural ways in the face of abuse, neglect, and exploitation. We are taught to internalize the blame and make excuses for the abusive and neglectful.
Victims see mental health professionals. Predators don’t. The whole mental health community is becoming increasingly predatory, is blaming a lot of victims and is heaping dehumanizing abuse on top of dehumanizing abuse.
I’m not saying that there is no such thing as mental illness, but that there isn’t so much mental illness that everyone who is feeling down and overwhelmed needs to be labeled with an endogenous mental illness and treated with drugs for life. Treating normal suffering and pain as a mental illness is dehumanizing.
Gad Meyer: Thanks. If I remember correctly, this article was responded to by a DSM-5 committee member and the proposed classification was given the bum’s rush. I think Dr. Carroll was involved in the correspondence but I really can’t be certain.
That’s it, precisely, Wiley.
Yes. See Kocsis JH, PubMed ID:21131414 and our reply in the same December 2010 issue of American Journal of Psychiatry. I am uncertain whether Dr. Kocsis was a task force member for DSM-5. Basically, we received no substantive response from the DSM-5 people. They simply failed to engage with this international group of dissenters.
Steve Moffic describes customers for psychiatry as pathetic losers in this MadinAmerica post, part of a speech he gave to the APA in May http://www.madinamerica.com/2012/05/human-rights-and-managed-care-part-5-conclusion/ .
I dunno. I never had a problem with the Depressive Neurosis diagnosis… it seems to fit much of everyday clinical experience. The loss may be external (a loved object) or “internal”– like a loss of self-esteem. Why is this such a problem for “scientific” psychiatry?
It
wasn’tisn’t…Hi, unscientific person here – but one with an interest in things psychiatric as I am a ‘consumer’ of mental health services, and I have a family member who’s been going through the revolving door for a couple of decades. I agree with Wiley – and aek. Sometimes, Life Just Really – Really – Sucks. I agree that the ‘institution’ of psychiatry needs to come around to the (gasp) bold concept of taking more of a “support and care” approach, and less of a authoritarian, drug oriented stance. I get that there are new drugs out there, and that they may, indeed, help folks get through the day – I even take a couple. That being said, while they have helped, they are no substitute for Taking The Time – to find out what is really going on w/ your patients, and what you can do to help, in a more wholistic way to address issues that may not be completely “psychiatric,” but which may impact your patient to a degree that makes them depressed (job loss, financial issues, etc.). Some people really just want to be Heard – and validated (I hate words like that, but whatever). Not saying you all need to become social workers, but just that you need to become more aware of your whole patients. Yeah, I know. That involves time, which implicates Money. I’m not one of those “all psychiatry is bad” people, I’m one of those “Some psychiatry is Just Common Sense, a listening ear, an open heart and a helping hand kinda person. This kind of change will only happen one shrink at a time, through education, word of mouth (or blog), before it’s the ‘norm,’ if it ever could be, given the financial and industrial forces behind modern day psychiatry.