Examining the Comorbidity Between Attention Deficit Hyperactivity Disorder and Bipolar I Disorder: A Meta-Analysis of Family Genetic Studies
by Stephen V. Faraone, Ph.D.; Joseph Biederman, M.D.; Janet Wozniak, M.D.
American Journal of Psychiatry. 2012 169:1256-1266.
Objective The existence of comorbidity between attention deficit hyperactivity disorder [ADHD] and bipolar I disorder has been documented in clinical and epidemiological studies, in studies of children and adults, and in diagnosed ADHD and bipolar I patient samples. Yet questions remain about the validity of diagnosing bipolar I disorder in ADHD youth. The authors aim to clarify these issues by reviewing family genetic studies of ADHD and bipolar I disorder.Method The authors applied random-effects meta-analysis to family genetic studies of ADHD and bipolar I disorder. Twenty bipolar proband studies provided 37 estimates of the prevalence of ADHD in 4,301 relatives of bipolar probands and 1,937 relatives of comparison probands. Seven ADHD proband studies provided 12 estimates of the prevalence of bipolar I disorder in 1,877 relatives of ADHD probands and 1,601 relatives of comparison probands.Results These studies found a significantly higher prevalence of ADHD among relatives of bipolar probands and a significantly higher prevalence of bipolar I disorder among relatives of ADHD probands. These results could not be accounted for by publication biases, unusual results from any one observation, sample characteristics, or study design features. The authors found no evidence of heterogeneity in the ADHD or bipolar family studies.Conclusions The results suggest that ADHD plus bipolar comorbidity cannot be accounted for by misdiagnoses, but additional research is needed to rule out artifactual sources of comorbidity. More research is also needed to determine whether comorbidity of ADHD and bipolar I disorder constitutes a familial subtype distinct from its constituent disorders, which if confirmed would have implications for diagnostic nosology and genetic studies.
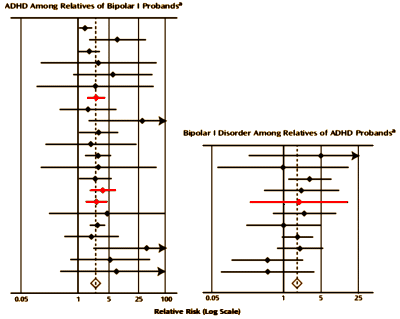
[the studies in red had bipolar children as probands (left) or targets (right)]
As we know, Dr. Biederman’s Conflict of Interest troubles and his subsequent censure by Harvard put a damper on "Biedermania" or the "Bipolar Child craze." When Senator Grassley began to investigate conflicts of interest and exploring the relationship between academic psychiatry and industry, Dr. Biederman was one of the central figures in the story. He had a million dollars worth of unreported income, J&J had funded a Center for him, and he had repaid by signing on to an old rewritten study proposing that Risperdal was effective for affective symptoms eg Bipolar Kids. Down, but not defeated, the MGH Group returns with this meta-analysis of the association between ADHD and Bipolar I Disorder. Dr. Biederman was the ADHD Guru who turned his attention to Bipolar Disorder in 1991 with this study:
Evidence of familial association between attention deficit disorder and major affective disorders
by Biederman J, Faraone SV, Keenan K, and Tsuang MT
Archives of General Psychiatry. 1991 48(7):633-42.
With the use of family study methods and assessments by "blinded" raters, we tested hypotheses about patterns of familial association between DSM-III attention deficit disorder (ADD) and affective disorders (AFFs) among first-degree relatives of clinically referred children and adolescents with ADD (73 probands, 264 relatives) and normal controls (26 probands, 92 relatives). Among the 73 ADD probands, 24 (33%) met criteria for AFFs (major depression, n = 15 [21%]; bipolar disorder, n = 8 [11%]; and dysthymia, n = 1 [1%]). After stratification of the ADD sample into those with AFFs (ADD + AFF) and those without AFF (ADD), familial risk analyses revealed the following:
Over time, his group developed the idea that Childhood Bipolar Disorder was much more prevalent than had previously been thought and that the symptoms were different from its adult counterpart – non-episodic irritability [bipolar kids: biedermania and super angry/grouchy/cranky irritability…]. As we all know, the diagnosis became a fad [maybe even a bit of an industry]:

Dr. Biederman and friends have lived in the eye of the storm on the issue of the over-medication of kids – ADD and Bipolar Disorder. The super angry, grouchy, cranky, irritable kids are the ones people want to medicate with the atypical antipsychotics to control their behavior. Labeling them "Bipolar" legitimizes the drug use, and many people think it is only that – an excuse to medicate disruptive kids [many of them foster kids]. Others think treatment of ADD is really "tuning up yuppie kids." And besides this recent article [above] looking like his way of trying to say, "See, I was right," it brings up several other aspects of psychiatric diagnosis in the post DSM-III era.
-
Comorbidity: It became a buzz-word like evidence-based-medicine, a sign you were on-board. literally, it means two [plus] Disorders at the same time, but is often used to imply that Disorders ‘run together" as in are related to each other in some way. It can be used as an excuse like when the poor DSM-5 reliability for MDD and GAD are explained as "too many comorbidities" as if that’s a meaningful explanation.
-
Soft Genetics: This is a study of the rate of ADHD in first-degree relatives of Bipolar I patients and vice versa. In psychiatry, we don’t have much in the way core Mendelian genetics. We have statistical family associations or risk factors like the ones reviewed in this study. ADD "runs with" Bipolar Disorder. It’s just the way it is – and it makes for endless speculations. Are ADD and Bipolar Disorders separate entities? comorbid? genetically carried cousins? different manifestations of the same thing? separate from each other and yet a third syndrome with symptoms of both? These are questions often discussed but rarely resolved.
-
"Bipolar": After the DSM-III, the diagnosis of Bipolar Disorder took off. With the DSM-IV it became Bipolar I and Bipolar II. With the COBY and other studies, there was Bipolar NOS. So things have gotten increasingly confusing. So Bipolar Disorder overflowed the boundaries of its humble Manic-Depressive origins before it metastasized to childhood under Dr. Biederman who redefined the syndrome in kids with neither periodicity nor "poles."
-
Diagnosis by "Symptom List": The descriptive diagnoses of the DSM-III may have moved psychologizing out of the system, but they weren’t without some confusion of their own. In the past, we spoke of Manic Depressive Illness as a disease entity with reasonably defined borders. Since then, those borders have become fuzzier and that is nowhere more apparent than in Dr. Biederman’s extension into childhood. But it’s also clear in the rural clinic where I volunteer and frequently hear patients say something like, "I’ve been told I’m Bipolar" – and have the pill bottles to prove it. As I said above, Manic Depressive Illness, the disease, has grown geometrically as the Bipolar Disorders. The clinic patients are people with unhappy lives, difficult circumstances, all sorts of other chronic problems. A handful actually have Manic Depressive Illness. But they have chronic symptoms, and that seems to be what lead to the label [and the meds]. I personally think it’s like "chemical imbalance," it gives their dysphoria a concrete explanation and the medication is validating [just the musings of an old shrink]. But diagnostic blurring of this type is common in modern times [symptoms = disorder = disease].
So back to the latest et al + Biederman in the AJP. The forest plots up top are problematic because there’s a lot of variability in the methodology of these studies [varying probands and targets]. But looking through them, I think they more or less show what this article says they show, a soft but real familial link between ADHD and Bipolar Disorder [going both ways]. What I was looking for were studies where the proband and/or target were Bipolar Children, since the obvious question is about his rewriting the diagnostic criteria. There were a few such studies from his MGH group and one from Geller et al. They cover this point in the paper:
in Results: Most studies of bipolar I probands (Table 1) ascertained parents with bipolar I disorder and reported the prevalence of ADHD in their offspring. The only exceptions were the Geller et al. and Massachusetts General Hospital child studies, which ascertained pediatric bipolar I probands and assessed the prevalence of ADHD in parents and siblings. Most studies of ADHD probands (Table 2) ascertained child probands and reported the prevalence of bipolar I disorder in siblings or parents. The only exception was the Massachusetts General Hospital adult ADHD study, which ascertained adults with ADHD and evaluated bipolar I disorder in offspring, siblings, and parents…
in Discussion: Regarding misdiagnosis, the samples diagnosed by the Massachusetts General Hospital group (data collected by the authors of this article) have been described as deviating from “classic” presentations of bipolar I disorder by allowing “severe, nonepisodic irritability” to qualify for the mood criterion… However, despite these concerns, if we exclude the Massachusetts General Hospital studies (or any other research group) from our meta-analyses, the estimated relative risks do not change and remain significant. Moreover, as Figures 2 and 3 show, the estimates of relative risk and confidence intervals from the Massachusetts General Hospital child proband studies are clearly consistent with the work of Geller et al., which is considered a more conservative approach to the diagnosis of pediatric bipolar I disorder.
Dr. Biederman is swimming against a heavy stream of criticism of the Bipolar Child diagnosis and charges of legitimizing the use of dangerous drugs for behavior control in difficult, disruptive children. A whole DSM-5 category, disruptive mood dysregulation disorder [DMDD], was created to undermine the effect of his claims. So in this article, he’s pretty careful to only discuss certain criticisms. He concludes:
Despite these limitations, our meta-analyses provide substantial evidence for a greater prevalence of ADHD among relatives of bipolar I probands and a significantly greater prevalence of bipolar I disorder among relatives of ADHD probands. These results could not be accounted for by publication biases, unusual results from any one observation, sample characteristics, or study design features. Our results suggest that ADHD and bipolar I comorbidity cannot be accounted for by misdiagnoses, but further work is needed to rule out artifactual sources of comorbidity.
I am certainly no fan of using antipsychotics in children and am a Doubting Thomas that the epidemic of Bipolar Children over the last decade is truly Manic Depressive Illness. The only proof will be longitudinal studies showing these kids become Manic Depressive Adults and they just aren’t yet definitive. My own skepticism comes in part from having seen a number of adult Manic Depressive people along the way, but never with a history of a super angry/grouchy/cranky irritable childhood. But I must add that I spent several days, on and off, looking at his references and rereading through his article, and I thought he played it straight. The article doesn’t legitimize his diagnostic criteria for childhood Bipolar Disorder, but he doesn’t claim it does. It does support that ADD and Bipolar Illness "run together" in families, affirming his claim of twenty years ago. And in a limited way, he showed that his results are mainstream rather than exceptions…
ADHD and bipolar disorder: Two vague diagnoses with shifting boundaries according to the politics and profits of the times.
Could it be the so-called association between the two indicates only that, in troubled populations, the diagnosticians give some bipolar diagnoses and others ADHD? (Wandering diagnoses amply demonstrated in DSM-5 field trials.)
If all the other major diagnoses were thrown into the pot, bi-directional relationships could be shown between any two.
To me, this indicates nothing predictable about “psychopathology” but the vagaries of psychiatric diagnosis.
And… naming is not explaining…