As a beginning psychiatrist, I read Eugen Bleuler’s 1911 description of the premorbid personalities of patients who went on to develop Schizophrenia. He acknowledged that although the personality type [Schizoid Personality] is very often described in the history of Schizophrenic patients, there are many people of the described type that do not develop Schizophrenia. I believed what I read and have seen that phenomenon play out in my own experience. I described such a case starting here. Drs. Patrick McGorry and Alison Yung in Australia took the logical step of trying to identify people who would develop the illness in advance. There were studies around the world with various criteria to identify the at risk population, and the early results suggested a 30+% conversion rate – identified patients who went on to became psychotic.
This line of thinking became more widely known when the DSM-5 Task Force proposed the Attenuated Psychosis Syndrome for inclusion as a new diagnosis. Dr. Allen Frances and many others opposed this move based on the preliminary nature of the research and fears that it would lead to unnecessary medication of patients. After a lot of tooth gnashing, it didn’t make it into the manual, and there were some disappointing follow up studies with much lower conversion rates [it just didn’t work…]. So it was a front page story that had its moment on the stage, then slid into the night. While I agreed that the Task Force was acting prematurely and that the danger of over-medication was very real, I hoped that the idea could be refined. Schizophrenia can be a devastating illness, and the idea that it might be detected before a psychotic break could well lead to safe preventive strategies.
by Nelson B, Yuen HP, Wood SJ, Lin A, Spiliotacopoulos D, Bruxner A, Broussard C, Simmons M, Foley DL, Brewer WJ, Francey SM, Amminger GP, Thompson A, McGorry PD, Yung AR.JAMA Psychiatry. 2013 1;70[8]:793-802.
IMPORTANCE The ultra high-risk [UHR] criteria were introduced to prospectively identify patients at high risk of psychotic disorder. Although the short-term outcome of UHR patients has been well researched, the long-term outcome is not known.OBJECTIVE To assess the rate and baseline predictors of transition to psychotic disorder in UHR patients up to 15 years after study entry.DESIGN Follow-up study of a cohort of UHR patients recruited to participate in research studies between 1993 and 2006.SETTING The Personal Assessment and Crisis Evaluation [PACE] clinic, a specialized service for UHR patients in Melbourne, Australia. PARTICIPANTS Four hundred sixteen UHR patients previously seen at the PACE clinic.MAIN OUTCOMES AND MEASURES Transition to psychotic disorder, as measured using the Comprehensive Assessment of At-Risk Mental States, Brief Psychiatric Rating Scale/Comprehensive Assessment of Symptoms and History, or state public mental health records.RESULTS During the time to follow-up [2.4-14.9 years after presentation], 114 of the 416 participants were known to have developed a psychotic disorder. The highest risk for transition was within the first 2 years of entry into the service, but individuals continued to be at risk up to 10 years after initial referral. The overall rate of transition was estimated to be 34.9% over a 10-year period [95% CI, 28.7%-40.6%]. Factors associated with transition included year of entry into the clinic, duration of symptoms before clinic entry, baseline functioning, negative symptoms, and disorders of thought content.CONCLUSIONS AND RELEVANCE The UHR patients are at long-term risk for psychotic disorder, with the highest risk in the first 2 years. Services should aim to follow up patients for at least this period, with the possibility to return for care after this time. Individuals with a long duration of symptoms and poor functioning at the time of referral may need closer monitoring. Interventions to improve functioning and detect help-seeking UHR patients earlier also may be indicated.
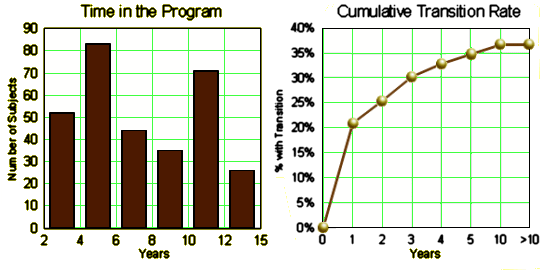
Clinical Implications The finding that transitions can occur up to at least 10 years after presentation but that risk is highest in the first 2 years indicates that the period of clinical care for UHR patients should be at least 2 years, with the possibility of reentry to services after this point if required. This need for ongoing clinical care is underlined by the substantial death rate in the sample [2.2%], mainly due to suicide. The association between UHR state and suicidality has been noted. Hutton et al found that 59% of UHR individuals presented with at leastmild suicidal ideation and 47% reported at least 1 suicide attempt before being accepted in an early intervention service. As indicated by the prediction analysis, patients with poor functioning and long duration of symptoms may need prolonged monitoring.It may be that different types of intervention are appropriate for patients with different durations of symptoms [ie, in an early or late phase of high-risk status].More benign treatments, such as supportive therapy32 or ω-3 fatty acids18 couldbe attemptedbeforeother,moreintensive, formsof treatment such as cognitive-behavior therapy. All of these treatments [supportive therapy, cognitive therapy and ω-3 fatty acids] address the UHR group’s clear need for care and are used for a range of mental health problems. Thus, they are low stigma and may be effective for several different conditions, including anxiety and depression. Antipsychotic medication is no more effective than more benign treatments and is currently not recommended for use in this population.
“The overall rate of transition was estimated to be 34.9% over a 10-year period [95% CI, 28.7%-40.6%]”
There’s a 5% chance (95% CI) the sample occured by chance, to show the transition rate was esitimated to happen just 1/3rd of the time. That’s pretty horrifying.
I wonder if the patients observed in the study were on any psychotropic drugs? Reminds me of a paper I read years ago,
“Antidepressant-associated mania and psychosis resulting in psychiatric admissions.”
http://www.ncbi.nlm.nih.gov/pubmed/?term=11235925
The authors found that “Forty-three (8.1%) of 533 patients were found to have been admitted owing to antidepressant-associated mania or psychosis.” I wonder how much of that 1/3rd in the ‘Long-term Follow-up’ study could be explained by psychotropic drug exposure, if so.
The last statement in the paper is nice.
———-
Not sure if I ever linked it before, but there was an excellent Canadian paper that determined the failure mechism of anti-psychotic drugs. In the synaptic cleft, feedback mechanisms which regulate specifically the D2 receptor fully overcome the effect of the drug though addition of new D2 receptors (attempting to compensate for the action of the drug’s blockade of these receptors).
(Blocking dopamine is the primary mechnism of action for all 3 generations of antipsychotics. Although the atypicals are categorized as ‘partial agonsits’, that aparently only meant they increase the release of dopamine while still blocking receptors all the same. The failure mechnism is still same.)
The result is a run-away process stemming from increased release of dopamine and too many additional receptors. The neurons increase in frequency (self-feeding) and basically no longer fire in proper synchronization.
The result is appearance of symptoms of ‘mental illness’ or specifically ‘psychosis’. The authors made note that raising the dose temporarily compensates for the increase in dopamine receptors. Of course, doing so just makes the problem worse. This is the eventual outcome of long term use.
“”Breakthrough” dopamine supersensitivity during ongoing antipsychotic treatment leads to treatment failure over time.”
http://www.ncbi.nlm.nih.gov/pubmed/?term=17360921
(Free Full Paper available)
Dr Nardo,
You are way off on this one. The previous commenter already raised some flaws.Let me give you a few others:
-even if the rate of so called “transition” were to be 80% in 2 years, and even giving you that schizophrenia is a “real” disease rather than an invented label and that the CI is 99%. Why should a particular individual be “suspect” of being a future schizophrenic, and thus a target of human rights abuses by the system even though he/she never might become one?
– there are more interesting correlates in the likelihood that a male black teenager in Detroit might end up in jail in 10 years or that a gay teenager in a big American city might get the HIV virus in 10 years. Should these two groups of people be dealt with preemptively?
Mickey, I a, very surprised reading that you seem to support the “Minority Report” model.
Mickey, thank you so much for posting this. and especially for highlighting the sentence about the relative lack of efficacy of antipsychotic drugs and the clear statement by McGorry’s group that such treatments are not recommended for this population. This is a welcome warning that is sadly lacking in so many “psychosis-risk syndrome” or “attenuated psychosis syndrome” studies.
Our natural, desperation-fueled impulse is to “do something” to help the patients and families, but there is no firm, uncontroversial evidence evidence from longitudinal studies that antipsychotic medication would halt, or even slow down, whatever pathophysiological processes (of which there may be hundreds in the body) that affect the brain to the point they would fit into our hydra-like heuristic that we call schizophrenia.
A century ago, the mental hygiene movement quickly pivoted from its original intention (to help people already ill and in asylums and state hospitals) and focused instead on a public health campaign of “prevention.” This led to a paranoid panic about our youth — who could tell how vast the number of latent or prepsychotic people were out there roaming the streets?
When I look at this from the perspective of the long arc of history, I see the contemporary push toward creating a DSM diagnostic category of “attenuated psychosis syndrome” as a replay of the frustration and admission of failure of a century ago: not much can be done for the poor souls already crushed by chronic psychosis, so let’s save the children and young adults instead.
The problem then, as now, is that our state of knowledge about (a) how to reliably identify and (b) treat such persons in everyday clinical practice is poor. Excellent studies such as this one reflect the universe of researchers, but the translation of such findings into messy everyday clinical practice would be premature. We have to learn to resist the impulse to intervene with medication until we know more. Allan Frances may have been right in claiming that including APS in DSM-5 would result in a “public health disaster.” The slightest subjective judgment by a physician that some young person had a few bizarre delusions or odd behaviors would reflexively result in treatment with antipsychotic medication. The fasle positive rate would be staggering.
I have been following the “high-risk” literature intensely for the past 30 years, in part because my dissertation supervisor, Prof. Erlenmeyer-Kimling of the NY Psychiatric Institute, was one of the pioneers of longitudinal studies of children at-risk for schizophrenia back in the 1960s. Markers such as attentional deficits, smooth-pursuit eye movement abnormalities, etc., were well-documented in those populations. From the perspective of science, these sorts of longitudinal studies are the way to go and promise the biggest pay-off in terms of fundamental knowledge about chronic psychotic disorders, prevention and treatment, so I am an enthusiast when it comes to this approach. The problems are many: the personal history of individuals is squahed into checklist bullet points on some scale, family context is inadequately ignored, etc. And, since the 1960s, the use of street drugs has been so rampant that these confounding factors are now downplayed or ignored by far too many schizophrenia researchers. And so on . . . .
As I tell my students,well-designed and executed research studies are a bit like trying to sip coffee with a fork — traces of something real are captured, but the structures of our instruments limit what we can sample from the stream of life. And remember, the structured “instruments” we use (rating scales, the statistical procedures and their often-forgotten underlying assumptions about distributions, etc., the starting assumptions about the defining characteristics of “psychosis” or “schizophrenia,” etc.), create their own artifical realities. On my worst days I see the mountains of published research studies (partcularly in the social sciences, and especially psychology) as a “house of cards.” On my fewer better days, I have hope.
Festina lente, I say.
Richard,
I’m a lay person, and sometimes both Mickey’s articles and the cogent comments that follow are a bit over my head. But, let me tell you, I certainly understand the last paragraph in your comment–and it is greatly APPRECIATED. Thanks.
…“Forty-three (8.1%) of 533 patients were found to have been admitted owing to antidepressant-associated mania or psychosis.”
Yes, TCR— rather than classifying this as an “unmasking” of bipolar disorder and creating “bipolar II”, this reaction should always be identified as a drug effect and studied as such. It’s a simple scientific thing to acknowledge the relationship and hold off on judging a drug reaction as an indicator of disease until there is sufficient evidence to declare that it “might” be evidence of an underlying bipolar disorder.
Since people who are taking antipsychotics have breakthrough psychoses, it’s best not to put entirely too much stock in medication as a prophylaxis.
The slightest subjective judgment by a physician that some young person had a few bizarre delusions or odd behaviors would reflexively result in treatment with antipsychotic medication. The false positive rate would be staggering.
http://forensicpsychologist.blogspot.com/2010/11/how-black-man-became-schizophrenic.html
… family context is inadequately ignored…
I call this the Have I mentioned that I lived with my mother? Effect.
…the use of street drugs has been so rampant that these confounding factors are now downplayed or ignored by far too many schizophrenia researchers.
My schizophrenic uncle did drugs in the sixties/seventies. It took four strong people to get him to the hospital (he was small enough to be a jockey), and some additional hospital staff to hold him down to give him thorazine. He was on PCP and was just as dangerous as anyone in the throes of violence on PCP. There is evidence that the risk of violence from psychotic people on certain drugs is the same as the risk for non-psychotic people on certain drugs— that includes alcohol.
I read an article in Harper’s once about prodromal symptoms in schizophrenics that talked about people learning to identify the very early stages of psychotic thought processes to help them contradict such thinking and seek the help of their choice.
And then there is the possibility that a psychotic episode may be a symptom of an underlying non-psychiatric state of bodily disorder:
http://blogs.scientificamerican.com/scicurious-brain/2013/01/30/scicurious-guest-writer-sleight-of-hand-sleight-of-mind-illusions-delusions-and-the-immune-system/
I should have said, “people identified or labeled as schizophrenic,” rather than “schizophrenics”.
The perversion of the “80-20” rule at its finest in corruption. This is yet another example of why the APA has an antisocial/sociopathic element in it, even if the driving force is ‘simply’ profit/money. Hey, corruption, be it drugs, money, power, sex, etc., can’t be rationalized as being more benign or less destructive just because a ‘cousin’ is worse.
Wow, psychopharmacology has come a long way. See those Gates of Hell, colleagues? Oh, and who is going to clean up that mess, all you silent and avoidant colleagues? Pathetic!
FYI
Mind
A Dry Pipeline for Psychiatric Drugs
Dr. Richard A. Friedman is a professor of clinical psychiatry at Weill Cornell Medical College.
http://www.nytimes.com/2013/08/20/health/a-dry-pipeline-for-psychiatric-drugs.html?hpw&_r=0
FYI more relevant to this post
From the President
August 15, 2013
Early Detection of Schizophrenia: The Time Is Now Jeffrey Lieberman, M.D.
”
From the President
August 15, 2013
DOI: 10.1176/appi.pn.2013.8b27
Early Detection of Schizophrenia: The Time Is Now
Jeffrey Lieberman, M.D.
Print
E-mail
Share
Reprints
Photo: Jeffrey Lieberman.
Medical research often takes a slow and unpredictable pace. The hours spent defining the question, setting up the experiment, and acquiring and then analyzing the data before getting to see the results makes for a long and arduous process. When you then add the time that it takes for new research findings to be translated into clinical practice, the rate of change in health care can be glacial. Psychiatry is certainly no exception to the seemingly snail’s pace of progress in health care.
But despite this pervasive pattern, research does periodically gain sufficient momentum to make inroads into clinical practice and move the field forward, as was the case with the introduction of antipsychotic and antidepressant drugs, lithium, community mental health, the development of time-limited forms of psychotherapy (for example, cognitive-behavioral therapy, interpersonal therapy, and dialectical behavior treatment) and cognitive remediation.
I believe that we are at another game-changing moment in psychiatry with the rise of the early detection and intervention strategy (EDIS).”
“…based on the experience and anticipated results of the NIMH’s ambitious Recovery After an Initial Schizophrenia Episode study, the Centers for Medicare and Medicaid Services and the Substance Abuse and Mental Health Services Administration are considering funding and supporting EDIS services and models of care.”
http://psychnews.psychiatryonline.org/newsarticle.aspx?articleID=1729380
@wiley
Thanks for the interesting links! There are so many medical conditions that can disrupt the nervous system and actually produce persistent psychosis. Vitamin defficencys (B-12/other B vitamins), CNS infections, some medications/psychotropic drugs, tyroid/hormone disturbances, etc.
Psychiatric diagnosis is just a mess my itself. Trying to predict that someone will go on to develop something worse seems impossible when diangosis itself (when they do) is so poor. It’s hard to imagine a patient labled with a psychiatric diangosis having received a diangostic test or medical evaluation for anything.
@ jamzo
So this is what everybody is talking about over at the APA, I guess.
“Recovery After an Initial Schizophrenia Episode (RAISE): A Research Project of the NIMH”
http://www.nimh.nih.gov/health/topics/schizophrenia/raise/index.shtml
One thing that always drove me nuts, the CATIE study had no placebo group. The replase rate increased by 50% (from 30% at start of study to 80% at end of 18 months). Where was the evidence the drugs were more cost effective at the end of 18 months then doing nothing?
The NIMH is now testing the cost effectivness of intervention, I’m sure, without a placebo group.
I have to ask, where does Lieberman get off refering to the toxic element Lithium as scientific progress? The drug came from some idiot injecting hamsters or something with the urine of Schizophrenics and realizing his PH ajustment with lithium sedated the animals. So he tested it on himself and then arbitrarily assuming it was safe after one dose, gave it to his Schizophrenia patients continously and declared Schizophrenia a “Lithium defficincy”. Eventualy Lithium lost it’s approval by the FDA for Schizophrenia, I wonder why. (I wish I had a citation for all that).
Lithium causes CNS dysfuction at low doses and sedation at high doses, interferes with the utilization of sodium which is elementally similiar to lithium and causes peoples thyroids and other organs to malfunction (including their brain, where neurons require sodium ions to fire).
Lithium’s drug labeling information carries the cyptic warning “Lithium should not be used in patients with Mental Illness”.
A psychiatrist-eye view of vitamin B12 deficiency:
http://www.nlm.nih.gov/medlineplus/news/fullstory_139225.html
Anemia Might Raise Dementia Risk, Study Suggests
“….
“We found a 60 percent increased risk of dementia with anemia. After controlling for other factors such as other medical illness, demographics, etcetera, the risk remained elevated 40 to 50 percent,” said lead study author Dr. Kristine Yaffe, a professor of psychiatry, neurology and epidemiology at the University of California, San Francisco.
….
“Because we studied this prospectively, we do think, as best we can tell, that anemia is causally related to dementia, but with observational studies one can never say for sure. But we did our best to exclude other explanations,” Yaffe said.
The job of red blood cells is to carry oxygen throughout the body. When you are anemic, less oxygen is delivered to brain cells, Yaffe explained. “We think the association is about low oxygen being carried to the brain,” she said.
….”
Excuse me? It doesn’t take a lot of Googling to find that B12 deficiency is related to anemia and a misdiagnosis of dementia. This has been known for many, many years.
The correct treatment is not psychiatric but to supplement vitamin B12!
Hey, Alto! I’ve been taking high doses of sublingual B-12 since I was diagnosed with a deficiency. I stopped taking after I tested with very high levels after the next physical. Then, I started slowly descending into what I thought was an MS relapse. Then I started taking the B-12 again. I’m not feeling any fatigue and very little brain fog. Yeah!
I knew I’d get diagnosed with depression if I saw a mental health professional for what turned out to be fatigue. Learning is wonderful.
“A crime is a deviation from generally recognized standards of behavior frequently caused by mental disorder. Can there be diseases, nervous disorders among certain people in a Communist society? Evidently yes. If that is so, then there will also be offences, which are characteristic of people with abnormal minds. Of those who might start calling for opposition to Communism on this basis, we can say that clearly their mental state is not normal.” Nikita Khrushchev Pravda on 24 May 1959
https://en.wikipedia.org/wiki/Political_abuse_of_psychiatry_in_the_Soviet_Union#Political_trend_toward_mass_abuse_onset
For those who followed Mickey’s link and re-read his blog piece on the phases of early psychosis, the terms for the early stages of psychosis (treme, apophany, anastrophe, apocalypse) came from the late 1950s work of German psychiatrist Klaus Conrad (1905-1961).
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2800156/pdf/sbp144.pdf
Like Bleuler’s 1911 book, pre-checklist psychiatry offered a literature with thick description that was, despite all its scientific limitations, very helpful in actual everyday clinical work.
O.K., now I’ve re-read it.
The descriptions of the states that were born of dialogue, study, reflection, and respectful relationships between patients and clinicians is refreshing. It seems that the “it”of bio-bio-bio psychiatry is doing its level best to dismiss the experiences as nothing more than glitches with which the patients who experience them don’t even have a relationship with them.