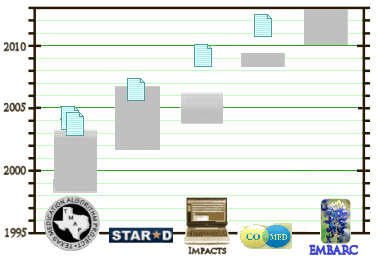
 As doctors and patients encountered the inconsistent performance of these drugs in their offices and clinics, they tried all those strategies mentioned above in non-responders [labeled as having treatment resistant depression] and anecdotal solutions abounded [along with the rise of poly·pharmacy, a former no-no]. That future history of the second age of psycho·pharmacology will undoubtedly have a figure like the one on the right showing what might be called the Texas Many-Step, a series of studies that attempted to systematize these anecdotal sequencing, combining, augmenting strategies as algorithms. The studies were publicly funded, expensive, and notoriously failed enterprises. TMAP, the opening gambit, was a drug company encouraged scam to get expensive drugs into the public sector – now defunct and still in the courts. The middle three were NIMH funded duds. And the final one is an ongoing NIMH study [AKA dud-in-training]. The history book chapter describing this period might be entitled squeezing blood from a turnip? I’ve chased off readers with my preoccupation with these studies, so I’ll skip the details [put any of them into search below if you need a refresher].
As doctors and patients encountered the inconsistent performance of these drugs in their offices and clinics, they tried all those strategies mentioned above in non-responders [labeled as having treatment resistant depression] and anecdotal solutions abounded [along with the rise of poly·pharmacy, a former no-no]. That future history of the second age of psycho·pharmacology will undoubtedly have a figure like the one on the right showing what might be called the Texas Many-Step, a series of studies that attempted to systematize these anecdotal sequencing, combining, augmenting strategies as algorithms. The studies were publicly funded, expensive, and notoriously failed enterprises. TMAP, the opening gambit, was a drug company encouraged scam to get expensive drugs into the public sector – now defunct and still in the courts. The middle three were NIMH funded duds. And the final one is an ongoing NIMH study [AKA dud-in-training]. The history book chapter describing this period might be entitled squeezing blood from a turnip? I’ve chased off readers with my preoccupation with these studies, so I’ll skip the details [put any of them into search below if you need a refresher].
by Stuart M Grieve, Mayuresh S Korgaonkar, Amit Etkin, Anthony Harris, Stephen H Koslow, Stephen Wisniewski, Alan F Schatzberg, Charles B Nemeroff, Evian Gordon, and Leanne M WilliamsTrials. 2013; 14: 224.
Background: Approximately 50% of patients with major depressive disorder [MDD] do not respond optimally to antidepressant treatments. Given this is a large proportion of the patient population, pretreatment tests that predict which patients will respond to which types of treatment could save time, money and patient burden. Brain imaging offers a means to identify treatment predictors that are grounded in the neurobiology of the treatment and the pathophysiology of MDD.Methods/Design: The international Study to Predict Optimized Treatment in Depression is a multi-center, parallel model, randomized clinical trial with an embedded imaging sub-study to identify such predictors. We focus on brain circuits implicated in major depressive disorder and its treatment. In the full trial, depressed participants are randomized to receive escitalopram, sertraline or venlafaxine-XR [open-label]. They are assessed using standardized multiple clinical, cognitive-emotional behavioral, electroencephalographic and genetic measures at baseline and at eight weeks post-treatment. Overall, 2,016 depressed participants [18 to 65 years old] will enter the study, of whom a target of 10% will be recruited into the brain imaging sub-study [approximately 67 participants in each treatment arm] and 67 controls. The imaging sub-study is conducted at the University of Sydney and at Stanford University. Structural studies include high-resolution three-dimensional T1-weighted, diffusion tensor and T2/Proton Density scans. Functional studies include standardized functional magnetic resonance imaging [MRI] with three cognitive tasks [auditory oddball, a continuous performance task, and Go-NoGo] and two emotion tasks [unmasked conscious and masked non-conscious emotion processing tasks]. After eight weeks of treatment, the functional MRI is repeated with the above tasks. We will establish the methods in the first 30 patients. Then we will identify predictors in the first half [n = 102], test the findings in the second half, and then extend the analyses to the total sample.
Acknowledgements: We acknowledge Brain Resource as the sponsor for the iSPOT-D study [NCT00693849]. Claire Day [Global Study Co-ordinator] is thanked for her pivotal role in making this study happen, and for her boundless enthusiasm and energy. We thank the iSPOT-D Executive Committee for their valuable input into this manuscript and into the study overall [Members: A John Rush [Chair], Lea Williams [Academic PI], Steve Koslow, AmitEtkin, Evian Gordon, Steve Koslow, Stephen R Wisniewski. We also thank those responsible for designing the iSPOT-D protocol [A. John Rush, Lea M Williams, Evian Gordon, Charles B Nemeroff, Alan F Schatzberg]. We gratefully acknowledge the editorial support of Jon Kilner, MS, MA [Pittsburgh, PA, USA]. SMG acknowledges the support of the Sydney University Medical Foundation. Dr Lavier Gomes, Ms Sheryl Foster and the Department of Radiology at Westmead are thanked for their substantial contributions to MRI data acquisition.
-
Churning:These studies produced a astounding number of articles. The hands-down winner of all times was STAR*D with well over a hundred, but the others were like this one – lots of intermediate articles. In spite of the voluminous ouptput, definitive reporting or formal compliance with clinical trial reporting was missing in action.
-
Design:
-
Ghost:Jon Kilmer, science fiction author and medical ghost writer, has been in the background for the long haul. I think these many articles make up the majority of his career as a medical writer.
-
Authors:Lead by A. John Rush and Madhukar Trivedi, a stable of other authors make up the cohort that has been the river that runs through all these studies, mixed and matched as the papers continued to pour into the literature – a who’s who of the PHARMA friendly psychiatric KOLs. Whether funded by the NIMH or by the Brain Resource group in Australia, you can count on familiar names – many familiar names. And they’re joined by even more KOLs in EMBARC and iSPOT – many listed in both projects
-
A Database [at last we reach the actual topic of this post]:Except for iSPOT, these were publicly funded projects that produced reams of data, and the grandaddy, STAR*D, made much at it’s outset of its creating a database for further study by all. This database has mainly been tapped by the original gaggle of authors, but a few others have waded in. iSPOT came with the Brain Resources Group making a similar offer, a vast database made available for mining by all. This was to be, in both cases, the dawn of data sharing – opening the vaults to the scientists of the world.
While none of these studies had anything directly to do with PHARMA, they all have everything to do with PHARMA, and a devoutly sought new industry – biological testing in psychiatry – encoded in the also becoming-passé topic, personalized medicine. But at least STAR*D and iSPOT advertised that the generated data would be available to all. With the front running issue now being data transparency and the pharmaceutical industry trying to get away with substituting data sharing while maintaining their former tight control and continuing to hold their cards close to the chest, these tired studies offer us some insight to the whole story of available data. How did the NIMH and Brain Resource handle the issue of the advertised data access? Are STAR*D and friends candidates for a RIAT team – abandoned studies in need of restoring? These are important right-now questions.
Authors: Stuart M Grieve, Mayuresh S Korgaonkar, Amit Etkin, Anthony Harris, Stephen H Koslow, Stephen Wisniewski, Alan F Schatzberg, Charles B Nemeroff, Evian Gordon, and Leanne M Williams.
Looks like the usual suspects, doesn’t it? The article in the journal Trials is like a press release before an IPO. Is NIMH pouring good money into this one, too?
TMAP is still used in Washington State. It’s an “evidence based practice” according to Jeffrey Thompson, the psychiatrist who is the medical director of Washington’s Medicaid program. The state actually hired John Chiles after TMAP was “discredited.” http://involuntarytransformation.blogspot.com/2012/10/washington-state-hired-architect-of.html#.UjYiC8Zwp48
I still see these posts by Mickey as “missing the forest for the trees”. The real issue is a flawed theory, namely, that something as complex as a human emotion can be cataloged as a “mental illness” with a simple solution: increasing neurotransmitter levels in the neuron synapses. It’s the whole notion of the “chemical imbalance” that has produced these travesties.
Same with his comments about trials. While no question there are abuses on the matter in other areas of medicine (most notably with respect to hiding side effects), the reality is that a drug cannot claim to be effective in lowering cholesterol levels unless, it really does. However, a psychiatric drug can claim to be as effective as it wants because it doesn’t change any measurable biological marker. Well, not really true. Neuroleptics have been shown to decrease brain tissue, but that is not something that I would call “efficacy” of the drug.
Psychiatrists like Dr Nardo or Allen Frances realize that their discipline is rotten, but instead of attacking it, they area attempting to psychiatricize the rest of medicine.
The problem of corrupt drug trials, and overmedication is overwhelmingly a problem with psychiatry. And the unbiased critical thinkers should ask themselves what’s in psychiatry that makes it such a great place for this type of fraudulent practices. The answer is not hard to see: psychiatry itself is a fraudulent endeavor.
Speaking of medicaid, I found something interesting in the NYTimes the other day.
“For weeks now, New Mexico has been in the midst of a sweeping criminal investigation into 15 of its largest mental health providers, suspected of defrauding Medicaid of $36 million over three years. ”
“Ms. McWilliams also cited a “suspicious business arrangement” between a group of providers, where it appeared the executives were shuffling Medicaid money away from their agencies to a corporation they had formed. ”
http://www.nytimes.com/2013/09/14/us/fraud-investigation-unsettles-mental-health-care-in-new-mexico.html?pagewanted=all
Aparently money was being stolen from medicaid though agressive overbilling, and then secretly funneled into a new corporation started by executives from the providers being investigated.
Finally a fraud investigation that doesn’t focus on drug sales. I wonder who this mysterious fraud-funded corporation is?
And to elaborate further on my idea. If one takes a look at the big scandals in Big Pharma, those associated with psychotropic drugs are of a very different nature from those outside psychiatry.
The biggest big pharma scandals that I can remember outside psychotropics are the thalidomide one (I wasn’t born when this happened but I heard horror stories growing up about it), the factor VIII one that killed tens of thousands of hemophiliacs and more recently Vioxx’s. In each of them, the scandal was that the drugs did treat a physiological symptom, only they also introduced secondary effects that were dangerous, even deadly in some cases. There was no question though about what they treated.
Most scandals associated with psychotropics are linked to Big Pharma promoting drugs for “off label” usage. Meaning, a big pharma company promoting the usage of a drug for a particular condition using bogus arguments. You have to wonder why big pharma cannot promote say Aspirin as an effective antibiotic. Or an antibiotic as an NSAID. The answer is obvious. However, with psychotropics it is possible to promote each of its drugs for almost anything. That is why instead of attacking Big Pharma, Mickey and Frances would do better attacking the big elephant in the room: psychiatry is a bogus medical specialty.
CannotSay2013,
I dunno if you saw apost I made much earlier. Take a look at this drug, specifically scroll down and see what the sole indications are.
http://dailymed.nlm.nih.gov/dailymed/lookup.cfm?setid=de55c133-eb08-4a35-91a2-5dc093027397
(this freely available database contains prescribing information/drug labeling information, and is maintained by the NIH for the FDA)
This is an antipsychotic drug tweaked and marketed for Acid Reflux.
Psychiatry is only the tip of the iceburg. Look closer and you’ll cringe. The problem actually isn’t so much with psychiatry as it is with fraud and data-manipulation, illegal marketing and fraud, kickbacks and bribes from the pharmaceuticaland medical device manufacturing industry. The degree of felony *convictions* against pharmaceutical companies each year is staggering.
Take a look at the American Medical Association, or what’s left of it. They recently elected a psychiatrist as their president, to represent all medical specilites in the US. The APA isn’t even unique for engaging in corruption and fraud.
If psychiatry didn’t exist, then psychologists would be prescribing drugs. They can already legally do this in two states, the APA ironically tries to fight this, but is losing.
In short, psychiatry is a philosophy, all the ‘science’ or ‘evidence based medicine’ bits and claims are industry paid for, and industry created. My gastroenterologist, when i asked him about a new medical device for heartburn told me “they come and they go, none work”. I asked about the drugs other then PPIs, and he told me simply “They kill people”.
This blog not the place to debate the scientific integrity of psychiatry, you’re preaching to the choir 🙂
Yet another site about this New Mexico issue claims the government has just shut down ALL clinics. Gotta love bureaucracy, blame all when trying to figure out who is being inappropriate as a minority.
And those who still think PPACA (ie Obamination Care) is going to do wonders for the country. “Wonders”, that is a loosely used term.
I “wonder” how many people will be irrevocably harmed by this legislation?
Frankly, Syria is an overt “Wag the Dog” exercise by the Democrats. Shame on all who have bought into this mentality, let’s have another war, who gives a —- about our citizens! But, the needs of the few have to screw the needs of the many, the mantra of Republocrats. Elections need to be won NOW!
Happy Fall.
TinCanRobot,
I don’t think I am preaching to the choir. While it might be true that you and I are probably on the same page, Dr Nardo shares Allen Frances’ view that psychiatry is a scientific discipline that helps people if “done right”. The amount of data, like the one showed in this post, providing evidence to the contrary doesn’t matter to them. It’s all about Big Pharma’s greed when the reality is that the reason none of these megastudies concluded anything useful is obvious. And for those that don’t see the “obvious part” here it is: since psychiatry is a fraudulent endeavor, each of those studies amounted to nothing more than an average over a pile of data generated by a zero mean white noise. The average of a large amount of data generated by a zero mean white noise is, well, zero. Which is why each of this studies was a failure. They were not testing anything scientific. For people like me, the problem is psychiatry. For somebody like Mickey, the problem is big pharma.
TinCanRobot,
And speaking of psychiatry’s true believers, here just popped one: Mr
Joel Hassman.
CannotSay2013
Please read the note in the comment box and follow it.
Mickey
I apologize to you Mickey and Joel.
However, you cannot square the fact that most of the issues you denounce in your blog, and rightly so, are rooted in psychiatry’s lack of scientific basis. You should have the courage to engage in a discussion about it.
CannotSay2013,
You may or may not have seen this portion of the blog’s history:
http://1boringoldman.com/index.php/2011/08/20/off-the-air/
http://1boringoldman.com/index.php/2011/08/22/about-comments/
From that post:
“And there are plenty of complaints about the field other that the ones I address – some valid and some not. This is not an open forum for that discussion. There are bloggers who do answer general questions or engage arguments, and others who use a blog as a form of social media like facebook or twitter. Those are all choices to make, but they’re not mine.”
There are some topics I feel passionately about, and put my best pitches out there, and that do not resonate with 1bom. Even just look at it as harm reduction if you’d like. We’re all better off with this blog than without.
Annonymous,
I hadn’t read those. I agree that we are all better off with this blog than without it. Mickey does a great job exposing a lot of useful information.
That said, those two postings are from 2 years ago. I would find it a bit strange that Dr Nardo has not “evolved” (to use a word that became a fad during last years’ presidential election) on his views about the validity of psychiatry, given all the things that he has talked about during the last 2 years. Even Allen Frances has been “evolving”. In his most recent writings he acknowledges having damaged individual people in his younger day (beyond his role as chairman of the DSM IV task force).
I would love to know if the things he has learned during this journey have affected his perception about the legitimacy of psychiatry. There are other psychiatrists who have traveled that road before, more prominently Peter Breggin or Colin A Ross.
And this is the last thing I will say about this matter (sorry for the numerous messages, but I truly miss an “edit” button).
The reason I am first and foremost interested in debunking psychiatry is because of the social effects of having been labelled “mentally ill”.
I am just interested in having my dignity back, a dignity that I lost the day I was labelled as “mentally ill”.
Because of that unscientific label, there are things that I am not legally allowed to do. And other things that, even if I were legally allowed to do, such as applying for jobs that require security clearances or say running for political office, I would be forced to agree to the dehumanizing psychiatric label imposed onto me. If you think that it doesn’t make a difference, just ask homosexuals the difference it made in their lives to have had their behavior been dropped from the DSM as “pathological”.
1 label dropped, 400+ left to go!
TinCanRobot -RE Medicaid fraud in New Mexico, I found this:
http://senatorfeldman.typepad.com/senator_dede_feldmans_blo/2013/07/fiddling-and-fighting-while-rome-burns-new-mexicos-crisis-in-behavioral-health.html
@ CannotSay2013
i’m sorry you suffered that. It’s increasingly common for patients to discover the degree of illegal acitvity surrounding psychatry, and the poor reliability of diagnosis. Many get very angry until they become better informed in how to approach the problem.
Patient discontent is growing, but so is criminal activity of the industry. It’s almost impossible to make the argument that psychiatry shouldn’t be a medcial specilaty and be taken seriously by anyone who doesn’t share that belief. Most people don’t have time or interest to reasearch psychiatry or the industry that makes psychiatric treatments. If they see a psychiatrist employed in hosptial, they ignore you.
For example, if you argue with a school teacher that ‘psychiatry isn’t a science’, she won’t stop referring childen who act up to the school’s psychiatrist for ‘adhd diangosis’. Certainly the school won’t listen either.
If you tell tell a teacher that Crystal meth is also approved for ADHD as ‘desoxyn’ simply because Amphetamine (aderall) was, and that simply because ritalin was, she might take pause. That’s about it though.
If you bring in news articles or court documents for felony convictions for illegal marketing of ADHD drugs, child deaths, the Congressional investigation of the APA by senator Grassley of congress over ‘Conflict of Interest’, and the disciplining by Harvard university of one Joseph Biederman for hiding millions of dollars in personal gifts from his pharmaceutical sponsors while creating the first ADHD trials, people will listen.
Once they see the criminal activity there’s little need to argue about the harm of of the APA’s embraced disorders and treatments. To top it all off, the ADHD drugs are shown not to work with the observations used for clincial trials after about 3 years continuous use. The marketers own ‘science’ can be used to expose them without challenging the integrity of that science.
It all only works when we make one specific narrow cirticsism, and don’t be overly broad. Psychaitry has 12 specilties, 2 approaches, more then a hundred drugs, medcial devices, and surgurys for treatment. Psychiatry treats everything from drug addiction and rape/torture/abuse/war victoms to those chronically psychotic, or suicide atrtempts.
The mental health system is made up of more then just psychiatry, we also have psychology, and countless bureaucrats.
Be as specific as possible, narrow arumgnets. There is immense power in exposing illegal activity and lack of data transparency.
There’s only one reason to hide data. To commit fraud. Put it out an the open, and it’s a hundred times more powerful then any other argument. No amount of ass covering or finacial motivation can fight something that kills careers and takes away profits.
@ a-non
This is a great find! I wish the references were cited though.. It’s hard to tell when there’s conficting information between news posts.
This seems to privde some detailed information as of late june though. Still no word who this mysterious corporation might wind up to be.
@Joel Hassman, MD
That’s a scary idea that thousands of people might wind up in acute drug withdrawal. There’s conflicting reports as to whether it happening though, I’m sure we’ll see though
Happy fall between the gloom and doom though.
TinCanRobot,
Thanks for your post but first of all, I reject the notion that I am a “patient”. I have been labelled with an invented illness (in my case it was OCD). I had recently an email communication with an academic psychiatrist the matter. I asked him explicitly, where is the “blood test” or “brain scan” that detects OCD. He conceded that there is none but he kept putting the line that it is nonetheless “real”. To which I say sure, just as Eintein’s genius was also real (just ask the field of theoretical physics). But claiming that pattern of behavior X, is an “illness” via a vote absent a biological test, is a “value judgement”. OCD is not an illness anymore than homosexuality is an illness (which is also real) or Eintein’s genius is an illness.
50 years ago, Thomas Szasz, wrote the ultimate critique of psychiatry. His paper “The Myth of Mental Illness” http://www.columbia.edu/cu/psychology/terrace/w1001/readings/szasz.pdf , was as valid then as it is now. In fact, especially in the aftermath of the Insel crisis, it seems that the NIMH has become Szaszian in its plan for the future with the line that one cannot call “illness” something that doesn’t have a biological origin. None of that matters until psychiatry is deprived of its coercive powers, which include not only the classic involuntary commitment/treatment but also the ability of psychiatric judgement to have any value in criminal and civil proceedings.
“This is a great find! I wish the references were cited though.. It’s hard to tell when there’s conficting information between news posts.” TinCanRobot
The source(s) are always in question, usually when I’m sniffing around I try to end up at a gov site ultimately.
For now I present this:
Optum Health New Mexico website
https://www.optumhealthnewmexico.com/
Just a side note: A friend is a pedi and hates this time of year. In the first week of school there is a constant flow of children all with ADHD request from the teachers, many of these notes include dosing demands with prescription levels that do not exist.
Her solution is sometimes a small dose to make the school happy and a referral to really see what the problem is and the problem is often a teacher that feels overwhelmed with a normal class of seven year old boys who are all active and wonder why school is not like Sesame Street.
Steve Lucas
Depending on income level, a false diagnosis might prove a useful recuitment tool for certain studies:
http://www.organicconsumers.org/school/beyondcheers051005.cfm
As I read them, most of Dr. Mickey’s posts question the direction of contemporary psychiatry and the evidence base for psychiatric drugs.
Here’s a cautionary tale of combining antidepressants and throwing in an adjunct antipsychotic:
http://cpnp.org/resource/mhc/2013/09/retrospective-review-case-serotonin-syndrome-after-discontinuation-risperidone
“At the time of presentation, the patient’s scheduled nursing home medication list included: venlafaxine, sertraline, trazodone, lorazepam, hydrocodone/acetaminophen, baclofen, conjugated estrogens/medroxyprogesterone, omeprazole, lisinopril, furosemide, potassium chloride, levothyroxine, docusate sodium, and calcium carbonate/vitamin D. “
Time to reevaluate the rat model? Addiction and mental illness?
“It’s not the morphine, it’s the size of the cage: Rat Park experiment upturns conventional wisdom about addiction”
“Alexander’s hypothesis was that drugs do not cause addiction, and that the apparent addiction to opiate drugs commonly observed in laboratory rats exposed to it is attributable to their living conditions, and not to any addictive property of the drug itself. He told the Canadian Senate in 2001 that prior experiments in which laboratory rats were kept isolated in cramped metal cages, tethered to a self-injection apparatus, show only that “severely distressed animals, like severely distressed people, will relieve their distress pharmacologically if they can.”
http://sub.garrytan.com/its-not-the-morphine-its-the-size-of-the-cage-rat-park-experiment-upturns-conventional-wisdom-about-addiction
Fox News has a brief article noting that PPACA will make doctors and patients HAVE to report sexual and drug abuse behaviors in at least some of treatment interactions, which then become part of the EMR. Umm, what is that agenda if true? The more this law is actually examined, it is becoming quite the travesty of polluting and controlling the health care agenda.
But, many here have said this law is ONLY good. Well, good for you all, until, something NOT good comes to pass. Bureaucracy is not a good thing when it takes on health care. Hence what is being experienced in New Mexico.
Keep waiting for the lame stream media to report concerns about PPACA. You might find out through personal experiences way before the truths are finally reported. Oh, is there going to be a post about the shooter in DC? You should read the crap that Dr Ablow wrote also at Fox. Absurd stuff some of our colleagues write.
have a nice evening.
“Putting all this together leads to the conclusion that the relatively small difference between drugs and placebos might not be a real drug effect at all. Instead, it might be an enhanced placebo effect, produced by the fact that some patients have broken [the] blind and have come to realize whether they were given drug or placebo. If this is the case, then there is no real antidepressant drug effect at all. Rather than comparing placebo to drug, we have been comparing “regular” placebos to “extra-strength” placebos.” – Irving Kirsch, Ph.D.
More here:
http://www.nybooks.com/articles/archives/2011/jun/23/epidemic-mental-illness-why/?pagination=false
Duane Sherry, M.S.
discoverandrecover.wordpress.com
Or as Irving Kirsch simply puts it, antidepressants are “worse than useless.”
And yet, doctors continue to prescribe them, like candy, with one in ten adults on them..,. Go figure.
Duane
Who defines what is “normal” and who controls the money/resource?
http://www.state.gov/s/fbci/
http://www.criticalpsychiatry.co.uk/index.php?option=com_content&view=article&id=284:a-philosophical-investigation-into-coercive-psychiatric-practices-roche-g&catid=34:members-publications&Itemid=56
“When religion and politics travel in the same cart, the riders believe nothing can stand in their way. Their movement becomes headlong – faster and faster and faster. They put aside all thought of obstacles and forget that a precipice does not show itself to the man in a blind rush until it’s too late.”
* Bene Gesserit proverb
Frank Herbert-Dune
That whole ‘personalized medicine’ or ‘optimized treatment’ thing creeps me out.
It’s the logic of saying that if we apply totally impractical and poorly replicated methods, we can justify off-label prescriptions by appearing scientific. If the treatments prevent recovery over placebo (such as the case with antipsychotic maintenance therapy in the NIMH directors blog), then it’s black and white the practice must be ended. Yet, claims that ‘some patients’ clearly ‘need’ the treatment are used to basically do a double-think.
(NIMH blog entry- http://www.nimh.nih.gov/about/director/2013/antipsychotics-taking-the-long-view.shtml)
The whole ‘optimized treament’ is a double-think. It’s harm-reduction by alowing off-label uses that harm over placebo to continue.
We often hear the deffinition of ‘insanity’ is doing the same thing over and over again and expecting different results. I think this only differs because the end result is that more money continues to be made by providing a service or selling a product that should not have been continued otherwise.
It has little to do with Pharma directly, but still everything to do with drug sales and providing that same ineffective type of service. It’s another way of pretending to legitimize off-label prescriptions, namely those that prevent recover over placebo.