But this is not a post about trigger-happy doctors, it’s about our literature. The articles are about the very real problem of patients with Alzheimers who become psychotic and agitated and often hurt themselves, particularly at night when in a state of sensory deprivation [sundowning]. A confounding problem is the well known fact that the usual "tranquillizers" and "sedatives" can have a dramatic paradoxical effect in dementia, actually causing agitation and psychosis. So the use of low dose antipsychotics which don’t suppress the cortical function makes medical sense, but the window is thin – the right amount might be good, but more is definitely not better. And the verdict on that usage has been mixed.
by Schneider LS, Dagerman KS, and Insel P.JAMA. 2005 19;294[15]:1934-1943.
CONTEXT: Atypical antipsychotic medications are widely used to treat delusions, aggression, and agitation in people with Alzheimer disease and other dementia; however, concerns have arisen about the increased risk for cerebrovascular adverse events, rapid cognitive decline, and mortality with their use.OBJECTIVE: To assess the evidence for increased mortality from atypical antipsychotic drug treatment for people with dementia.DATA SOURCES: MEDLINE [1966 to April 2005], the Cochrane Controlled Trials Register [2005, Issue 1], meetings presentations [1997-2004], and information from the sponsors were searched using the terms for atypical antipsychotic drugs [aripiprazole, clozapine, olanzapine, quetiapine, risperidone, and ziprasidone], dementia, Alzheimer disease, and clinical trial.STUDY SELECTION: Published and unpublished randomized placebo-controlled, parallel-group clinical trials of atypical antipsychotic drugs marketed in the United States to treat patients with Alzheimer disease or dementia were selected by consensus of the authors.DATA EXTRACTION: Trials, baseline characteristics, outcomes, all-cause dropouts, and deaths were extracted by one reviewer; treatment exposure was obtained or estimated. Data were checked by a second reviewer.DATA SYNTHESIS: Fifteen trials [9 unpublished], generally 10 to 12 weeks in duration, including 16 contrasts of atypical antipsychotic drugs with placebo met criteria [aripiprazole [n = 3], olanzapine [n = 5], quetiapine [n = 3], risperidone [n = 5]]. A total of 3353 patients were randomized to study drug and 1757 were randomized to placebo. Outcomes were assessed using standard methods [with random- or fixed-effects models] to calculate odds ratios [ORs] and risk differences based on patients randomized and relative risks based on total exposure to treatment. There were no differences in dropouts. Death occurred more often among patients randomized to drugs [118 [3.5%] vs 40 [2.3%]. The OR by meta-analysis was 1.54; 95% confidence interval [CI], 1.06-2.23; P = .02; and risk difference was 0.01; 95% CI, 0.004-0.02; P = .01]. Sensitivity analyses did not show evidence for differential risks for individual drugs, severity, sample selection, or diagnosis.CONCLUSIONS: Atypical antipsychotic drugs may be associated with a small increased risk for death compared with placebo. This risk should be considered within the context of medical need for the drugs, efficacy evidence, medical comorbidity, and the efficacy and safety of alternatives. Individual patient analyses modeling survival and causes of death are needed.
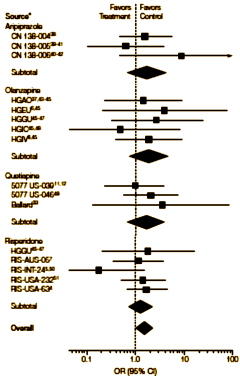 The forest plot in that meta-analysis of the atypical antipsychotics [top down: Abilify; Zyprexa; Seroquel; and Risperdal] showed a small negative signal [OR 1.54 p=0.02], supporting the Black Box Warning. I remember when it came out I thought it would reinforce only using the medications when absolutely necessary. And while I was relieved that the signal was low, it left things in limbo. I did think it was a thorough meta-analysis and one of the first where I realized how many negative trials went unpublished. When I saw the study below in this month’s AJP, I flagged it as something I hoped might clarify things. But I’ve gotten gun-shy about studies countering the FDA’s Black Box Warnings after so many examples that I thought were commercially biased rather than some kind of real useful clinical information.
The forest plot in that meta-analysis of the atypical antipsychotics [top down: Abilify; Zyprexa; Seroquel; and Risperdal] showed a small negative signal [OR 1.54 p=0.02], supporting the Black Box Warning. I remember when it came out I thought it would reinforce only using the medications when absolutely necessary. And while I was relieved that the signal was low, it left things in limbo. I did think it was a thorough meta-analysis and one of the first where I realized how many negative trials went unpublished. When I saw the study below in this month’s AJP, I flagged it as something I hoped might clarify things. But I’ve gotten gun-shy about studies countering the FDA’s Black Box Warnings after so many examples that I thought were commercially biased rather than some kind of real useful clinical information.by Lopez OL, Becker JT, Chang YF, Sweet RA, Aizenstein H, Snitz B, Saxton J, McDade E, Kamboh MI, Dekosky ST, Reynolds CF, and Klunk WE.American Journal of Psychiatry. 2013 Jul 30. doi: 10.1176/appi.ajp.2013.12081046. [Epub ahead of print]
OBJECTIVE: The authors sought to determine the effects of conventional and atypical antipsychotic use on time to nursing home admission and time to death in a group of outpatients with mild to moderate probable Alzheimer’s disease.METHOD: The authors examined time to nursing home admission and time to death in 957 patients with the diagnosis of probable Alzheimer’s disease who had at least one follow-up evaluation [mean follow-up time, 4.3 years [SD=2.7]; range, 0.78-18.0 years] using Cox proportional hazard models adjusted for age, gender, education level, dementia severity, hypertension, diabetes mellitus, heart disease, extrapyramidal signs, depression, psychosis, aggression, agitation, and dementia medication use.RESULTS: A total of 241 patients [25%] were exposed to antipsychotics at some time during follow-up [conventional, N=138; atypical, N=95; both, N=8]. Nursing home admission [63% compared with 23%] and death [69% compared with 34%] were more frequent in individuals taking conventional than atypical antipsychotics. In a model that included demographic and cognitive variables, hypertension, diabetes mellitus, heart disease, incident strokes, and extrapyramidal signs, only conventional antipsychotic use was associated with time to nursing home admission. However, the association was no longer significant after adjustment for psychiatric symptoms. Psychosis was strongly associated with nursing home admission and time to death, but neither conventional nor atypical antipsychotics were associated with time to death.CONCLUSIONS: The use of antipsychotic medications, both conventional and atypical, was not associated with either time to nursing home admission or time to death after adjustment for relevant covariates. Rather, it was the presence of psychiatric symptoms, including psychosis and agitation, that was linked to increased risk of institutionalization and death after adjustment for exposure to antipsychotics.
by D.P. Devanand, M.D.American Journal of Psychiatry. 2013 170:957-960.
The only reason I mention this article is that for one of the first times in a long time, I felt like I was reading something straight in our journals, better than straight, actually clarifying. They were bringing the previous literature and some data from a large cohort to bear on a very real and common problem. I thought the analytic method was clever, and took what had been done before a step further.
Nice post. Maybe I will start reading journals again. Maybe.
I hope to God I drop dead before I’m senile and end up in the hands of psychiatrists.
I recently talked to a couple of psychiatrists about the FDA’s black box warnings and listings of adverse effects in the PDA. One dismissed FDA warnings as merely “cover your *ss.” The other said the PDA had to list every reported adverse effect and dismissed them all as so rare he’d never see them.
So much for educating psychiatrists about adverse effects. What source would they believe?
Reading this article that seems to conclude that the real cause of the faster death of the elderly with “probable” Alzheimer’s is their old age/disease processes rather than due to the toxic neuroleptic drugs used raises many alarm bells with me. First, there is this statement from Dr. David Healy about our useless protector the FDA and other perils in medicine:
“Soon afterwards, following a UK model, an FDA Modernization Act led to FDA being part funded by industry and encouraged to partner industry. We could note that George H Bush had been on the board of Lilly. That Mitch Daniels, later the Governor of Indiana, ran the public relations around Prozac and suicide, coming up with the key concept – it’s the disease not the drug. ”
This “study” appears to be another blaming the victim enterprise to hide the very well known effects of lethal neuroleptics from which even Dr. Thomas Insel, Head of the NIMH, backed away in a recent release on his blog. On a recent post, I added an article by Dr. Joanna Montcrieff on these toxic drugs and a link to her new book, The Bitterest Pill on the sordid history of these lethal drugs and their many toxic effects. Many agencies have exposed and denounced the over use of neuroleptics causing early death among the elderly in nursing homes to literally shut them up. The Boston Globe did a series of articles on this growing menace to the elderly not to mention children as predation on the weakest and most powerless members of society for enhanced profits for Big Pharma, nursing homes and others of their ilk not to mention blaming the victims as usual.
http://davidhealy.org/pills-and-the-man/
There have been many studies showing that abuse of neuroleptic drugs with the elderly used in nursing homes and elsewhere to make them more easily controlled zombies requiring far less staff and care has led to many complications and early death. The same is true for ECT and other so called treatments forced on the powerless elderly in nursing homes and other vulnerable states and places with women having Medicare the main victims. This harks back to the days of the old mental institutions whereby brain damaging “treatments” were used to create docile “patients” to make life easier for their caretakers. There has been news of a comeback of lobotomy so old age and life in general grows more dangerous daily.
Finally, everyone knows that the DSM 5 was very controversial because it expanded already absurd expansions of the medicalization of life and other abuses that included the inclusion and expansion of Alzheimer’s for the obvious purpose of stigmatizing more and more people with even minor memory problems typical of aging even in midlife to push existing useless, toxic drugs and attract more of the same from Big Pharma. Even Allen Francis attacked the DSM V for this disease mongering expansion of Alzheimer’s in the DSM V among many others online and in his book, Saving Normal.
Thus, I think that such studies should be taken with not only a grain of salt but a whole shaker full of it given biopsychiatry’s/Big Pharma’s history. I suppose they will be advocating for depot injection neuroleptics for the elderly if they haven’t already since many Big Pharma corporations have extended their patents by converting to these even more lethal, deadly neuroleptics.
http://www.madinamerica.com/2013/08/nimh-director-acknowledges-
antipsychotics-worsen-long-term-outcome/
“Evidence that antipsychotics cause brain shrinkage has been accumulating over the last few years, but the psychiatric research establishment is finding its own results difficult to swallow. A new paper by a group of American researchers once again tries to ‘blame the disease,’ a time-honoured tactic for diverting attention from the nasty and dangerous effects of some psychiatric treatments.”
Article by Dr. Joanna Moncrieff on neuroleptics causing brain shrinkage:
http://www.madinamerica.com/2013/06/antipsychotics-and-brain-shrinkage-an-update/
http://www.psychologytoday.com/blog/mad-in-america/201102/andreasen-drops-bombshell-antipsychotics-shrink-the-brain
http://www.jewishterrorism.com/honey-they-shrunk-my-brain-study-confirms-antipsychotics-decrease-brain-tissue/
Scientific Proof: Antipsychotics Shrink Brain
http://www.ahrp.org/cms/content/view/772/9/
I’ve got my questions as well … it seems like such a classic case of “blame the disease not the drug.” Even if done more responsibly than the average Pharma-funded study. It’s been my experience that words like “agitation” and “aggression” — and maybe even “psychosis” — are used retrospectively by staff of institutions to cover their asses after they have implemented certain measures, like antipsychotic drugging, restraints or seclusion. Sort of like the charge of “resisting arrest” which is a retrospective charge the police may have to file after they have rearranged your face.
The other question I have is: did they control for dose and duration of drugging? A person with prominent “disruptive” symptoms would also tend to be a person given high doses, long-term meds, depot meds etc. Whereas a person who has dementia but who the staff admits is not “agitated” or “aggressive” may have received fairly minimal dosing …
Study shows atypical antipsychotics not worth the many risks for those over 40 years old
http://survivingantidepressants.org/index.php?/topic/3493-study-atypical-antipsychotics-not-worth-the-risks-in-those-over-40/
I don’t believe that psychotic symptoms are resposible for early death in alzheimers. Although there is correlation with some illnesses, like rabies in that regard. I’d have to see other behavioral/neurological symptoms that predict outcome before I would accept that. So far, symptoms are generally random.
One study found up to a 5 fold reduction in lifespan when the drugs are used, with clear differences between specific drugs and mortality recorded.
http://www.ncbi.nlm.nih.gov/pubmed/21474930
As Florence mentioned, antipsychotics cause pretty nasty brain dysfunction, including structural volume reductions. It is brain dysfuction (from neuronal death) that actually kills the patient in alzheimers, so one would expect lifespan to be negativly affected by addition of another factor of brain dysfuction.
One thing is certain, the use of the sedatives correlates with reduction in lifespan.
A better designed question would be:
“Does pharmacological treatment of neuropsychiatric symptoms in Alzheimer’s disease relieve caregiver burden”
http://www.ncbi.nlm.nih.gov/pubmed/22350526
No suprise, another off-label use of antipsychotics has no clear benefit.
Also, Florence, some of the references you used for citation are alright, like http://www.ahrp.org, http://www.psychologytoday.com, and http://www.madinamerica.com are reasonable places to cite something. They usually cite their references, and you could instead copy and paste those.
Scientificamerican.com has some great articles on these drugs and brain shrinkage. I mean really great articles, fully cited.
Another great source is the pubmed database at the NIH, also known as MedLine. a shortcut URL is http://www.pubmed.org
The NIH (a gov department in the USA) has a dozen databases, and you can switch between them, PubChem is a excellent source to find all known published information on a drug.
Really, please don’t ever link to somthing like:
http://www.jewishterrorism.com
As soon as i saw that i ignored the rest of your posts.
There’s a lot of good informtaion out there reposted or archived, but you never want to get it from somewhere like that.
TinCanRobot,
Thanks for your alerts. You are right only in that I am not familiar with the jewishterrorism web site and in my haste I just thought it was a normal Jewish web site that had the information I was seeking while not checking out the other things there. I still don’t know what the web site is about, but I’ll check that out as time permits while not using it for this purpose again.
Actually, I was pretty sure that Dr. Nancy Andreasen, the great “schizophrenia expert,” had articles written about her and/or written them herself recently where she finally admitted and published the fact that antipsychotics cause brain shrinkage/damage, but when I tried to find them I suspiciously had a hard time. This seems to happen often with articles that might threaten the biopsychiatry/Big Pharma cartel. Since I didn’t have time to search indefinitely, I posted articles that contained information about atypical neuroleptics with which I’m very familiar that included the article that seems to have offended you. Therefore, I apologize for that and your point is very well taken. I will be much more careful in the future.
I have total respect for Jewish people and as you can see on another post, I included an article by Dr. Peter Breggin, who is Jewish, about the contemptible role psychiatry played in the horrific Nazi Holocaust due to their eugenics theories that continue today. You will also see that I gave Dr. Breggin the highest praises, so I am certainly not anti semitic, but rather, share their heritage through my own Christian background. However, your point is well taken and I hope you will forgive me.
Here’s a recent New York Times article about Andreasen latest “bombshell” about her coverup of the fact that neuroleptics do indeed cause brain shrinkage and damage, which is why they should not be used on those over 40 per a study I cited above never mind the elderly in nursing homes.
http://www.nytimes.com/2008/09/16/health/research/16conv.html?_r=0
You offered some very good points and references yourself, which I appreciate.
Florence,
I think it’s some ‘conspiracy’ site, lol. Google actually has a seperate search engine for scholerly articles, otherwise google doesn’t always sort well.
http://scholar.google.com/
You might find this one interesting:
http://www.nature.com/news/2010/100606/full/news.2010.281.html
(or very worrying)
—
The Pubmed database is the largest index of scientific publications on earth, where all important scientific publications for researchers are made availble by a free-to-the-public tax funded department of the US gov, the NIH.
It also allows you to search by author
http://www.ncbi.nlm.nih.gov/pubmed?term=Andreasen%20NC%5BAuthor%5D&cauthor=true&cauthor_uid=16055776
Nifty huh?
Not sure why that link didn’t come up properly, “Author” should be inside brackets “Andreasen NC[Author]”
You can use the clickable “Display Settings” drop-down menu in the top left to arrange by “Pub date” to sort for chronological order.
http://www.ncbi.nlm.nih.gov/pubmed?term=Andreasen%20NC%5BAuthor%5D&cauthor=true&cauthor_uid=16055776
TinCanRobot,
Thanks for the research tips. I tend to go more with trusted names and sources since I’ve done a great deal of research on this topic for many years. I tend to be very cautious about mainstream research without trusted authorities to interpret it like Robert Whitaker, Dr. Peter Breggin, etc. I appreciate your helpful research tips because certain things are hard to find at times.
Perhaps Andreasen’s research isn’t available from those links you cited because she admitted she didn’t publish it in the NYT article for dubious reasons like covering up the fact that neuroleptics cause permanent brain damage and shrinkage. That makes me question the article from Nature claiming the shrinkage is permanent when many, many other good studies show the shrinkage/damage is permanent which is obvious with such permanent damage like tardive dyskinesia not to mention early death by about 25 years on average with drug induced dementia as well per Dr. Grace Jackson’s work, Drug-Induced Dementia: A Perfect Crime.
http://www.amazon.com/Drug-Induced-Dementia-MD-Grace-Jackson/dp/1438972318
Correction: The Nature article claimed the brain shrinkage from neuroleptics is temporary while other very credible sources claim it is permanent. (I mistakenly wrote that the Nature article said it was permanent…)
Andreasen news: http://now.uiowa.edu/2013/08/how-schizophrenia-affects-brain
Altostrata,
Thank you for the updated article/link about Andreasen’s ongoing coverup of the brain damage and shrinkage caused by neuroleptics and possibly other psych drugs that led up to the supposed psychosis/altered brains she claims are part of the bogus schizophrenia label. This article like so many others blames the victims’ supposed faulty brains for totally made up social constructs lacking all science and evidence.
But, finally, at least she is admitting the harm of neuroleptics.
I mistakenly said these poison drugs shouldn’t be used for those over 40 or the elderly when they should not be used for anyone regardless of age or any other bogus criteria.