Looking back, I can now see that they based their predictions on the promise of some new technologies that they felt sure would be confirming – the cracking of the genome and non-invasive functional neuroimaging. We’ve long known that many mental illness run in families [see too big a hurry…]. So with modern genetic sequencing techniques, they felt it was only a matter of time before the genetic bases of some mental illnesses would be handed to them on a platter by the herd of researchers looking for the answers. Likewise, we all know that the brain is the seat of matters mental. Being able to study the brain in action with the fMRIs would surely yield a cornucopia of confirmations. So the bet wasn’t so risky after all. All they had to do was wait. It was in the bag. And with luck, the neurochemists might come up with a biomarker or two that sealed the deal. No more turtle science. The hares had arrived!
by Maciej Trzaskowski, Philip S. Dale, and Robert PlominJournal of the American Academy of Child and Adolescent Psychiatry. 2013 52[10]:1048-1056.
OBJECTIVE: Twin studies of behavior problems in childhood point to substantial genetic influence. It is now possible to estimate genetic influence using DNA alone in samples of unrelated individuals, not relying on family-based designs such as twins. A linear mixed model, which incorporates DNA microarray data, has confirmed twin results by showing substantial genetic influence for diverse traits in adults. Here we present direct comparisons between twin and DNA heritability estimates for childhood behavior problems as rated by parents, teachers, and children themselves.METHOD: Behavior problem data from 2,500 UK-representative 12-year-old twin pairs were used in twin analyses; DNA analyses were based on 1 member of the twin pair with genotype data for 1.7 million DNA markers. Diverse behavior problems were assessed, including autistic, depressive, and hyperactive symptoms. Genetic influence from DNA was estimated using genome-wide complex trait analysis [GCTA], and the twin estimates of heritability were based on standard twin model fitting.RESULTS: Behavior problems in childhood-whether rated by parents, teachers, or children themselves-show no significant genetic influence using GCTA, even though twin study estimates of heritability are substantial in the same sample, and even though both GCTA and twin study estimates of genetic influence are substantial for cognitive and anthropometric traits.CONCLUSIONS: We suggest that this new type of "missing heritability," that is, the gap between GCTA and twin study estimates for behavior problems in childhood, is due to nonadditive genetic influence, which will make it more difficult to identify genes responsible for heritability.
Discover BlogsBy NeuroskepticOctober 8, 2013A paper just published reports that there are: No Genetic Influence for Childhood Behavior Problems From DNA Analysis. This is pretty big. Using a powerful approach called GCTA, King’s College London researchers Maciej Trzaskowski and colleagues found no evidence that genetics can explain differences in children’s behavioural and conduct difficulties.
First some background. ‘Missing heritability‘ refers to the fact that genetics has mostly failed to find common genetic variants that are associated with ‘complex traits’ like personality, mental disorer and intelligence. This is surprising because these traits are largely heritable – meaning that they run in families, and that identical twins [with all their DNA in common] tend to be more similar than non-identical ones [with only half]. But if they’re heritable then, by definition, there must be genes behind that. But with a few minor exceptions, over a decade of studies drew blanks. Hence the heritability is missing in our DNA, unaccounted for.
Yet geneticists finally struck gold – or seemed to – with a new technique called genome-wide complex trait analysis [GCTA]. Instead of looking at each variant individually, GCTA quantifies how genetically similar any two people are as a whole. GCTA has shown that the more genetically similar people are, the more similar they tend to be in terms of complex traits. Hooray – the missing heritability is… well, it’s still missing, but at least we know it’s out there, in small pieces scattered across the genome.
But this good news only applies to some complex traits, according to Trzaskowski et al. It doesn’t hold for child behaviour. In the TEDS sample of British twins, the authors conducted a simultaneous twin and GCTA study. During childhood these twins were assessed for IQ, height, weight, and a range of ‘behaviour problems’ including symptoms of autism, hyperactivity, psychopathy, conduct disorder and more.
The results of the twin study said that all of the traits were moderately heritable [roughly 0.5 on the scale of 0 to 1]. But while GCTA confirmed a large genetic influence on the intelligence traits, height and weight, it found no genetic influence on the behaviour measures: The difference between the two sets of traits is stark:
The same picture was seen whether it was parents [shown here], teachers, or the children themselves rating their behavioural symptoms. So, some of the missing heritabilities have been located [if not pinned down], but others are more missing than ever. Trzaskowski call it a “new kind of missing heritability” but I wonder if the name “mystery heritability” is more appropriate in relation to these behavioural problems. What’s going on?
The authors say that GCTA can only detect additive genetic effects, and can’t detect nonlinear interactions between genes. But the trouble is, the twin data just aren’t consistent with the idea that nonadditive effects explain any of these traits. However, Trzaskowski then suggest that the results make sense if we assume that twin studies substantially overestimate the heritability of behaviour problems [but not intelligence].
This might be because behaviour problems are just questionnaire ratings of traits, which are essentially subjective and prone to bias [e.g. by parents who assume that their identical twins ‘must be identical’ and rate them as such], while intelligence tests, although not perfect, are less easily fudged.This account does leave room for some genuinely heritability, but only a little.
It says to me that what looks like inherited complex behavior, indeed by all reports is at least partially inherited complex behavior, does not fit the genetic concepts of our current thinking – and isn’t likely to fit in the near future. I see it as confirmation, here in Dr. Insel’s Decade of Discovery, that we don’t yet know what we think we know about the inheritance or the hypothesized biological substrate of human behaviors. And we are anything but a year and a half away from the long yearned for Decade of Translation:
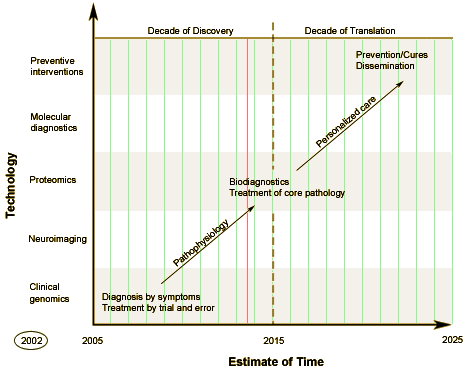
Although I have always thought Dr. Insel’s Clinical Neuroscience call was at best premature and more likely way overstated, I don’t post this just to rub his nose in that map. Time has already done that quite well. I mention it because valuable NIMH resources are still being squandered on the obsession with Translation in general – a frantic hurry-up to legitimize psychiatry’s biology. That’s not what the NIMH is for. That’s not what psychiatry is for either. We know a lot more about caring for mentally ill people than we’re doing right now – things forgotten in the current climate. This study is just one of many pieces of evidence that says priorities need re-evaluating and resources need re-allocating.
If there’s one blog post that Dr. Insel needs to take another look at, it’s Director’s Blog: Balancing Immediate Needs with Future Innovation from January 2012. How many more studies does he need to see that say fund free-range basic research and look at the very real problems of right now with new glasses instead of chasing the now very tired dreams of he and his cronies? If he can’t escape the rut he’s in, he needs to find somewhere else to be in his rut. His version of just-around-some-corner-future-innovation has failed the test of time.
If it has neither been the Decade of Discovery nor the Decade of Translation, what should we call this time? I think that it’s already on Dr. Insel’s slide. Realistically, we’re still in the time of Trial and Error. And rather than lamenting or denying that fact, it is incumbent on us to absolutely insure that our Trials [our Clinical Trials] are the best they can be. This is the Time of Clinical Trial Reform and our current task is to insure that we do that thoroughly. It’s exactly what we’re supposed to be doing right now…

Looking at this from the outside I have watched as friends have raised their children and now grandchildren with the expectation that if they do x they will get y result and any deviation is caused by a medical issue.
Force the children to watch PBS and they will become social, singing, tree huggers. When the kids instead want to run around and make noise they feel there is something medically wrong. After all there are “test” and “medications” and we followed the instructions for giving our children an enriched childhood experience.
This focus on the physical and medication has often robbed children of their identity and personality. I will leave it to those who are much smarter than I to discuss the parents using these situations to their benefit.
I have been amazed when interacting with friends children how few problems I have with the children. There are clear fair expatiations and room for self expression. When boundaries are broached there are clear consequences and explanations.
This rush to give Johnny a med because the parents just “know” there is a problem is robbing not only the children but society of their future.
Steve Lucas
I’ve encountered a lot of that do x (consistently) and the child will do y, with social workers and psychologists. Our society doesn’t have much room for children. While a nanny for a girl with special needs with a poor father. I attended a parenting class he was required to attend and learned that it’s enough for a parent to spend “15 minutes of quality time with their children” a day. Because so many working parents don’t have time for their children.
It was fascinating to watch the little panel of experts rolling their eyes at parents who did not consistently do x so their child would do y— why it was just ridiculous that parents didn’t know how to set limits on their children and enforce them. In that position, I had to bite my tongue; but I just looked on them in awe of their complete unawareness that it was people in their field telling parents that the word “no” would prevent them from being creative as if “yes” means anything without “no” and as if they had the faintest clue about what creativity is and how it works.
Our society— especially the professional part of our society— does not have time for children. Children don’t give a quarterly return, and their care depends on unpaid and low paid labor.
I would so love to see you write a dense synopsis of the problem with the “science” in psychiatry, Mickey. A lot of liberals think that “science” is something monolithic and pure, when there isn’t even “science” there are sciences, and the profit motive is corrupting them.
Sciences are not pure and all the hubris of humanity is as much ingrained in the sciences as it is philosophy and political science. That, when the Human Genome project began, it was somehow truth that that the DNA they didn’t understand was “junk” is an example of how scientific minds can delude themselves and interject “knowing” where an open question mark should be.
Still, anyone who hasn’t read this article about the social life of genes will likely find it very gratifying and hopeful.
http://www.psmag.com/health/the–life-of-genes-64616/social
That doesn’t suprise me. Behavioral problems don’t necessarily result in hosptilization or a prison sentence, so they’re not really ‘medical’ in the sense of the word. ADHD is something for psychology to treat, not a medical specialty.
It hadn’t occured to me a similiar but different problem might be occuring with schizophrenia gene sequencing research. Schizophrenia hasn’t been shown to be hereditary, and does not occur from birth in most cases, and like many aquired illnesses that can produce symptoms of persistent psychosis, they might result from environmental exposure to infections or toxic elements/compounds. It’s possible even if genes switches were found flipped in response or feedback to these things, it wouldn’t neccessarily exceed what is considered normal. The discovery of neurosyphilis and mercury poisoning were good examples.
Progress probably needs to be made first in estabilishing CNS dysfuction before genes should be explored, as there’s simply no rational for jumping to genes with no idea at all what is being looked for. Psychiatry is still struggling to adopt the term ‘brain dysfuction’ to replace ‘mental illness’, and until that happens Dr. Insels approach won’t make ay sense at all. I can’t see even that happening until psychiatry shrinks back to a role treating only medical illnesses and not problems-of-life/behavioral issues. We know who’s paying for those things to be treated though, pharma.
“Not knowing what you think you know” is a fair summary of anosognosia.
What do you mean “establishing CNS dysfunction”? How is psychiatry supposed to “shrink back to the role of treating only medical illnesses” when, as this post addresses, they have little to no scientific evidence to support the “brain dysfunction” hypothesis? What good would substituting the CNS for genetics or any or any physical cause of ‘mental illness’? Once a condition is determined to be neurological then it should be treated by neurologists, not psychiatrists.
wiley,
I meant that neurology believes ‘psychiatric’ symptoms are produced randomly by CNS dysfuction, while the NIMH belives the symptoms are specific to specific dysfuctions. That ladder of which does not have any evidence to support it, while the former has been demonstrated by everything from drug withdrawal to B-12 deficiencies.
Psychiatry needs to do basic research to correct their approach, because no progress has been made trying to make corelations with specific dysfuctions and mental disorders or symptoms.
There is some reasonable evidence of psychotic patients having abnormal QEEGs, but each patient is different… correlations with specific symptoms of mental illness simply don’t exist.
Psychiatry is just applying the ‘evidence’ though an approach that makes no sense… so nothing is resulting.
Psychiatry has tried to distance itself from psychology, because it wants to be medical specialty. If psychiatry treats ADHD, it’s a big step backwards from that, and thus a big step backwards from scientific progress of determining a cause of illness.
Simply put, “psycho-biological” is not the same as biological. The treatments may be biological, but the research is not. Psychiatry does not research pure biological illness just to see what the psychiatric symptoms are. As a result, psychiatry lags behind neurology is making the corelation that psychiatric symptoms are produced at random, and an approach towards making corelations with specific symptoms and specific causes will not work.
The APA is lost and without a soul, as far as most responsible and invested psychiatrists go, not that most who write here know the difference between a psychiatrist who cares versus who profits.
I am going to be off the gird for a week, for the first time in a while, and it will be interesting with the BS going on in Congress and DC as a whole, what the F— will happen these next several days. Frankly, when I return to the shores of the US next week, if the country still exists, irregardless just about psychiatry or the whole damn process as a whole, I just hope some who are plainly bad and just out to screw the public, they are ruined and made useless to the process.
That would be nice. Have a great week people, I plan to!!!
Joel,
Bon Voyage!
Right, Tin Can. I think it’s funny that the field has determined that bipolar disorder is often “comorbid” with MS. Here they have clear evidence of lesions in the brain, but psychiatric symptoms must be that elusive biological condition that can’t be found in autopsies. You’d think that they would at least lean toward wanting to understand how lesions in the corpus callosum might cause mood disturbance, but nooooooooo.
http://www.ncbi.nlm.nih.gov/m/pubmed/21749303/
http://www.ncbi.nlm.nih.gov/m/pubmed/23810479/
http://www.ncbi.nlm.nih.gov/m/pubmed/23122540/
Wiley, as these examples indicate, there does seem to be interest among psychiatric researchers in the topic you mentioned. Though I may have misunderstood the thrust of your post.
Interesting Annonymous, I’ll take a closer look at these. There were small sample sizes, and what was previously thought to be a shrinking of brain volume from psychosis, was eventually found out to be the effects of drugs. I’m not dismissing these studies as having no value, and would appreciate it if you post new studies along these lines but I still think the “comorbid” label is used a bit too freely and it conveniently leads to cocktails of drugs that are very seldom studied in combinations such that the researchers and clinicians cannot say with any evidence-based confidence what effects these drugs and combinations of drugs have on individuals.
Furthermore, bipolarity may not be— I would say is unlikely to be— a single discrete condition. Many psychiatric symptoms may as well be “flu like” symptoms in the uncharted universe of the human brain. Besides the fact that many people have one incidence of psychosis their whole life and recover without medication, psychoactive drugs— prescription and illicit— can cause imbalance in brains that make a person more likely to have a psychotic episode.
http://wileywitch.com/2013/uncategorized/ssri-induced-mania/
The new “axiom” that antidepressant “unmasks” bipolar disorder is entirely to questionable and not understood in scientific terms to be an axiom. It’s also quite convenient for drug companies and KOLs who benefit from setting treatment standards.
Is it really true that anyone who has a drug induced mania was hiding their bipolarity should take psyche drugs for the rest of their life lest they become hopelessly psychotic even if the very worst and most debilitating years of their life was the time they took those drugs? For those who might possibly just have one or two psychotic episodes, are those really so bad that they must spend the rest of their lives on debilitating drugs (that don’t really significantly prevent psychosis)? I don’t think so.
And as long as the field is dismissing traumatic stress, unbearable grief, and overbearing social stresses, they are ignoring triggers and strategies to deal with stresses. Biological psychiatry is colonizing the human mind by dismissing it.
it ate my comment
Note: I found it. I have no idea why the spam lady ate it. She’s a loose cannon sometimes.
Mickey
There’s also an autoimmune disease called PANDAS that can result from a Strep A. infection.
This condition can produce Tic disorders, OCD, ADHD, Mood changes, Pain, etc.
http://www.nimh.nih.gov/health/publications/pandas/index.shtml
The NIMH uses the word “triggered” instead of the words ‘produced’ or ’caused’ or ‘results in symptoms of’.
I wouldn’t say gastritis ‘triggered’ vomiting. Or an overdose of cocaine ‘triggered’ seizures. Yet they say PANDAS ‘triggered’ OCD.
Are they implying the sick kids were predisposed to these symptoms, and PANDAS just brought them out?
Ah, there it is, plain as day.
“Could an adult have PANDAS?”
“No. By definition, PANDAS is a pediatric disorder. It is possible that adolescents and adults may have immune mediated OCD, but this is not known. The research studies at the NIMH are restricted to children.”
It always left me scratching my head. Just what do they think these symptoms are? They’re suposed to be symptoms, not disease entities! I know a little better now, but really, it’s just so bizzare… the NIMH is stuck in alternate philosophical world that collapses if symptoms are just random symptoms after all.
PANDAS isn’t a mental disorder, but it’s symptoms are their own disorders.
Wiley,
I was looking for that SSRI paper for months! I lost it and had no idea why i couldn’t find it.
Thanks!!
You are spot on about “The new ‘axiom’ “.
“Withdrawal following chronic therapeutic use may unmask symptoms of the underlying disorder that may require follow-up.”
– Ritalin’s Black box warning.
http://dailymed.nlm.nih.gov/dailymed/lookup.cfm?setid=c0bf0835-6a2f-4067-a158-8b86c4b0668a
How can one unmask symptoms of groups of symptoms? 0.o
I guess one can make the problem worse, but i don’t think that’s ‘unmasking’.
It’s very common for withdrawal symptoms to be misdiagnosed as relapse, “unmasking” of prior disorders, or emergence of a new, exotic disorder.