Adverse emotional and interpersonal effects reported by 1829 New Zealanders while taking antidepressantsPsychiatry Researchby John Read, Claire Cartwright, and Kerry Gibson3 February 2014
Background: In the context of rapidly increasing antidepressant use internationally, and recent reviews raising concerns about efficacy and adverse effects, this study aimed to survey the largest sample of AD recipients to date.Methods: An online questionnaire about experiences with, and beliefs about, antidepressants was completed by 1829 adults who had been prescribed antidepressants in the last five years (53% were first prescribed them between 2000 and 2009, and 52% reported taking them for more than three years).Results: Eight of the 20 adverse effects studied were reported by over half the participants; most frequently Sexual Difficulties (62%) and Feeling Emotionally Numb (60%). Percentages for other effects included: Feeling Not Like Myself – 52%, Reduction In Positive Feelings – 42%, Caring Less About Others – 39%, Suicidality – 39%, and Withdrawal Effects – 55%. Total Adverse Effect scores were related to younger age, lower education and income, and type of antidepressant, but not to level of depression prior to taking antidepressants.Conclusions: The adverse effects of antidepressants may be more frequent than previously reported, and include emotional and interpersonal effects.see also:
| Note: This article is getting and should get a wide audience because it confirms what many people have already been saying – that the antidepressants have a lot of unmentioned side effects and are no panacea for depression. But for the record, as a practitioner, I was only surprised by a few of the numbers. I wouldn’t have guessed that the suicidality figures would be as high as reported here, though I would’ve been close, and about right on the "severe" end. Similarly, I would’ve underestimated withdrawal and missed with withdrawal from Tricyclics. My experience with them is limited, but I haven’t seen withdrawal. But thanks to what I’ve learned as a blogger, I’ve learned to taper everybody, so I’m not surprised that I underestimate withdrawal incidence. Celexa is actually the only SSRI I use in new patients, and I’m pleased to have the reasons confirmed by this survey. |
The history is well known to us. When these drugs were first introduced, we were lead to believe that the sexual side effects were occasional. And as it became apparent that was untrue, the drug-makers fought that truth tooth and toenail. When the issue of suicidality was first on the table, the same fight ensued. It’s still going on with the endless attempts to disprove the black box warning put in place in 2004 using population statistics. Well this article uses population statistics in the right way, they asked the question directly and the results are right there in black and white. The main findings are in the abstract above. Here’s the breakdown by specific drug:
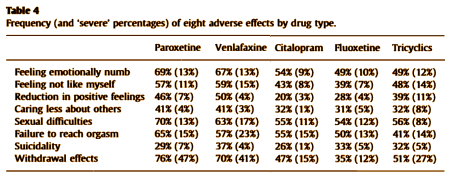
In my own musings about these medications since they came out, I’ve wondered how they work. I don’t think I ever thought that they had a primary effect on depression per se, nor did I ever think they were acting at some fundamental level on the cause of depression. When it became apparent how common the sexual side effects were and I started hearing about those first four symptoms in the table, I wondered if they were working by dampening down the emotional system in some global way, and the fact that some people with anxiety disorders are so responsive seemed confirmatory. Some patients complained about those first four symptoms and stopped the drugs. Others seemed to welcome them, saying something like "I need to be turned down." But the main observation I can add to that was something I noticed when I left practice.
My practice was primarily a psychotherapy practice with patients who were treatment failures from other therapies. I was a rare medication user: short term Benzodiazepines for crises; stimulants for some adult patients with undiagnosed ADD; some time limited Inderal for people with performance anxiety. When I retired, I went over every case I’d seen as sort of an exit exercise, and the surprise to me had to do with SSRIs. I’d used them here and there along the way, but in retrospect, every case I had with significant PTSD was on SSRIs. And I came to think think that was because those patients are hypervigilant, have affect storms, and actually do better with the volume turned down. I was surprised that I hadn’t noticed that along the way, but I didn’t.
I wasn’t surprised by this next part either. Most SSRIs are prescribed by Primary Care Physicians and people take them for a long time. Lots of people I see are reticent to "give them up," however people who’ve been on them for a long time frequently feel better when they’re off of them – "I feel my life."

But I’ll have to admit that this next part was a surprise:

83% improvement? With this?
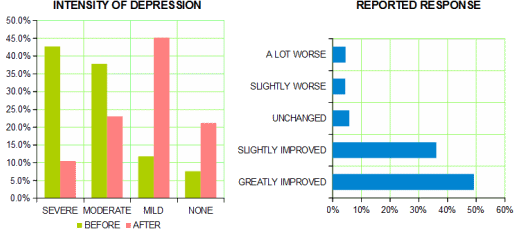
One doesn’t know how representative on-line responders are vis á vis the general population exposed to antidepressant drugs. The fact that so many took the drugs for a long time suggests they may not be representative. At least one study has looked at adherence to the drugs in primary care – it found that most patients did not refill their prescriptions after 30 days.
That said, the self-reported benefit to these self-selected respondent patients is, as you say, more encouraging than most clinical trials would allow us to hope for. It is certainly superior to the experience of the STAR*D trial. That they report such improvement despite the side effects is testament to the aversive quality of untreated depression.
Just as the super-high rate of treat response is likely due to a placebo effect, I wouldn’t be surprised if the high rates of reported adverse events is at least partially due to a nocebo effect. Which makes uncontrolled surveys like this very hard to interpret.
Not too surprising to me. If clinical psychiatry was really like STAR*D or CATIE – most of us would have quit a long time ago. But then again – you have to be cognizant of Table 4 and manage and prevent those side effects even if it means stopping an entire class of medications.
I have a couple of thoughts on this subject from the outside:
Many PCP’s practice outside their area of expertise and one of those areas is prescribing antidepressants. They see a problem, they have a pill, and in the two or three minutes of a typical visit someone is medicated.
I am trying to deal with a professional whose depression has become the cornerstone of their professional personality and an excuse for any behavior.
The medical community has come to celebrate taking antidepressants as becoming more self aware with the result that those not involved in this type of medication are deemed lacking in knowledge.
It has become almost impossible in today’s world to deal with certain people as they are “sensitive.” Knowing that a mental health issue will protect them from performance standards it is easy to adopt depression as an excuse.
Depression is real, but it is not treated by a pill in two minutes. Depression is also not an excuse to abuse those around you with unacceptable behavior.
My shock has been at the acceptance of this by the general medical community and often promotion of depression as an excuse for unacceptable behavior.
Steve Lucas
Antidepressants are psychotropics that cause sensory, cognitive, and affective changes, as well as side effects. Some people interpret these changes as beneficial, some find them unpleasant, and some don’t feel them at all — about what you’d expect from a drug class that is not any more effective than a placebo.
In clinical trials of antidepressants, generally about a third of subjects drop out, usually because of intolerable side effects. However, clinicians still prescribe antidepressants to this population and, obeying years of instruction from the drug companies, manipulate, coax, and bully these people into staying on the drugs for extended periods of time.
Having been told they need the drugs for their psychiatric conditions, patients who have endured adverse effects for years are highly invested in believing the drugs were good for something.
I submit that some part of this glowing self-report about efficacy is due to cognitive dissonance. While the individuals are reporting an uncomfortable rate of adverse effects, they need to rationalize their continuing to take the drugs. Hence, “must of helped my depression because I don’t feel like that anymore.”
“Celexa is actually the only SSRI I use in new patients, and I’m pleased to have the reasons confirmed by this survey.”
Do you think it’s safer than Prozac? Prozac obviously has bad sexual side effects, but the withdrawal seems less problematic because of the longer half-life.
EastCoaster,
What you say is correct. But since I taper 100% that doesn’t matter so much. I saw several cases of suicidaity on Prozac, and rarely with Celexa. That may be coincidence, but it swayed me. The other thing is that I’ve had good luck with low doses [5 mg, 10 mg] and those Prozac capsules are hard to break up.
Good to hear you’re using lowest effective dosages, Dr. Mickey. People are routinely overdosed on antidepressants; too often a benzo is thrown in to counter adverse effects.
Thank you profusely for tapering everyone!