In musings…, the thing I was musing about wasn’t, apparently, clearly stated based on some emails and tweets that came my way. Here’s another shot. I work as a volunteer in a local charity clinic. There are several reasons, but one of the main ones is that the local primary care physicians and my colleagues in the clinic don’t know much about psychiatric medications and treat them as if they are like the symptomatic medications in the rest of medicine. So if a person is depressed, the give an antidepressant. And if the patient returns saying I’m still depressed, then they add another, or some other psychiatric medication like an atypical antipsychotic that’s advertised for depression. And so patients are walking around taking hands full of pills, and if they stop, they have withdrawal symptoms. It’s a mess. So as much as I’d like to get a lot of them medication free, at least I can slowly bring things down to something rational – to levels that meet some kind of conventional standard. And with patients with psychotic illnesses, I can lower doses, trim the polypharmacy, monitor for TD etc. There’s a lot more that can be done as a glorified social worker, and I find that very rewarding having gotten a pretty good feel for the resources in the community. And then there’s crisis intervention, and some limited psychotherapy. We have three volunteer "therapists" and so when I find a person who badly needs counseling, I can refer them.
This was foreign soil to me, but I enjoy it enough and feel like it’s helpful enough to keep at it. But I can’t help but make some observations working there. As I said, one of the observations is that a lot of the pressure to medicate comes from the patients themselves. They’d be glad for me to give out Xanax like people did in the past. It’s a major drug of abuse in these parts in spite of the hypervigilance of pharmacists, DEA, and Georgia Narcotics Bureau. I use those drugs in acute crises, in some patients with panic disorders, and in psychotic people as a way of minimizing antipsychotics – pretty standard fare. But saying "no" to requests for benzos is a major activity of every clinic day. There’s another surprising pressure from patients – antidepressants. Like everywhere, there are large numbers of people on SSRIs, and they both complain that the drugs aren’t enough and insist on continuing to take them. I’ve read all the explanations for that: television ads; withdrawal if they stop; pressure from doctors; hopes for a panacea; etc. and I’ve seen a lot of every one of those. But that’s not the whole story. They sure aren’t pressured by me. And I find that people with false hopes aren’t that hard to wean off the drugs if one is careful and have some alternative ways to improve their lives available. But I’m personally convinced that a lot of people take them for a reason that is related to drug effect. And a lot of people who stop them, come back later asking for them – even knowing the negative effects that caused them to stop in the first place. In spite of their negative effects, they get something from taking them. The question is what? not if? in my mind.
So, if I’m right, what is it? and is it good for them? I’ve never bought that the antidepressants are specific antidotes for depression, even though it’s clear that they help some people with depressed affect. They help other people too – patients with OCD, patients with anxiety disorders and panic attacks, women with bad PMS symptoms. They often work better in those conditions than in depressed people. And the notion that the antidepressant properties and the side effects can be separated is a fantasy of chemists, not a reality that I’ve seen. So I’ve assumed that the therapeutic benefit [when there is one] is part of the same complex of effects as the downside side effects. That’s why I jumped on that NZ study, because the incidence and quality of the side effects they reported feels right. And the cohort they describe is reporting a double edged sword, a compromise. That’s what I see from these drugs myself. And since I don’t think these medications are specific antidepressants, I wonder what they are actually doing.
The universe isn’t very helpful with that question. The pharmaceutical industry and a whole generation of psychiatric KOLs preach the gospel of ANTIDEPRESSANTS as if they should work specifically for all depression. If they don’t, the patient has TREATMENT RESISTANT DEPRESSION and drugs are changed, combined, augmented, the patient is genetically screened, etc. There’s even a move to have a diagnostic scheme that fits the drug’s effects [RDoC] rather than the clinical symptoms. I don’t find that line of thinking at all helpful. On the other side of the coin, there are people who point to the same things I point to on this blog – the academic-pharmaceutical alliance, the experimercials, the KOL class in psychiatry, the bio-bio-bio rhetoric, the myth of chemical imbalances, the dreams of neuroscience, the DTC television ads, etc. In their view, these drugs are all hype, created by entrepreneurs, charlatans – a mass hypnosis. All of those things happen and are real. I don’t like them either. But they don’t address the fact of the patients I see that would answer the questions exactly like the cohort in New Zealand – these medications are a double edged sword, a compromise that they prefer to the alternative.
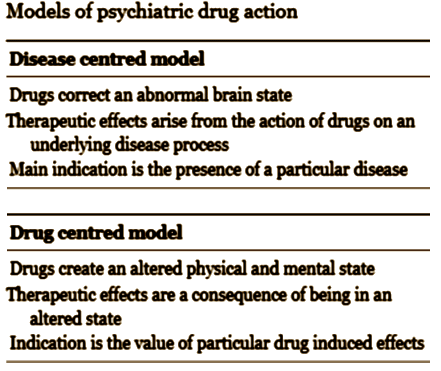
by Joanna Moncrieff and David CohenBritish Medical Journal. 2009 338:b1963.Drugs for psychiatric problems are prescribed on the assumption that they mostly act against neurochemical substrates of disorders or symptoms. In this article we question that assumption, proposing that drugs’ action be viewed rather as producing altered, drug induced states, a view we have called the drug centred model of action. We believe that this view accords better with the available evidence. It may also allow patients to exercise more control over decisions about the value of pharmacotherapy, helping to move mental health treatment in a more collaborative direction.
[modified to fit your screen]
I don’t mean to trivialize her work by saying this, because she has lots of important things to say, but for this post, that slide says it all clearly and simply [in spite of the mispelling – just kidding]. In my way of thinking, her drug centered model has to be correct in this instance. I know of nothing that suggests the antidepressants are specific anti-depressants [a possible exception is that sometimes, the Tricyclics reverse endogeous depression in dramatic fashion – emphasis on sometimes]. From where I sit, the SSRIs create a syndrome that is perceived as helpful by some depressed people. I say that they "turn down emotions" and use words like "blunting" or "dampening." Others say that in a more perjorative way – "numbing." That would explain their effects in GAD and OCD. I don’t know how refine that further. As I mentioned, I discovered after the fact that the place where I had prescribed them most often was in patients in therapy for PTSD who had hard emotional times along the way. I think I was trying to help "dampen" their emotions, but I wouldn’t have known to say that at the time.
As a baby boomer, I took a few recreational drugs when I was younger and better able to recover from their effects. From my experience with psychiatric drugs, which ultimately was disastrous but, compared to many, limited, I can personally say they behaved like any other psychoactive substances, but not as much fun.
Even with antidepressants, initially there’s a rush and you can feel them coming on. As a good little patient, I took mine regularly and this wore off, leaving only a complacent feeling and the side effects.
Benzos, of course, are downers, so it’s perfectly obvious why people develop a liking for them.
I never tried any of the meth analogs, but you can see clearly why students trade ADHD drugs just like we did with speed. Bonus — they’ve learned how to snort them like proper street drugs http://www.grandforksherald.com/content/chase-ultimate-high-students-are-indulging-deadly-duo
In short, the only differences between psychiatric drugs and recreational psychotropics are that you get psychiatric drugs through a doctor and you get psychotropics from the guy down at the park, and given the opportunity, most people in search of a high would go with recreational psychotropics.
However, in a pinch, in a culture where getting high is common and the government is paying for the drugs, psychiatric drugs will do. They’re a lot more convenient and socially acceptable, too.
(One might expect when marijuana is legalized — which I would like to see — requests for psychiatric drugs will go down.)
I’m not saying the people who ask for psychiatric drugs intend to get high off them, what I’m saying is an altered mental state (as Moncrieff so aptly put it) is familiar and desirable to them. (Plus there are all the other drivers Dr. Mickey described above.)
As for, say, antidepressants “working” for PMDD and other ills: The reason is that antidepressants are hormonal disruptors. The sexual side effects are proof. Some people experience the hormonal disruption as beneficial, some as detrimental, and some don’t feel anything at all.
(That doctors think every hormonal stage of a woman’s life is a pathology that requires medication, in my opinion, a crime against humanity. I beg any doctor reading this not to prescribe psychiatric drugs to women for PMDD, post-partum depression, or menopause symptoms. Yes, I know there are extreme cases. Please figure out another way to treat estrogen imbalances.)
That antidepressants and other psychiatric drugs affect so-called neurohormones and not regular hormones is one of those pleasant lies physicians tell themselves. Would you throw out long-term prescriptions for steroids like candy? No? Well, why are you throwing out long-term prescriptions for serotonin reuptake inhibitors?
I submit: Psychiatric drugs taken chronically differ from steroids only in that the degree of observable physical symptoms is less. Otherwise, they are all deliberate dysregulation of normal hormonal processes and it’s the health of the patient that pays the price.
Here’s an interesting paper from 2012 that takes an evolutionary perspective on this class of drugs, and has some tough conclusions. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3334530/pdf/fpsyg-03-00117.pdf
Maybe it’s time to consider the dynamic meaning of medications. There are papers in the analytic literature:
Medication as Object
http://www.pep-web.org/document.php?id=apa.054.0781a&type=hitlist&num=0&query=zone1%2Cparagraphs%7Czone2%2Cparagraphs%7Cauthor%2Ctutter%7Cviewperiod%2Cweek%7Csort%2Cauthor%2Ca#hit1
Also, Adelman, S.A. (1985). Pills as transitional objects: A dynamic understanding of the use of medication in psychotherapy. Psychiatry 48:246-253
I can’t find the Adelman article, but the idea of an antidepressant as a transitional object, neither self nor other, but something in-between, and necessary, is intriguing.
I like Dr. Moncrieff’s concept. Working with 50+ year old well educated professionals this explains much of their behavior. They make no secret of their antidepressant use and have an expectation of special treatment. I also often question their logic as it seems to be impaired.
A drug centered model fits the behavior; otherwise I am dealing with a group that mimics 15 year olds who are too old to spank, yet old enough to know better.
Steve Lucas
PsychPractice
I think I read that article in ancient history. I can’t find it either. It is certainly a familiar dynamic. When I’ve suspected its presence, I’ve tried to move things to a safer Teddy Bear. Transitional objects are owned by the child, and given up when they’re good and ready, not taken away. So if it’s a pill, it should be a benign, soft cudly pill, not one that’s a wolf in sheep’s clothing…
Joanna Moncrieff’s conceptualization has been of enormous import to me. It is now how I think about all of these drugs. It comes easy to us when we think about a group like the benzodiazepines. We do not believe this only impact people with anxiety or sleep troubles. They impact all of us and those effects may be advantageous to some.
All of this fails to take into account the fact that the majority of the *patients* who continue to take the drugs feel that they benefit from the drugs. That’s why they continue to take them. They are not experiencing “addiction” because physical dependence is not addiction— addiction is compulsive use of a drug despite negative consequences. If the consequences of a physical dependence are positive (say, taking insulin to survive with diabetes), it is not an addiction.
What is missing here is any sense of individual variation. Some people *actually benefit* from being a bit numb. If you go through life with your senses set on high and your emotions completely dysregulated due to their extreme intensity, turning the volume down is not going to make you insensitive, it’s going to make you normally sensitive, AKA, able to function without crying when you see a commercial about families being nice to each other and able to move around in the world without being overwhelmed by loud sounds and bright lights. It will make you capable of actually being kind to others, rather than being so distressed by their distress that you have to go away and soothe yourself.
That is my experience with SSRI’s: they mitigate oversensitivity. If you are under-sensitive, they may well feel awful and do harm. But pretending that everyone has the same experience of a particular drug and saying that therefore these drugs are no different from placebo ignores both the data (where you can clearly see some people getting dramatically better and others worse when you look at particular patients) and clinical and personal experience.
It’s like opioids: some people find them immensely attractive and other people find them aversive (probably for some of the same reasons: they do counteract overly intense emotional experience and that’s helpful to some and harmful to others) and many people find them “meh.”
If you try to simply merge all the data, you may find that they are no better than placebo (and indeed, even some trials of opioids for pain find this, even though it’s very clear they are the best painkillers we have) but you will not be representing reality and will be doing depressed people a disservice.
Why can’t we recognize that drugs aren’t “good” or “bad” inherently but good or bad for a specific person at a specific time? And if these individual variations affect drug response (which they most obviously do), the distinction between the “disease” model and the “drug” model is not very interesting. The pharmacological effects vary based on the person’s baseline: you might call an oversensitive baseline a “disease” or you might call the alteration a “drug effect” but what results is that the person is more comfortable and functional.
Sandra,
I think I always thought that, since Internal Medicine days. Saying it out loud [“these are symptomatic medications”] got me in big trouble in the 1980s at the dawn of the modern era, and had something to do with my exit from academia. Those were the salad days when the catecholamine/serotinergic hypotheses were in full swing. Dr. Moncrieff has a good way of saying it. I’m surprised more people haven’t pick it up…
Maia,
That’s why I want an outside opinion [from Mars]. All the craziness with drug companies and KOLs has us so polarized that the drugs really do fall into a “good/bad” dichotomy that doesn’t do any of us a bit of good. What I notice is that any mention of these drugs is interpreted as “good” or “bad.”
I liked the New Zealand survey because they ended up with what seems more like what patients I ask actually say in person than much of what I’ve read. Maybe when these things finally go completely off-patent, we’ll figure out what they really are and where they fall in the pharmacopeia.
I’ve seen people using antidepressants for recreation, and I. don’t. even.; but perhaps they were getting a hypomanic high?
This. What makes me distrust psychiatry the most is that “it” continues full bore to find a biological cause for their unscientifically supported taxonomic categories while doing little to nothing to understand the biological actions of the medications they are using, some of which they use to diagnose people according to their reaction. Got manic— they’re bipolar. Felt better— they’re depressive. Double blind studies wouldn’t cut it, they would need to study with the fewest preconceptions they could muster and “they” would not be psychiatrists, but input from psychiatrists could help and, if possible, psychiatrists could learn something from studies based on biology and chemistry. Funny that— what’s most directly biological, the “it” is ignoring.
If a drug helps in a crisis, it helps. For people who have to keep slugging just to keep their heads above water in a life that is antithetical to mental health, then maybe dulling their feelings is the most that could be done to make their lives tolerable. Or maybe not being on an antidepressant is what keeps them from killing their boss. Who knows? But informed consent should include all possible effects, and should also include a disclaimer that mental illness is NOT a biological illness and the drugs DO NOT treat some indogenous chemical imbalance by rectifying it. Social services could help some reach a place in their life in which they can climb out from under some of their problems. Much misery in our society is structural and at some point that needs to be acknowledged when confronting people in psychic and/or emotional distress.
What amazes me most is the number of solidly middle class people (mostly liberals) who have swallowed the whole “it”, hook, line, and sinker so that any dissent is taboo. They think they’re helping when they tell other people to see a psychiatrist and try utopiazine. I’d love someday to read someone’s thesis on this phenomenon, I imagine there’s a socially psychology at work for most of them that would be quite interesting to learn about.
Also, Maia, part of the point here is that not everyone is more comfortable and functional and when that happens there is often a failure to take into account drug effects. It is too often viewed in the context of a illness that is not adequately treated. Side effects are often seen in that context as well (and here I am thinking more of negative symptoms of schizophrenia vs long term drug effects).
Obviously, if someone isn’t doing well, they need help and the medication needs to be considered a potential part of the problem, in case it is.
But what I hear all the time is that anyone on antidepressants who thinks they are doing well must be deluded because it’s “all placebo” or “addicted” and fearing withdrawal— and as an actual former heroin addict who knows from withdrawal, I think that’s pretty absurd. Withdrawal can suck, no doubt about it, but once it’s over with it’s over with— with antidepressants, there’s no association between “I take this and I feel good” for the vast, vast majority of people since it generally takes a few weeks to really have an effect. What that means is that there’s no craving: once you are withdrawn, you don’t find yourself longing wistfully for the antidepressant because the learning of “I take a pill” and shortly thereafter I feel better doesn’t occur. This is why people forget to take their Prozac, but I have never known a heroin addict who forgot to take their heroin!
Moreover, most heroin addicts I know have gone through withdrawal repeatedly: you don’t see people “craving” antidepressants once they have completed withdrawal and “relapsing.” What you see are people who discover that they are more functional on the drug than off— rather the opposite of what occurs with addiction. (For some people, however, opioid maintenance for addiction proves more effective than abstinence, and this is because what has occurred is that simple physical dependence has replaced addiction).
While there are surely idiosyncratic reactions, the idea that you can get high on SSRI’s is pretty ridiculous: they meet none of the standard tests for abuse potential (ie, neither humans nor animals generally “like” or will “work” for them when administered acutely).
And, really, how could mental illness *not* be biological? *Everything* must be biological at its root, unless you want to believe that the mind does not reside in the brain. That doesn’t mean that culture and psychology don’t matter, but they must ultimately translate into biology otherwise they cannot have an effect. So, the debate over this is like saying “no one can have a hardware problem” in computers, the problem is always software. For some people, mental illness *is* biological and drugs sort it out. For others, it’s more complicated. But to say that it’s never biology is simply incorrect.
The interpretations of the New Zealand survey are like an actually effective Rorschach test: the people who want to see them as evil point out the high level of side effects and ignore the fact that the vast majority of patients believed that the drugs were helpful. The people who see them as beneficial point out the majority, but at least in my cast, I do not deny at all that there are some people for whom these drugs do more harm than good.
I’m the first person to say that personal experience and anecdote are not data— but it’s clear hear that you can’t entirely ignore subjective experience and say that millions of people are simply deluded. It makes much more sense to think that some benefit and some are harmed and this washes out in the data and looks like placebo.
Re – “What do these drugs really do? How do psychiatric drugs work?”
This text published in 2000 is the best, most comprehensive answer to this question to date: http://www.amazon.com/Introduction-Behavioral-Pharmacology-Thomas-Byrne/dp/1878978365 – and it is now available on Kindle for $36.87. Far from an easy or simple read. May seem from Mars. May enlighten!
Maia, You wrote above and in one of your articles about the variability of response and how one’s perspective influences how one thinks about these things. I think this applies to this discussion. You report a good response to antidepressant drugs. Mickey’s experience mirrors mine and that of many of our colleagues – there are quite a few people do not seem to be much better with the drugs yet want them and want more added on. It is a peculiar phenomenon.
I went to ask for an SSRI in the end of 1990’s. At that time, the use of SSRI was far behind USA here in Finland. I think I actually had relatively severe depression, anxiety and social phobia at that time, much worse than many who eat these drugs, yet the general doctor refused to renew the prescription after a short trial, and later an older psychiatrist tried to talk me down about using them even though I insisted they help a lot. How much different was the attitude I received some years ago when I again contacted psychiatry!
In any case, yes, I’m certain that at that time I at least thought SSRIs helped me. In retrospect, I’m still not sure if they “helped”. I can easily notice the effects of a small dose of an SSRI on my experience the same day. I can definitely notice the “numbing” sexual effects, especially related to achieving orgasm. It does cause a clear altered mental state for me. It may be that in some sense, SSRIs helped me at that point of time. I was stressing myself with university studies, work, life, not so good lifestyle, etc. Perhaps one effect of SSRI on me was that it kind of prevented the strongest negative states of mind, or perhaps in a way kept my head floating above water in all kind of storms. Since then, I was on and off SSRI on different occasions, and later on the experiences weren’t that good anymore. It’s quite possible and even likely that I kept on going back because of the positive seeming experience at the very start.
It’s also possible that SSRIs during the first year kind of helped in getting back from the “rut” by somehow enabling me to build some new habits or outlooks. However, with time more and more negative stuff without benefits became evident. Both starting and stopping SSRIs several times has also confirmed me that they modulate hormones/cytokines through some mechanism which may have a great effect on mental stuff (see, for instance, cytokine/inflammation theories of depression and other mental illnesses). There may be some hazy ground around here with drug/illness models.
It has also been my experience that a subset of patients takes a simple mechanistic view of mood and antidepressants. I.e., if they feel worse, perhaps just for a day or two, the medication “stopped working” or they tell me they “need more.” Such a view isn’t unexpected in a culture that peddles quick cures on tv ads, and the best response I can offer personally is respectful education in the office. I agree with PsychPractice that the dynamic meaning of meds takes this one important step further; it’s an issue we address in some depth in the residency training program where I teach.
The polarization described by Mickey and Maia Szalavitz is very real and very unfortunate. For every “survivor of psychiatric abuse” there are others extolling the virtues of the very same treatment. As a field and as a culture we need to find a way to see beyond the polarities. An objective Martian would be nice. In the meantime I suggest humility in the profession about what we know and what we can change — Dr. Moncrieff’s view is a good corrective. And equally, a recognition by critics that psychiatrists are fallible fellow humans who are trying to do good with blunt tools in a complex field, and that despite all of this we actually help a great many people. We won’t all join hands around the campfire, but at least we can treat each other civilly.
For what it’s worth, I heard 20 years ago that SSRIs “put a barrier between you and negative [and sometimes positive] feelings.” In the years since, I’ve heard this subjective report from a few patients. Most report no such altered state, which may mean that Dr, Moncrieff’s formulation is mistaken, that the altered states too subtle to notice, that my sample is atypical, or something else.
Steven,
I think you may be misinterpreting with Moncrieff means by “altered state”. The point she makes is that the drugs do not correct an altered state but “work” by changing the brain,i.e., in a concrete sense the brain is altered. She is challenging the notion that we understand what is “wrong” in the brain and the drugs bring that problem back to “normal”.
In reading the comments and some other material I have to wonder if the long term use of antidepressants do not create an ever changing emotional landscape for the patient and doctor. This would explain some of the patient responses and I feel add additional support for Dr. Moncrieff’s position.
A person’s psychological make up is not static.
Steve Lucas
With all due respect, Maia Szalavitz, you need to know more about antidepressant withdrawal syndrome. See case reports here http://tinyurl.com/3o4k3j5 It’s not heroin withdrawal lite.
If you’re going to prescribe a pill as a “transition object,” why not prescribe fish oil? Most people would benefit from it anyway because omega-3s are lacking in our diets. And there is no difficulty in stopping it.
As I’ve said before, psychiatric drugs are psychotropics. They’re like MDMA or LSD toned down to be taken daily. Like MDMA or LSD, some people find their effects beneficial, some detrimental, some feel nothing, and others are crippled by extreme adverse reactions.
In fact, when I took 20mg Prozac, which proved to be too strong for me, I was speed-talking and joking like someone who was high.
(Doctors — Patients who don’t like the drugs you prescribe leave your practice. Do you think this could be contributing to your sense that the drugs are so frequently beneficial?)
Seeing psychiatric drugs for what they are allows for the spectrum of attitude towards them, but demystifies them. They possess no magical therapeutic qualities. Basically, you’re lobbing a chemical grenade into the nervous system to shake it up, hoping the fallout is good.
Correct if I am wrong, but I haven’t seen the social aspect addressed so far. Steve touched on it a bit with the negative aspect of playing the sympathy card for the illness of depression. But, there is another side to this, and perhaps it is, taking a medication to legitimize their condition to others in their lives and maybe even to themselves.
This thought doesn’t track well to an anonymous survey, but it may be an important item in your real world interactions with patients. In this culture, there is an extreme prejudice against talk therapy with it being seen as only for the weak. And even with physical illness, if you are not under a doctor’s care and being treated with something, then there is nothing really wrong with you except that you are a malingerer. So, some patients may insist on them or be wedded to them for what it represents in their sick role, whether for good or bad.
I’m sure for some patients, everyone they know is taking some psychiatric drug.
Altostrata – I agree with you, yet I mean a different type of peer pressure. One where a person endures taking a medication that doesn’t work because it is the only way their illness is validated.
Anti-depressants are anti-feeling medications. And that’s good for some folks; maybe not so good for others.
I never said antidepressant withdrawal was heroin withdrawal lite: I said that heroin withdrawal is over-hyped and that having been through it multiple times, I know that it’s *not* the reason heroin addicts relapse and the vast majority of addiction experts now agree. If simply getting through withdrawal cured heroin addiction, you could lock people up for its duration and they’d be all better. But that’s absolutely not what occurs. Most people manage just fine getting through withdrawal (particularly if they are somewhere where they can’t get drugs)— instead, they relapse well after withdrawal has resolved. In fact, during acute withdrawal, it’s really hard to relapse because you feel so lousy you don’t want to deal with anyone!
It’s when you feel better *afterwards* when you think “I’m not an addict, I’ve just kicked, I can do it just on weekends” that you are at risk. And that thinking simply doesn’t happen with antidepressants. When you get through withdrawal, either you feel better and you are like “whew, glad that’s done” or you still have the problems that made you take the drug in the first place and may discover that you need it or something to avoid depression relapse.
Either way, it’s simply not analogous because you don’t *crave* the antidepressant experience. You want to feel normal and OK, which is part of what you want after heroin addiction, but there is *also* a craving for the high which is entirely absent when you cease antidepressants because they simply do not produce the same type of euphoria.
Maia, you still need to learn about antidepressant withdrawal. Your assumptions about parallels to heroin withdrawal are incorrect.
Arby, I agree with you, some people find drug treatment to be validating — they always knew there was something seriously wrong with them.
I think that the following studies get us closer to understanding the actual effects of SSRIs:
http://www.ncbi.nlm.nih.gov/pubmed/10616614
http://www.ncbi.nlm.nih.gov/pubmed/19996037
Altostrata, if you are talking about the fact that taking ADs validates that there is something wrong with the ADs, again a different issue. I would think that the people taking ADs that have validated that they are terrible would be intelligent enough to get off of them, yet there are quite a few who are not.
I offered a sociological reason besides the business reason of advertising and get-better-quick-with-a-pill thinking in this culture as a possible explanation. If you can’t see that there is pressure on people to take an AD, not just from their doctors or their own need, but rather from others in their lives, then I can’t explain it to you. You’ll miss something in your thinking though, and what will slip through is that even if you go ahead and banish AD’s to the dust bin of history, the way we live now, another drug will just take its place.
I agree with you, Arby.
I would go further and say that the fracturing of traditional community and the way many people live in isolation is very much at variance with the human need for emotional connection and stable social context. Add to this the artificial and stressful work environment, and you get a need for drugs that will relieve anomie.