by Maximilian Huhn; Magdolna Tardy; Loukia Maria Spineli;Werner Kissling; Hans Förstl; Gabriele Pitschel-Walz; Claudia Leucht; Myrto Samara; Markus Dold; John M. Davis; and Stefan Leucht.JAMA Psychiatry. Published online April 30, 2014.
IMPORTANCE There is debate about the effectiveness of psychiatric treatments and whether pharmacotherapy or psychotherapy should be primarily used.OBJECTIVES To perform a systematic overview on the efficacy of pharmacotherapies and psychotherapies for major psychiatric disorders and to compare the quality of pharmacotherapy and psychotherapy trials.EVIDENCE REVIEW We searched MEDLINE, EMBASE, PsycINFO, and the Cochrane Library [April 2012, with no time or language limit] for systematic reviews on pharmacotherapy or psychotherapy vs placebo, pharmacotherapy vs psychotherapy, and their combination vs either modality alone. Two reviewers independently selected the meta-analyses and extracted efficacy effect sizes.We assessed the quality of the individual trials included in the pharmacotherapy and psychotherapy meta-analyses with the Cochrane risk of bias tool.FINDINGS The search yielded 45 233 results.We included 61 meta-analyses on 21 psychiatric disorders, which contained 852 individual trials and 137 126 participants. The mean effect size of the meta-analyses was medium [mean, 0.50; 95%CI, 0.41-0.59]. Effect sizes of psychotherapies vs placebo tended to be higher than those of medication, but direct comparisons, albeit usually based on few trials, did not reveal consistent differences. Individual pharmacotherapy trials were more likely to have large sample sizes, blinding, control groups, and intention-to-treat analyses. In contrast, psychotherapy trials had lower dropout rates and provided follow-up data. In psychotherapy studies, wait-list designs showed larger effects than did comparisons with placebo.CONCLUSIONS AND RELEVANCE Many pharmacotherapies and psychotherapies are effective, but there is a lot of room for improvement. Because of the multiple differences in the methods used in pharmacotherapy and psychotherapy trials, indirect comparisons of their effect sizes compared with placebo or no treatment are problematic.Well-designed direct comparisons, which are scarce, need public funding. Because patients often benefit from both forms of therapy, research should also focus on how both modalities can be best combined to maximize synergy rather than debate the use of one treatment over the other.
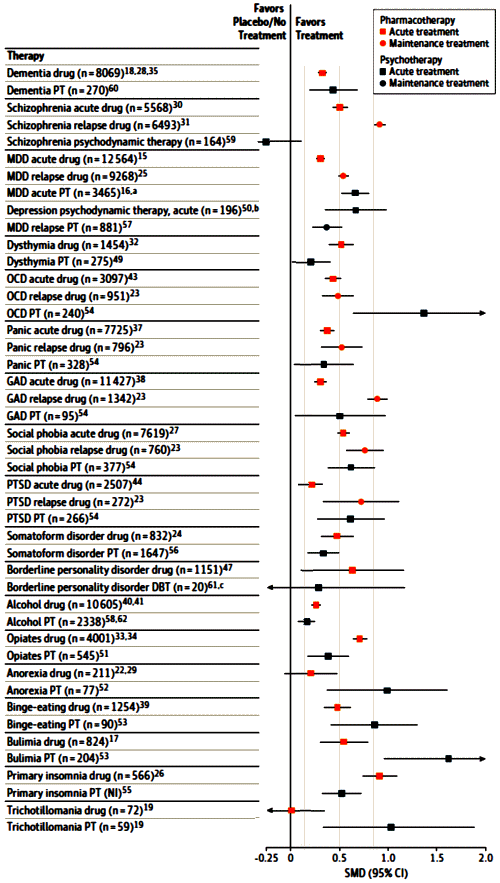
This study was a huge undertaking and the methodology deserves a thorough look-see in the coming days, but just scanning their results, it looks like an important resource in addressing these recent confusing years. The scale at the bottom [standardized mean difference] is the difference between the means of two groups divided by the standard deviation of the pool of participants. Expressing the effect sizes in this way allows studies using differing measurement instruments to be compared. If the horizontal lines [95% Confidence Limits] don’t cross 0, the difference is significant. In general, an SMD of 0.2 is small, 0.5 moderate, and 0.8 is large. The authors caution that the methodologies of the drug and therapy studies are different enough to invalidate direct comparisons of magnitude between the two.
Leucht and his collaborators do an excellent job. Their meta-analysis in the Br. J Psychiatry on the comparison of psychiatric versus non-psychiatric medications was first rate:
http://real-psychiatry.blogspot.com/2012/02/critical-article-on-efficacy-of.html
As an editor, I was glad when they took up my challenge to respond to Ioannidis (reference 3).
Thanks to both of you. Dr. Dawson I also very much enjoyed the blog you linked and the sources on that page. If either of you are interested, I would be interested in your views of the questions that have been nagging at me. While the effect sizes for drugs for both acute treatment and prevention of relapse in schizophrenia are large, I am still not sure we are understanding what that actually means. For instance, in the acute setting are we targeting something specific about schizophrenia (or even psychosis) or do they have some general psychoactive effect that happens to be helpful for people who are experiencing psychosis? In the relapse phase, are we seeing a recurrence of the underlying condition or are we seeing the effects of withdrawing a drug that has sensitized the brain so the relapse is at least in part due to the withdrawal? To anticipate a response, I would add that one might still choose to use these drugs regardless of the answer to these questions; the answer nevertheless could influence practice in a number of ways. I realize that this may not be a primary interest for either one of you but if you happen to take it up, either here or in a personal communication, I would be interested in your perspective.
I spoke to a young psychiatrist on Tuesday who specializes in “treatment-resistant depression” (heinous term). Independently, he concluded he was seeing a lot of iatrogenesis and he wanted to talk to me about withdrawal syndrome patterns, particularly prolonged post-acute withdrawal.
He said he’s sent some of his patients to my Web site (peer support for tapering and withdrawal syndrome, http://SurvivingAntidepressants.org). “They’ve found symptom patterns that fit them to a T,” he told me.
He asked me if I would speak to a group of his colleagues, who are seeing similar patterns in their clinical practice. Of course I said yes.
I hope this indicates a trend: These young psychiatrists, who perhaps don’t suffer from the cognitive dissonance of those who have been prescribing psychiatric drugs for upwards of 30 years, are paying attention to what’s going on with their patients and seeing patterns of injury that patient advocates like myself have been carrying on about for many years.
Of course, should psychiatrists be relegated to playing telephone with primary care physicians in the APA’s new “integrated care” scheme, this observational experience will be lost.
Also, it looks like the above review surveyed only published studies, which have been massively engineered to show benefits for psychiatric drugs.
Alto,
Great news. The patients I’ve sent to your site say the same things…
You’re not just teasing me, are you, Dr. Mickey?
nope…
Looks like I might have defined post-acute psychiatric drug withdrawal syndrome and redefined “treatment-resistant depression.”