I work in a fairly unusual charity clinic, one that only has one paid employee – a Director. The place is teeming with volunteers, most of us with grey [or little] hair – many living in retirement communities nearby. The doctors who started the clinic had an amazing vision, so we have a pharmacy stocked with donated samples and some purchased medications. And there’s a group that is skilled in getting patients with individual medical needs their medications through the indigent programs of the drug companies. In addition, this group helps patients seen elsewhere [mental health centers] get in-patent medication. Another group arranges for patients with specialty needs to be seen by doctors in the community where possible [by begging], or set up tests that we can’t do [like EEGs or MRIs] elsewhere [also by begging]. Their skills in getting people taken care of are remarkable. Some of the local docs volunteer too [eg a diabetic clinic].
I saw a woman Friday who has been followed in a State contracted Mental Health Clinic in a nearby town. She developed a psychotic illness in her mid-fifties with agitation and persecutory delusions. She was hospitalized with a diagnosis of "Schizophrenia" and treated with Geodon® [Ziprasidone], an Atypical Antipsychotic, which she has taken continuously for six years. She saw me at the request of our pharmacy staff for an "administrative" matter. Our pharmacy has been able to supply her with the medication through an indigent program, but is no longer going to be able to do that. She has a nine month’s supply, but they can get no more. So she came to see me to find an alternative. She’d thought about Risperdal®. In the original hospitalization, they had tried Seroquel® [she made an it-made-me-sick face as she said it]. She had taken 60 mg daily since being hospitalized, but the dose had recently been lowered [at her request] to 40 mg. She still had some "60’s," and was "taking them up" before going to "40s." She said she could never afford to buy it herself at "$300/a month" at the pharmacy. Her husband had died in the recent past and she lives alone. She said with a grin that if I picked "too high a dose," she’d know it ["I’ve got the Internet"] and wouldn’t take it. I admired her spirit [putting me in my place, not knowing I was already there].
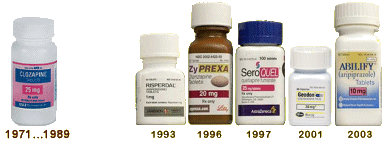
If it were just an "administrative" matter, it wouldn’t be a big problem. The local pharmacies are as helpful as the local doctors and our volunteers. The reason we can’t get it for her anymore is that the patent on Geodon® ran out, and along with it, the indigent program shut down. The Generics are now available and with the discounts and the good will of our local druggists deferring their profit, it could be purchased for $55/month. It is likely that I could get the pharmacy at our clinic to get it for her with discretionary funds at that price. But it’s not just an "administrative matter." First, "Schizophrenia" with a first episode in her mid-fifties? Sounds odd to me. And she’s had no symptoms since that hospitalization. So was the diagnosis "Schizophrenia?" I don’t know that but have my doubts. When I saw her, the focus was on her meager finances, as well as staying on a lowest possible dose. She also mentioned that she had tried going off of it altogether, but couldn’t sleep without it. She seems to have been followed as if lifelong-medication were the standard treatment, and we’re not thinking that anymore – at least I’m not. But that’s not the whole story.
She has early Tardive Dyskinesia [TD]. It’s subtle, but it’s noticable if you know what it is – fingers, a little in the face. So from my point of view, the imperative at this point is to begin to taper her off of the medication altogether. She was the last patient of the busy day and the clinic and pharmacy staff had all left. So I encouraged her to go ahead and go down to the 40 mg dose, reassuring her that we would take care of all the administrative matters. There are domain issues as she’s not really our patient and if we’re going to taper her, I’ll need to get some lower dose capsules. But those kind of "administrative" matters are do-able. I’m obviously mentioning the case here in relation to the recent discussions of the treatment of psychosis and the medications used.
In my first medical life, I was a Clinical Immunologist, which meant treating diseases of unknown etiology [like Rheumatoid Arthritis, Systemic Lupus Erythematosis, etc] and it was the early days of organ transplants. We used some mighty toxic drugs in those days – steroids, anti-inflammatories, immunosupressives, antineoplastics – poisons. The consequences were potentially dire, but the alternatives were even worse. Getting people off the medications was always part of starting them. Toxic drugs like those could often be used safely short term, but were long term nightmares. Every case was a rock and a hard place. That’s just how it was. That’s still kind of true in that field, though they have a lot wider [and safer] range of drugs to choose from these days – but the risk/benefit ratio remains a constant watchword [just listen to those mumbled warnings at the end of the t.v. ads].
I think that mentality came with me when I came to psychiatry. In Rheumatology, I’d learned the concept that every single pill was a therapeutic trial, and we saw people frequently to see how the endless trials were going. Coming to psychiatry and encountering the neuroleptics of the 1970s was no different to me. Acute psychosis was a show-stopper and antipsychotics "worked," but the medications long-term were toxic [as in Tardive Dyskinesia as one example]. It felt familiar to me – just another rock and a hard place as a part of a medical life [those double binds I was talking about in part one: the bind…]. I was fortunate in having teachers who taught that these were symptomatic medications and they were in the lowest-effective-dose-drug-holiday-when-possible mindset of the day. Most of the people who pushed the notion that our job was insuring endless medication compliance or using depot injections were not psychiatrists, but rather administrative types trying to keep people out of harms way [and out of the hospitals]. By temperment,  I might have fallen into the no medication set, but by experience following some of these patients long term, I am planted in judicious-use-of-medications-and-supportive-psychotherapy where I will likely stay. Like in Rheumatology, I use the medications when I have to, and aim for less or none when I can – another rock and a hard place as a part of a medical life.
I might have fallen into the no medication set, but by experience following some of these patients long term, I am planted in judicious-use-of-medications-and-supportive-psychotherapy where I will likely stay. Like in Rheumatology, I use the medications when I have to, and aim for less or none when I can – another rock and a hard place as a part of a medical life.
So I agree with Robert Whitaker’s campaign against medications-for-life, though the anti-medication-altogether meme seems ill-informed to me. When the Atypical Antipsychotics were introduced, it was hoped that they were not going to cause the long-term neurological problems, but that turned out to be untrue as in this case. I personally think this patient has been ill-advised in that the medicine has been continued for six years – an older patient [more prone to Tardive Dyskinesia] with no apparent attempt to get her off [even though she is asymptomatic]. I’ve seen patients like this who have tried to stop it themselves, but had symptoms that interfered [like insomnia] and so they continued it. I would suspect in this case that those symptoms may well have been from withdrawal and might’ve been managed by a slow tapering and help with safer medications for sleep if needed, but that’s not what happened. In addition, TD can sometime worsen when the medication is withdrawn [another rock and a hard place]. Sometimes it goes away with stopping the medications – sometimes it doesn’t.
There are a number of forces perpetuating the medications-for-life idea. Our KOLs certainly haven’t been much of a help in alerting people to the adverse events. The drug companies made money from the number of pills sold so medications-for-life is not something they would discourage. Rather, they’ve actively minimized adverse events. Families, doctors, law enforcement officers, and staff who live in the revolving door world get very burned out by the patients who stop their medications on discharge and keep showing up every few months with recurrent psychosis. Insurance companies, families, and public mental health centers aren’t keen on the costs of repeated hospitalizations so they tend to advocate for staying on medications. Back in the day, when one or another of the psychiatry residents was showing signs of that kind of frustration, getting angry when patients stopped their medications, I often suggested that they try a dose themselves one free weekend. Some took me up on that, and slept the weekend away. One said he felt like "a tree." The point is that the patients are between a rock and a hard place too. Antipsychotics are no fun to take.
This is the first case of Tardive Dyskinesia I’ve seen in a long time. I’ve not practiced in a situation where I would see it a lot, but I’m still surprised at how little I’ve seen. The case reminded me that that this is where I came in forty years ago. The drugs were different then [first generation], more toxic, but the music was the same – the same rocks and hard places, the same impossibilities. Then, we worried about the mental patients confined to State Hospitals. Now, we worry about those in State Prisons. The opinions about neuroleptics was similarly polarized though the divisions cut along somewhat different lines – more within specialty groups in 1974 rather than between them now.
More to the point, what are the differences between 1974 and 2014? the differences between those first generation antipsychotics and the Atypical Antipsychotics of the modern era? Well, underneath all the drug company propaganda, there’s some actual data:
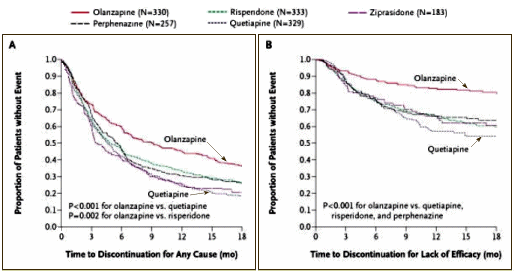
[C.A.T.I.E.]
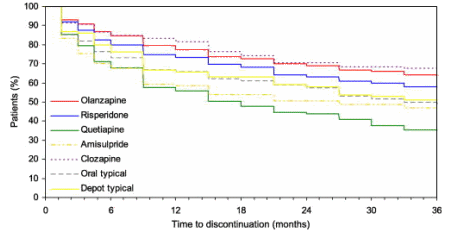
[European Schizophrenia Study]
And also this from that European Schizophrenia Study:
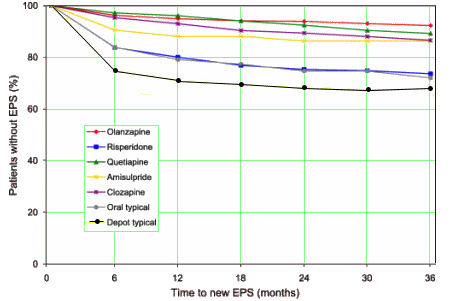
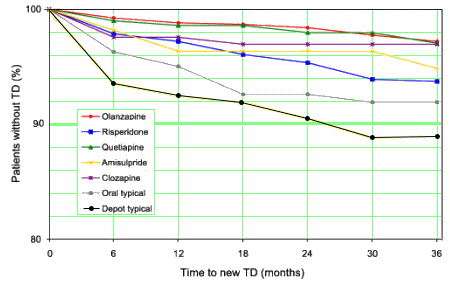
At least in the area of neurologic Adverse Effects, there’s been some demonstrable progress.
I’ve always thought it ironic that many KOLs [specifically Dr. Lieberman] stick to the line that medication compliance is a key, even using the term "neuroprotection" [see Neuroprotection: A New Strategy in the Treatment of Schizophrenia] [for the record, I don’t believe that Lilly-funded CME roundtable]. The irony is apparent in the discontinuation rate in Dr. Lieberman’s own NIMH C.A.T.I.E. study above, and in other studies like this one from the VA hospitals:
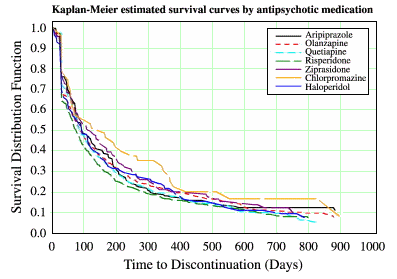
That’s certainly what I think, and hope for with the coming changes in parity, or the RAISE program, or its SAMHSA extensions – that it will allow these patients more face time. In the patients I’ve followed over the years, case management has been much more than about medication compliance. It has been about using the least amount of medication possible and learning with the patient how to live with the illness as it is manifested in their specific case. As I said, by temperment, I’d love to be in a medication free world and I read all the Open Dialog studies with great interest. But the lives of the patients trump my temperment, and so I live with the rocks and hard places and the double binds along with them – I worry when they’re on medications and I worry when they’re not. Such is my lot just like it was in Rheumatology. I personally think that if there’s something -for-life, it’s not meds, it’s periodic contact no matter how infrequent with someone who knows the case and can jump into action when it’s needed [In a crisis, I can do a hell of a lot better job with patients I already know than otherwise].
I would just add that in some cases these negative symptoms may be due to the long term use of the drugs.
Mickey,
I know someone who has been on APs long term and has severe adverse affects from them. For various reasons, i am convinced this person could be maintained at a very lose dose or taken completely off of the meds with a very gradual tapering program. But this person’s chance of finding a psychiatrist in his insurance plan are slim and none who would do that.
Regarding the woman who was diagnosed in her 50s with a first time psychotic episode, is there anyone in psychiatry who does any critical thinking and question these odd types of diagnoses? i realize regular doctors have a problem with this so I am probably asking a dumb question. All sarcasm aside, that was the first thing I thought of when you described this situation and am glad you came to the same conclusion.
Kudos to you for the work you do.
Also, thanks for posting the Hordern and Hamilton paper. I had not seen this. There is so much in it of value – the different approaches in the US and UK, the country differences in dosing, the mention of the so-called neuroleptic threshold. In the latter part of the paper, the authors mention a study by Hamilton and colleagues in which the positive effects of OT where hindered by drugs. This is echoed in the three RCT’s I have found that show worse functional outcomes with long term use of neuroleptics. We are now using neuroleptics for many more individuals whose problems are thought to fall under the wide umbrella of mood disorders. There is no data on long term outcomes and I believe there is reason to be concerned about this.
Sandra,
re the point about mood disorders. I think antipsychotics have been used in the “psychotic” states periodically since they came into being [eg Mania, Psychotic Depression]. But I really balk at their long term use in Manic Depressive Illnesses. It feels like an FDA Approval that has been “stretched” to cover long term use, implying that it’s a preventive. So I agree that this usage is highly suspect of industry influence rather than clinical wisdom…
The Hordern and Hamilton paper and the Vermont Studies you called to attention say the same thing to me. These patients need both. The “just medication” approach is a waek sister compared to a combined approach. It’s why I glaze over when the topic turns EITHER/OR. Psychotic Illness is psychiatry’s biggest challenge and something we know a lot about. To relegate patients with an illness that can be such a life changer to “med checks” seems like misinformed practice to me. These patients need all the help we can muster from both sides of the aisle. And I would fault the psychotherapy community as well as the biomedical community for not studying the effectiveness of interventions more thoroughly and systematically.
When I read your case history the question of a depressive episode arose in my mind. For some years I have pushed back against use of atypical antipsychotic drugs in depressed patients, especially when they are not psychotic. See PubMed ID 19142117 and PubMed ID 20007291, as well as Health Care Renewal here and here and here. The usual suspect KOLs keep pushing them, however… where is oversight from the APA?
Thank you for caring so much for your patients, Dr. Mickey.
And thank you for taking on gradually tapering these people off their drugs!
Upon further reflection, it seems that Dr. Lieberman’s talent in coining vapid pseudoscientific but slick promotional catchphrases such as “neuroprotection” made him the perfect President of the marketing juggernaut that is the APA. The National Association of Realtors must be jealous.
Many of the problems in psychiatry and medicine, and other disciplines are a result of a fossilized divisions in the academy, IMO. Our universities and professional titles are often more parochial than timely and adaptive. True and open exploration and observation tends to get lost in the publish or perish grind with it’s cronyism and territorial defensiveness.
http://somatosphere.net/2014/07/the-collaborative-turn-interdisciplinarity-across-the-human-sciences.html
I agree. Peer review does not work if academia is the Adirondack Club.
The quality of almost all psychiatric research since 1980 is abysmally poor.
It’s disheartening to see the decline in research in more objective fields like oncology.