New York Times: OpinionBy EDWARD LARKIN and IRENE HURFORDAUG 12, 2014Edward Larkin is a second-year medical student at the University of Pennsylvania, where Irene Hurford is an assistant professor in the department of psychiatry.
A few months ago, a patient came to our hospital, seeking help. One of us, Edward, was on the team that treated him. He was pleasant, if slightly withdrawn, and cogent. He was a college graduate in his 20s and had recently been fired from his job as a high school math teacher, because of unexpected absences. He had come to believe that government agents were conspiring against him, and he had taken to living out of a truck and sleeping in different parking lots. By the time he came to us, he was exhausted. A diagnosis became clear: he had . We admitted him to the hospital, and after a few days, with his symptoms under control, we released him. Unfortunately, we prescribed a medication for him that could cause significant, permanent harm, instead of an equally effective drug with milder side effects — all because he was uninsured.
Schizophrenia, which affects 1 percent of the population and emerges in the late teens to early 20s, is deeply misunderstood. People who suffer from it are often suspected of being dangerous, but this is not usually the case, and antipsychotic drugs are very effective. Our patient was exactly the kind of person who, with the right treatment, could have weakened the stigma surrounding schizophrenia. Antipsychotic drugs fall into two classes: the older ones, like Haldol, and newer ones, like Abilify and Latuda. Both classes are equally effective at treating some of the worst symptoms of schizophrenia, specifically the , delusions and paranoia that cause social alienation. [They’re not effective for treating “negative symptoms,” like low motivation].
But the older drugs can cause a multitude of serious side effects, including a potentially devastating one called . This condition involves unsettling, animalistic smacking and wagging of the lips and tongue. At its extreme, it can affect the entire body. It occurs in 20 percent or more of patients who take the drugs long-term, and it tends to start so mildly that patients can’t identify it in time to stop taking the drugs. It is often irreversible.
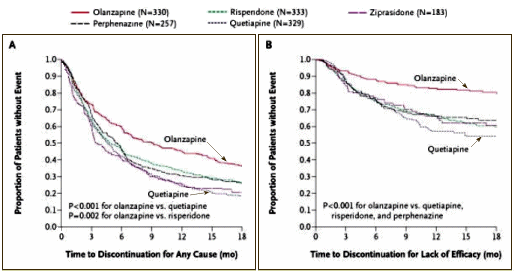
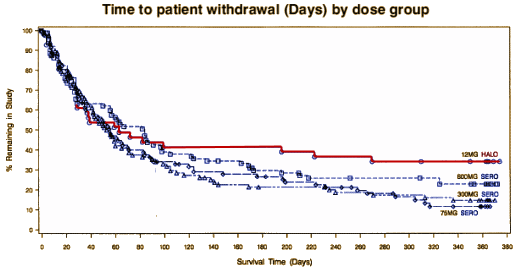
The newer drugs have lower rates of tardive dyskinesia [estimates vary, but most likely less than half or one-third the risk], although they can cause weight gain and predisposition to , among other side effects. The newest among them, however, have decreased these risks, too. And a 2006 study showed that patients were more likely to keep taking the new drugs than the older ones.
Note from 1boringoldman: This 2006 study is from a proprietary Insurance Claims database with the following financing and ghost? authorship: "This study was supported by AstraZeneca Pharmaceuticals LP. The authors would like to acknowledge the assistance of Anusha Bolonna, PhD [PAREXEL MMS], who provided medical writing assistance on behalf of AstraZeneca." [The article itself makes multiple pair-wise comparisons with no overall ANOVA to justify them, nor did it provide enough information to allow me to accurately estimate the overall ANOVA’s significance].As a result, most psychiatrists prefer the newer drugs, especially for younger people, and they should have been the clear choice for our patient. He didn’t have the luxury of choice, however, because he was uninsured, and he was explicit about the fact that he didn’t have much money to spend on medications. So we had to prescribe him Haldol, which costs about $20 per month, instead of one of the newer drugs, which can cost more than $600 per month. These issues will be amplified as progress is made in discovering the mechanisms of psychiatric disease, as it likely will be, thanks to the billions of dollars that are now going to neuroscience research. We can already see the results of that kind of investment in oncology, where extravagantly expensive specialty drugs are coming on the market. But as we make much-needed progress and develop new, expensive treatments that are clearly superior to old, cheap ones, we have to ask: Will those with the most to gain still receive a lower standard of care?
So while his point holds that we aren’t taking good-enough care of Schizophrenic patients, it’s not our using the older medications that’s the problem [in fact, there are generic Atypicals now as available as the first generation antipsychotics]. Our failure is in offering little more than medications to his young patient and vague hopes for some future breakthrough medication that will fix everything.
This was an incredibly depressing article. Clearly, this student is regurgitating what he has been told. As you note, the article is full of misinformation. But even if one buys “the new drugs are better” idea, this article makes no sense since almost all of the so-called second generation anti-psychotic drugs are now off patent. The give away is that he names Abilify and Latuda but fails to mention the others that are now off patent. Of course, as you say, the hype that these drugs are less toxic has not held up to review.
Looks like the NYT is up there with Fox News for BS. A 90 supply of either loa zapping or quetiapine at Costco would cost $30 to $40. That is less than the $20 per month for the Haldol they mentioned. So whether one thinks meds are the answer or not their argument has no merit. One could argue that Latuda and Abilify do not cause as much weight gain, but they did not make that point. And I have seen patients with weight gain on Latuda and akathesia on Abilify. The article is just another piece of Pharma propaganda, whether the authors realize it or not.
Oops did not notice my spell checker turned olanzapine into loa zapping. And who said AI systems lacked a sense of humor
I kind of like “loa zapping”…
Powerpoint is wrecking medical education.
My spell check’s choices for amitriptyline were “triphenylarsine”, “pantyliner”,
“nonlinearity”, “trampoline”, and “immaterialness”. All of which are contraindicated or irrelevant to nerve pain.
Maybe the spell checker had a Freudian slip there, eh?
Perhaps the spell checker for Freud would be “Frau Blucher”, Blazing Saddles fans get it!?
Oops, now i have to check myself! Should be a reference to “Young Frankenstein”! Don’t utter it around the horses!
Loa is a Haitian voodoo God. If your delusion was that Loa was responsible for first rank psychotic symptoms, Loa Zapping would be uncannily accurate.
However, it would probably only contain Loa by about 30-40 percent.