I’m sure we’re not out of drugs forever, but we’ve sure picked the low fruit, and then worked our way pretty far up the tree. A bit of mold on a petri dish kills staphylococcus; a new TB drug perks the depressed guys on the Chest Ward; a tweaked antihistamine that shuts down psychotic symptoms – that kind of serendipity is taken. And the hard work with similar compounds or similar pathways added some value, better tolerability. But the odds of an antipsychotic that isn’t neuroleptic are approximating zero. The same for an antipsychotic that improves negative symptoms. Many of us think that the symptomatic improvement of depressive affect may not have a much higher mark, particularly in patients with life/mind/social problems that transcend their biology. And how much more mileage is there in the war on serum lipids? This graph implies to me that we’ve passed the point of diminishing returns – probably even overshot:
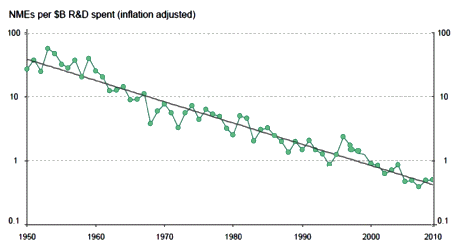
Click the graphic for the article
Edited for clarity
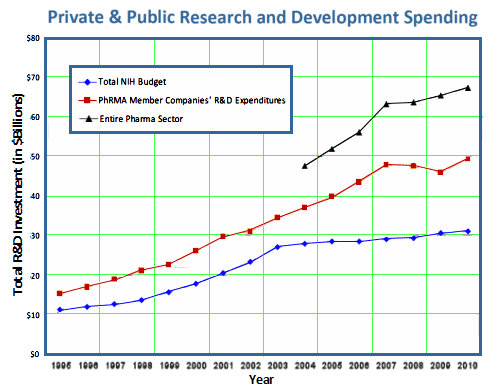
We’ve mined our current science, and we don’t really know if there’s a new next science that will add very much, at least any time soon. That’s what the PHARMA laboratories say and have been saying. I’ve had trouble giving their assertion proper valence because I’ve become so used to looking for the tricks in their words that I seem to have glossed over the main message [and there have been tricks enough to justify my skepticism!]. This next graph is from Janet Woodcock, MD Director, Center for Drug Evaluation and Research – FDA called "Today’s Biomedical Innovation: Lost in Translation?" In this slide, she makes clear that the PHARMA spending has not fallen off as much as the public spending – approaching close to $ 80 B/year:
In the summer of 2011, PHARMA essentially exited CNS Drug development [suddenly, last summer…] and the DSM-5 Task force was forced to admit that its planned biologically based DSM-5 was being scrapped for lack of evidence. Speeches were given; meetings were held [APF Convenes Unique Pipeline Summit], rants were ranted [Are future psychiatric treatments doomed?]. The neuroscience base was stalled along with drug development. Dr. Insel had long tried to keep the NIMH focused on biological research and treatments, and the NIMH went into high gear. The slide above is parodoxical in that it shows that the PHARMA resources far exceed the NIH Budget. The party line was that industry had stuck with ‘me-too’ drugs and that the NIMH needed to pick up the ball and intensify its drug research endeavors with creativity and innovation. Both Drs. Woodcock [top slide below] and Insel [bottom figure below] showed us how hard and expensive it was for PHARMA to develop a new drug. Notably, neither pointed out that their figures came from ‘the end of the line’ – when there were ‘slim pickings’ [see the first graph above]. Both saw the development of new molecules as the job of academic researchers, someone else who fell down on the job:
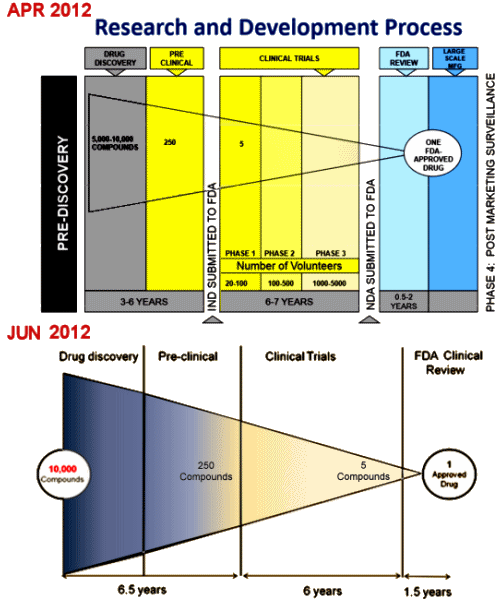
They were joined in this rhetoric by former NIMH Director, Stephen Hyman [hope and hype…]. Now it’s two years later and the NIMH leads us ahead with an RDoC [Research Domain Criteria] and an NCATS [National Center for the Advancement of Translational Science] with all kind of new, innovative, novel strategies [see rather than micromanage…].
An Editorialby H. Christian FibigerSchizophrenia Bulletin. 2012 38[4]:649–650.Psychopharmacology is in crisis. The data are in, and it is clear that a massive experiment has failed: despite decades of research and billions of dollars invested, not a single mechanistically novel drug has reached the psychiatric market in more than 30 years. Indeed, despite enormous effort, the field has not been able to escape the “me too/me [questionably] better” straightjacket. In recent years, the appreciation of this reality has had profound consequences for innovation in psychopharmacology because nearly every major pharmaceutical company has either reduced greatly or abandoned research and development of mechanistically novel psychiatric drugs. This decision is understandable because pharmaceutical and biotechnology executives see less risky opportunities in other therapeutic areas, cancer and immunology being the current pipeline favorites. Indeed, in retrospect, one can wonder why it took so long for industry to abandon psychiatry therapeutics. So how did we get here and more importantly, what do we need to do to find a way forward?
The discovery of all three major classes of psychiatric drugs, antidepressants, antipsychotics, and anxiolytics, came about on the basis of serendipitous clinical observation. At the time of their discoveries, the mechanisms by which these molecules produce their effects were unknown, and it was only later that antipsychotics were shown to be D2 receptor antagonists, antidepressants monoamine reuptake inhibitors, and anxiolytics GABA receptor modulators. It is interesting and perhaps instructive to consider whether any of these classes of drugs could have been discovered by current drug discovery strategies. For example, what genetic or preclinical data exist that point to the D2 dopamine receptor as a likely target for antipsychotic activity? Presently there are no genetic data that suggest that this receptor is expressed or functions abnormally in psychotic disorders. And without the benefit of the prior clinical validation, it is difficult to see how preclinical data alone would point to the D2 receptor as an interesting potential target for the treatment of psychotic disorders. The same can be said for monoamine transporters with respect to depression where, like psychosis, there are no animal models based on disease pathophysiology and no compelling preclinical data pointing to these as potential targets for antidepressant drugs. This raises a troubling question: if in retrospect the three major classes of currently prescribed psychiatric drugs would likely never have been discovered using current drug discovery strategies, why should we believe that such strategies are likely to bear fruit now or in the future?…
There are likely additional potentially productive ways to get psychiatric drug research and development back on track but a few things are now clear: [1] what the field has been doing for the past 3 or 4 decades has failed to generate effective, mechanistically novel psychopharmaceuticals, [2] the pharmaceutical industry is now well aware of this fact and has therefore greatly reduced investing, and [3] there is no choice but to make changes in how we approach the study of disease mechanisms, drug discovery, and development in psychiatry. This will require major investments in neuroscience research, humility in the face of our ignorance, and a willingness to consider fundamental reconceptualizations of psychiatry itself. It will be a long, important, and exciting march.
All of these people [Insel, Hyman, Woodcock, Fibiger] and the collective APA hierarchy [APF Convenes Unique Pipeline Summit] seem to be desperately looking for a way to redirect our efforts at any cost to keep the dream alive, including reshaping psychiatry and psychiatric diagnosis [again!]. I find myself in a more pragmatic frame of mind as one might expect from my background. I think slim pickings are slim pickings. I doubt that there are magical drugs just around any corner waiting to be harvested by these new approaches. I now believe PHARMA gave it the old college try and "it is clear that a massive experiment has failed: despite decades of research and billions of dollars invested, not a single mechanistically novel drug has reached the psychiatric market in more than 30 years." They are the best financed act in town with a bevy of the best scientists available. They are surely the most motivated – finding silver bullets is their only reason for being. I’m sure that PHARMA would love to find better drugs than they’ve offered us recently. They’d much rather build their brand and fill their coffers from genuine breakthroughs than slithering around marketing the weak [and sometimes toxic] sisters they’ve sent our way [lying about their safety and efficacy]. But they can’t find those wonder drugs – and they could’ve bought a small country for what they spent on looking.
No one would have predicted this pathetic outcome after the human genome was sequenced 14 or so years ago.
I think the approval process is hopelessly outdated in the era of personalized medicine.
Take the cow behind the barn and shoot it. There’s no tweaking that is going to fix this mess.
Maybe it is weird to quote from my own blog but here goes:
While the notion that we would identify compounds – drugs – that could improve mood and thought might have seemed reasonable in 1970, there is so much to suggest this is not likely to be attainable. Complex behaviors do not seem to yield so easily to the drugs we prescribe.
Sandy,
Not weird – it’s a good thought. This idea of screening chemicals to see what they do seems more like something out of Tom Wolfe’s 1968 The Electric Koolade Acid Test than legitimate research into therapeutics…
Thanks. The sentence before suggested that this is a faulty paradigm.
Perhaps I missed something, but does the chart show aggregate R&D spend for drugs that made it to market plus the ones that failed?
How much of the spend was on researching novel agents vs copying competitors and competing in a saturated market?
I am curious about all drugs not just CNS agents, but there I agree with you about treating patients. It seems as if the industry became its own patient and humans got left somewhere behind.
Arby,
You’re confused because it’s confusing. I’m still working on that one.
http://www.accessdata.fda.gov/FDATrack/track?program=cder&id=CDER-RRDS-Number-of-NME-and-new-BLAs-submitted-and-approved
Dear Mickey and all,
With apologies for pointing out, once again, that there IS a well-established (since 1955) different “approach (to) the study of disease mechanisms, drug discovery, and development in (medicine).” I could point you to MANY early behavioral pharmacology papers (from the late 50’s onward) clearly and accurately predicting that the current state of affairs would arise from a simplistic, mechanistic, mentalistic approach to the effects of drugs on human behavior. You can learn about this well established DIFFERENT scientific approach best in this excellent book, now on Kindle:
“Introduction to Behavioral Pharmacology” – Edited by Alan Poling Ph.D., Thomas Byrne Ph.D. – There are hundreds, if not thousands, of substances that are used to modify behavior. While different classes of substances have known effects, one has only to see a group of people drinking to excess to recognize that not everyone responds in the same way to a given substance. Why do substances have the behavioral effects they do, and why do individuals vary in their responses to them? “Introduction to Behavioral Pharmacology” provides a conceptual framework for answering such questions. includes a short overview of behavioral analysis and general pharmacology, followed by detailed discussion of assessment of drug effects, the stimulus properties of drugs, drug abuse, and more.
It includes the following chapters:
Thomas Byrne and Alan Poling on Principles of Behavior Analysis
Alan Poling and Thomas Byrne on Principles of Pharmacology
Lisa Baker, Thomas Morgan, and Alan Poling on Neuropharmacology
Alan Poling and Thomas Byrne on Assessing Drug Effects in Non-Humans
Susan Snycerski, Sean Laraway, and Alan Poling on Basic Research with Humans
Alan Poling, Thomas Byrne, and Thomas Morgan on the Stimulus Properties of Drugs
Alan Poling on the Variables that Influence Drug Action
Scott H. Kollins, Kristal Ehrhardt, and Alan Poling on Clinical Drug Assessment
Sean Laraway, Susan Snycerski, Thomas Byrne, and Alan Poling on Drug Abuse
“This is a superb text which goes into great detail of explaining a multitude of effects drugs have on nonhuman and human systems. A must for the field of behavioral pharmacology, and I believe to be a good reference text for pharmacology and medicine as well. Gives some great insight into behavior analysis, operant condition, and respondent conditioning, and brings you up to speed before going into the behavioral aspects of drugs.
It speaks to many levels, from the novice undergraduate, to the graduate student and beyond, and is supplemented with charts and data from his lab experiments. There’s also some discussion of behavioral neuroscience as well, which can be helpful in describing how the drugs affect the Central Nervous System.”
I think I should take issue here with Sandra Steingard’s pessimism. We already did demonstrate that some drugs can improve mood and thought. Remember lithium? The issue now is are we going at drug discovery in a sensible way? Complexity is not a reason to declare the project quixotic.
Much of the fall-off in yield displayed so well by Dr. Mickey results from a series of perverse shifts of paradigm. One of these was the new conceit that science could be managed and that it was, moreover, too important to be left to the boffin scientists. So the center of gravity in drug development shifted away from academic centers to corporations. Once that happened then short sighted short term objectives elbowed out the commitment to basic science. The second perversion was the new conceit that top-down science would trump bottom-up science. One result of these shifts was the emergence of drug candidate screening programs, driven more by blind faith than by solid results.
A third perversion was the herd-like embrace of unacceptable animal models of psychiatric disorders. I have a favorite aphorism: the model is not the disease. In the case of depression, there are reasonable animal models that possess some verisimilitude to the clinical disorder, with face validity and construct validity. Problem is, these are not the models adopted by corporations in their very expensive drug screening programs. Following the business model, corporate drug screening programs focus on quick and dirty, utterly empirical animal models that lack all validity except for spotting me-too agents and then only with acute rather than chronic exposure.
Then of course in the case of depression there is the train wreck of DSM-III through DSM-5. The construction of Major Depressive Disorder, along with the rise of contract clinical trials, guaranteed that we probably wouldn’t recognize a genuine new antidepressant drug even if we had it in clinical trials. Little wonder that the yield has evaporated.
Interesting, Rob. In my experience, at least, I’m no longer having the experience of a psychiatrist looking at me like I just landed when I report an effect that is not on the insert. Progress.
Along the lines of different drugs having different effects on different people, is drugs having different effects on the same person when taken in combination. The changes can be profound, and I think this should be studied.
Joanna Moncrieff sums it up http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3230235/
“Drugs for psychiatric problems are prescribed on the assumption that they mostly act against neurochemical substrates of disorders or symptoms. In this article we question that assumption, proposing that drugs’ action be viewed rather as producing altered, drug induced states, a view we have called the drug centred model of action…..”
Some people experience these altered states as beneficial and some don’t. So much for efficacy.
I don’t recommend saluting anything Joanna Moncrieff runs up the flagpole. She is manifestly confused about the distinction between symptoms and disorders, so much so that her Exhibit A is the action of alcohol on symptoms of social phobia. To critique her tendentious misstatements thoroughly would take forever. Forget it.
I find her conceptualization of drugs as being symptom rather than disease specific extremely useful.
What exactly is a “symptom”? Basic understanding of the effects of drugs on behavior, including the critical influence of the context including the history of the species and of the individual, including genetic, environmental, behavioral, is critical. “Why do substances have the behavioral effects they do, and why do individuals vary in their responses to them?”
IMHO it really is an obligation of any prescribing psychiatrist to understand this. “Introduction to behavioral pharmacology” is likely to be VERY eye opening for anyone who has not encountered this detailed, rigorous scientific perspective and decades of careful experimental work.
The lie is the truth, I see it every damn day I have been working the past 10 years. Patients do not want to work at real, honest change; providers don’t want to work at getting to the true dysfunction; and administrators want a healthy bottom line to stay in power.
Again, pharma is not the primary enemy today, they have spawned a greater and more prevalent foe: fairly much everyone in the mental health system. Pharma just sits back and enjoys the chaos. The money made by psychotropics now fuels the next conquests as noted earlier: Geriatrics, oncology, and Hep C!
Sorry, I see lots of wasted energy at this site of late. I’m sure the same can be said of my blog as well, but, I want the head of the beast, and that is the APA, corrupt academia, and politicians who reinforce the criminality that pervades our society. The last that through Obamacare will complete the decimation of effective mental health care.
Hey, don’t believe me, keep railing about Paxil and Seroquel. Hmm, aren’t they generic for some time now…
Rob Purssey-
Thanks for the reference but it does seem that this approach is a more drug centered than disease centered way of thinking about psychoactive substances and that is the Moncrieff’s argument. In retrospect, I misrepresented her above by emphasizing symptoms.
“While the notion that we would identify compounds – drugs – that could improve mood and thought might have seemed reasonable in 1970, there is so much to suggest this is not likely to be attainable. Complex behaviors do not seem to yield so easily to the drugs we prescribe.”
Well it was not that difficult to observe people in 1970 using recreational drugs like cocaine or LSD that changed mood and thought, so it really didn’t seem like too much of an intuitive leap to think that if you could make a safer version of such without the side effects and addiction that seemed like a worthwhile goal.
The post makes it sound like antidepressants don’t work at all, which is hardly true.
I’m kind of in the Dr. Hassman camp. I’ve always though the bigger problem was KOL/ academia inertia than pharma. As we have discussed, I think much of modern research methodology is poor, and if secular saints were running these studies using DSM5, you would still produce junk for many of the reasons we talked about. I think back to those older TCA/MAOI studies and the striking difference between the efficacy vs placebo response rates. Any study that shows 50% placebo response in a study only proves that the academic needs to go back to school. Lesson one is Feynmann’s 1974 speech at Cal about sandy mice cages.
Sandra Steinberg did not misrepresent Joanna Moncrieff at all. For Moncrieff, “(her) drug-centred model suggests that instead of relieving a hypothetical biochemical abnormality, drugs themselves cause abnormal states, which may coincidentally relieve psychiatric symptoms.” If readers wish to immerse themselves in Moncrieff’s private world of selective reporting, misinformation, misconception, special pleading, and tendentious bias then here is a good summary.
The only sober guy at a fraternity party takes on all the KOLCHO happy talk at the Psychiatric Times:
http://www.psychiatrictimes.com/blogs/most-exciting-time-history-psychiatry
See comments….
You know what got me grief in residency? When people pointed out the placebo effect was 30-40% and the efficacy of the standards at the time, (the TCAs and Prozac getting settled as the first SSRI) was at best 70%, my reply was “so antidepressants only work 30-40% of the time, that must mean something else is needed to have a greater impact”. Wow, the hostility and looks of incredulousness were pervasive.
And now here we are 20+ years later and I feel a bit vindicated. Yep, the antidepressants only work about 40% of the time, and the lack of pushing for therapy and personal growth/change in patients by providers shows this pathetic push for more med trials and this disgusting polypharmacy now making antipsychotics drugs of primary use to be the ruin of mental health care. And the silence by credible providers who care is deafening!
So, yeah, my earlier comment here is the primary problem: why are we just dismissing or rationalizing, or just plain ignoring the logarithmic growth of therapists pushing patients to be on meds?
Look, I can see if my earlier comment was a bit rude to Dr Nardo, but, I don’t get the point of this blog by a psychiatrist who has witnessed the degradation of the field that has traveled far past the transgressions by Big Pharma alone. His voice should be focused on the abandonment by professionals beyond just psychiatrists. And, maybe he won’t embrace my focus on the role of antisocial cretins and sociopathy in various facets that just bash psychiatry into further submission, but, it is out there folks.
This election Tuesday will impact on health care for the next 4 years at least, don’t believe me today, but wait until Obamacare goes unchallenged if the Democrats keep a sizeable voice in federal politics into the 2016 election for the next ruler of America. And, no swipe at Dr O’Brien, but we will see the return of TCAs and MAOIs as primary drugs of use, because they not only are the cheapest, but the insidious agenda to create havoc on mental health patients is a goal by politicians and administrators. The disdain for mental health is pervasive among the elite in this country, who profoundly are the ones we should be enforcing be in care! But, what can ya do with pathologically impaired narcissists and antisocials at the end of the day!?
Oh, and neither a Democrat or Republican will change things for the better in 2016, note that as well. Remember one thing about genuine human nature, people who are best to lead don’t instinctively want to, but have to. Because healthy and responsible people realize leading has risks, and want to be cautious and respectful that directing the public is not an easy task.
You think Obama and his ilk could say that above, much less even think it?
Just watch the way he walks up and down stairs, what a non verbal cue!
I think rationing and medical legal pressures will force psychiatrists (correction: GPs or NPs who consult with a psychiatrist–and eventually a software program– through Collabo-care) into using off patent SSRIs, since TCAs and MAOIs are really no cheaper. Plus many pharmacies don’t even carry MAOIs in stock and freak out when the see a script for an MAOI. Prozac is 9 bucks for a 3 month supply at WalMart.
GPs and NPs will never use MAOIs. Even most psychiatrists are afraid of them. TCAs will continue to be used off label for pain and sleep issues.
Forget the grid. You have to go off it to get away from the middlemen and the paperwork and constant ethical challenges.
Actually your above comment is true, but, it will still come down to what is cheap, easy, and convenient, oh, and popular too. Hence how health care becomes what politics is inherently about. Yeah, using TCAs and MAOIs require thought and attention, and let’s face it, too many of our “colleagues” do not want to expend that effort!
Thanks for the clarification.
Joel H
Hmm, about that Obamacare concern:
http://www.nationalreview.com/article/391532/health-care-hell-kevin-d-williamson
My best highlight to share with you all from the link?:
“Nearly 60 percent of doctors said they expected the ACA to have an unfavorable or very unfavorable impact on their practices. Expect those additional costs to be passed on to consumers in the form of higher prices or diminished quality of care.”
The non providers who read and comment here, you can read the link and take away that doctors are just being jerks in only worrying about money, but, I just want to ask each and every one of you out there, how many of you have taken a vow of poverty and do your job willingly and eagerly accepting being underpaid and micromanaged in your job responsibilities?
That is what Medicare and Medical Assistance do to us physicians, and all you patients know about that is prescription authorizations. Which is falsely portrayed as our fault, as how many of you clinicians out there have been told by the patient or pharmacist, “you wrote for the wrong drug”.
The motto of Obamacare is simply that of politicians, “what is popular, easy, and convenient, oh and cheap too”.
Which is how your politicians frame you as constituents, cheap and easy especially!!!
If interested, read the post at my blog today about what the election will deteriorate to with the ads and rhetoric this weekend, I think the links in the post alone will be thrilling and stimulating to peruse!!!
You might need a benzo after trying to digest those articles!!!
Dr. Hassman, I agree that being micromanaged as a physician by insurance companies must stink to high heaven. I can’t imagine being in that position after I dealt with mine on an authorization issue.
Regarding physicians having to take a vow of poverty, for me the issue is not so clear cut. I could see how the ACA could affect physicians like primary care docs. But as far as it making sleep docs poor, well if they have to operate 4 centers vs. their current 6, sorry, I don’t have as much sympathy, particularly when so many of them aren’t very helpful in helping patients resolve pap therapy problems.
And you and I have discussed this issue before but it bears repeating. The ACA is definitely not perfect by a long shot. But without having insurance, I would be royally screwed big time since medicare eligibility is a few years away.
I look forward to reading in future times WHEN those who support Obamacare have their personal moment of being on the wrong end of a mandate.
Mandates are almost NEVER about doing what is right and responsible, just solely what is easy, convenient, and, controlling.
So, yes, I recognize and respect being without insurance sucks, but, people have the right to chose, even if a choice is reckless and irresponsible, but, you listen to the leadershi* of Democraps and Repugnocants, they are not interested in the welfare of the public. It is only about a win for the party, not the public.
Just remember what George Carlin said, “if you vote for seone who is selfish and incompetent, who then screws things up, you have no right to complain.”
I add this: if you vote to keep such people in place to overtly continue such bad rule, well, people like me are on to you, and this partisan agenda to corrupt and self serve is living on borrowed time.
There is a better way to access and provide care, politicians only belong in the system to make sure accountability and consequences for poor choice and agenda by providers is in place.
Fair and unbiased readers, pay attention to those who advocate for agendas that favor the few and dismiss the many. And that goes for providers and patients equally.
Nice addendum to the above comment to AA re Obamacare, from this link:
http://www.foxnews.com/opinion/2014/11/01/real-reason-hillary-clinton-keeps-changing-her-economic-message/?intcmp=ob_homepage_opinion&intcmp=obnetwork
the comment: “For example, ObamaCare is a gusher when it comes to hosing down businesses and entrepreneurs with job-killing costs and regulations. The non-partisan Congressional Budget Office has estimated (its estimates keep varying) that because of ObamaCare, “Virtually as many Americans will lack health coverage in 10 years as before the law was passed—but 2 million fewer will be working than if the law hadn’t passed.”
Wow, now there is a real good legislative agenda with this law! So, hope you keep that wonderful insurance you have today, thanks to Obamacare.
But, what if you are unemployed because of it? See the negatives a bit more, AA? What’s next, Obama is going to mandate employment?!
One of the most infuriating things about psychiatrists and psychologists as a group as that they endorsed ACA and universal care while the majority will not accept insurance through ACA (or any insurance for that matter). This is intellectually and ethically indefensible no matter how you feel about the subject in general. It’s like limousine liberals who wouldn’t dare send their kids to public school. It’s time for some of these hypocrites to preach what they practice.
I understand that people with disagree with me as the country is split on the issue, and I saw the flaws with ACA from the beginning. But at least I have respect for psychiatrists who supported it and follow it up by seeing patients covered by it. That group is very small.
Kind of the same reason that as a climate change skeptic, I can respect Ed Begley who rides the bus and mock Leo DiCaprio and Al Gore whose lifestyles are one massive carbon footprint.