by Relman AS.New England Journal of Medicine. 1980 303[17]:963-70.
The most important health-care development of the day is the recent, relatively unheralded rise of a huge new industry that supplies health-care services for profit. Proprietary hospitals and nursing homes, diagnostic laboratories, home-care and emergency-room services, hemodialysis, and a wide variety of other services produced a gross income to this industry last year of about $35 billion to +40 billion. This new "medical-industrial complex" may be more efficient than its nonprofit competition, but it creates the problems of overuse and fragmentation of services, overemphasis on technology, and "cream-skimming," and it may also exercise undue influence on national health policy. In this medical market, physicians must act as discerning purchasing agents for their patients and therefore should have no conflicting financial interests. Closer attention from the public and the profession, and careful study, are necessary to ensure that the "medical-industrial complex" puts the interest of the public before those of its stockholders.


Pharmalot: WSJby Ed SilvermanDec 4, 2014Walk into any physician’s office and promotional messages about medicines can be seen no matter where you look – brochures are typically displayed on a counter and advertorial messages are often playing on a flat-screen TV mounted on a wall. This type of patient outreach, which is called point-of-care marketing, is hardly new, but what is different is that the pharmaceutical industry and other companies selling health products are relying on this form of promotion more than ever before, according to a new study.
Since 2010, the amount of money spent on POC marketing in physician offices, hospitals and pharmacies grew 10% annually, reaching $400 million this year. Nearly 90% of that spending was done by drug makers, says Hensley Evans of ZS Associates, a consulting firm that conducted the study. Moreover, spending on POC is expected to exceed $500 million within the next two to four years. “This is clearly growing in importance,” says Evans, adding that POC communications are second only to television advertising in terms of reaching consumers.
Of course, patients waiting to see a doctor are the classic captive audience. ZS points to another study that found 89% percent of patients say they watch television in a waiting room, and 76% of patients recalled information they read or heard in a waiting room. Moreover, ZS notes that patients can wait 20 to 40 minutes to see a physician, and wait times are expected to rise over the next decade as the number of visits to primary care doctors reaches 565 million in 2025, up from 462 million in 2008. ZS also cites data indicating 65% of patients find POC materials credible because there is an implied endorsement from the doctor. This is a subtle but important distinction from DTC advertising on television, if only because the consumer receives the message at home or in some other surrounding.
Meanwhile, the growth in direct-to-consumer advertising for prescription drugs rose 1.3% on a compounded annual basis. As a result, ZS calculates that POC spending will have accounted for 10% of all DTC spending this year, up from slightly less than 7% in 2010. The shift reflects a few developments. For one, drug makers are increasingly trying to remind patients to take their medicine, since adherence boosts revenue. And ZS notes that a logical forum for delivering that message is in a location where diagnosis and treatment are discussed.
At the same time, drug makers are selling fewer blockbusters to the widest possible patient population and, instead, are increasingly marketing therapies targeted at specific patient groups. This shift calls for more customized marketing than what television commercials may allow, according to ZS. The marketing is apparently having the desired effect. ZS cites data indicating that 84% of patients who visited waiting rooms and were exposed to POC communications report that the messages made them interested in the product.
Nonetheless, Evans does not believe that POC marketing will overtake or supplant other forms of marketing. Rather, she believes that drug makers are simply increasing their POC spending in response to changing business models. “But we are seeing more consumers become more engaged,” says Evans. “They can have a more educated conversion with physicians and not just about a promoted brand [product], but also about broader information for treating a condition.”
If this sounds familiar it is because this is the same explanation that the pharmaceutical industry has used to explain why DTC advertising is beneficial. Some doctors, however, complained that patients were not given complete information or were unnecessarily prompted to ask for certain medicines. Now, though, the marketing is increasingly shifting to the physician office. In effect, the physician has become more of a marketing partner with the pharmaceutical industry.
In 1980, Dr. Relman saw what had already happened in the years after President Nixon opened Pandora’s Box in 1973 [see «parity?»…] with the Health Maintenance Organization Act, "which encouraged rapid growth of Health Maintenance Organizations [HMOs], the first form of managed care." While it may seem far-fetched to propose that things could change in so a short period, that’s certainly how it felt. 1980 was actually probably too late. Dr. Relman was the long-time editor of the New England Journal of Medicine [see Dr. Arnold Relman, 91, Journal Editor and Health System Critic, Dies] who continued the themes in this piece throughout the remainder of his career. I’m not aware of his mentioning psychiatry, but his wife, Marcia Angell, who later also became an editor of the NEJM herself, made up for that in her widely read review of the books of Irving Kirsch [The Emperor’s New Drugs: Exploding the Antidepressant Myth], Robert Whitaker [Anatomy of an Epidemic], and Danny Carlat [Unhinged: The Trouble with Psychiatry] [see in the name of ethics… and no leg to stand on…].
 It’s such an old story – Pandora’s Box. She was given a box [actually, a jar] as a wedding present with the injunction to never open it. Pandora’s curiosity won out but in opening the box, she unwittingly unleashed all the evils stored inside to spread throughout the world. So the lesson of the story is that some things, once released, can be neither contained nor put back in the box.
It’s such an old story – Pandora’s Box. She was given a box [actually, a jar] as a wedding present with the injunction to never open it. Pandora’s curiosity won out but in opening the box, she unwittingly unleashed all the evils stored inside to spread throughout the world. So the lesson of the story is that some things, once released, can be neither contained nor put back in the box.
While I would and did argue with the changes Drs. Sabshin and Spitzer brought to psychiatry with the DSM-III, that’s not my point this time. American psychiatry did everything possible to get with the Managed Care program including producing a code book that made things easy for them, gravitating to short sessions primarily focused on symptomatic drug treatments, abandoning traditional in depth evaluations, being empaneled in plans for the insured outpatients, abandoning hospital treatment for the severely disturbed, etc. In addition, Academic psychiatrists "signed on" as authors to papers written by medical writers that exaggerated drug efficacy and minimized adverse events. Many became traveling speakers for the pharmaceutical companies. But it all came for naught. Worse than that, it lead to the routine use of medications for almost anyone who showed up. And now the whole specialty is being appropriately discredited for these practices. Simply put, various industries increasingly controlled the psychiatry from 1980 forward. But psychiatry is just a loud and now very public example of a general trend felt throughout medicine – the one Dr. Relman warned us about in 1980.
In 2012, asked how his prediction had turned out, Dr. Relman said medical profiteering had become even worse than he could have imagined. His prescription was a single taxpayer-supported insurance system, like Medicare, to replace hundreds of private, high-overhead insurance companies, which he called “parasites.” To control costs, he advocated that doctors be paid a salary rather than a fee for each service performed.
Dr. Relman recognized that his recommendations for repairing the health care system might be politically impossible, but he insisted that it was imperative to keep trying. Though he said he was glad that the signed by President Obama in 2010 enabled more people to get insurance, he saw the legislation as a partial reform at best. The health care system, he said, was in need of a more aggressive solution to fundamental problems, which he had discussed, somewhat philosophically, in an interview with Technology Review in 1989.
“Many people think that doctors make their recommendations from a basis of scientific certainty, that the facts are very clear and there’s only one way to diagnose or treat an illness,” he told the review. “In reality, that’s not always the case. Many things are a matter of conjecture, tradition, convenience, habit. In this gray area, where the facts are not clear and one has to make certain assumptions, it is unfortunately very easy to do things primarily because they are economically attractive.”

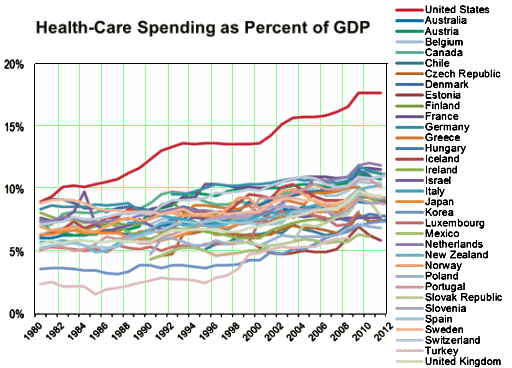
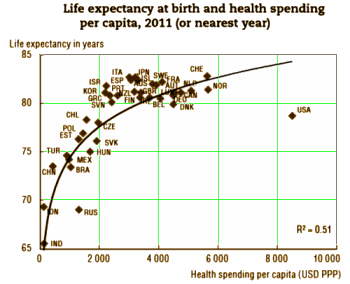
Amen… here is my 2 cents worth, from the time of President Obama’s inauguration.
Hope.I remember her well, present when Obama was awarded a premature Nobel Peace Prize. coming close to suffocation in Cassandra’s box when wars and shameful human rights abuses followed the US president’s highly praised and highly abstract talk on “just war”. Hope is visibly present again this week, with Malala and Kailash in town, meeting the prime minister and the minister of foreign affairs just now. The population is more firmly social democratic than the present conservative minority government, and the city of Oslo is not as besieged by security forces as when the Obamas were here. When dr Relman and his wife, whom he sweetly called “angel” were in town a couple of years ago, for a panel discussion on health policies, Hope was there, as she is in today’s commendable articles on this site, by doctors Nardo, Carroll and the comment on Health Care Renewal from January 2009 by one of my favorite commenters, Steve Lucas. Thank you all!
Robert Whitaker encourages Hope too. His recent open talk at the UiO was on the critical question How do we know what we know? History, science and the long-term effects of psychiatric medications. That story can be told as progressive Progress, more and more safe and effective drugs. In my experience, this is the deceit which the institution of psychiatry and most practicioners I know of hide behind. The truth is another, far darker story, sharply rising numbers of disabled and early death parallell to the rise of DSM diagnostics, KOLs-led overdiagnosis, overprescription and so on. Whitaker told of a tense meeting with APA members who objected to the version he presented. “We knew that years ago.” Whitaker’s answer: “Yes, but you never told your patients and the public.”
I know I’ve been deceived, but I’ll do my best to keep up with Hope. The institution of psychiatry has undermined its credibility. We barbarians are at its gate – accompanied by Hope!!
Then we have this situation where an administrator drove a new doctor out of a practice:
http://www.kevinmd.com/blog/2014/11/joining-medical-practice-importance-autonomy.html
And this doctor who is afraid to practice:
http://www.kevinmd.com/blog/2014/12/residency-im-scared-practice-outpatient-medicine.html
And how far will an office go to collect $25.00
http://healthbusinessblog.com/2014/12/02/an-expensive-25/
The system we have today in medicine is so geared to supplying a commodity that all semblance of personal service has been lost. We are but widgets in the machine.
Steve Lucas
Dr. Relman was the intellectual and life partner of Dr. Marcia Angell, author of two 2011 articles in the NY Review of Books that caused a great stir and some condemnation from organized psychiatry:
http://www.nybooks.com/articles/archives/2011/jun/23/epidemic-mental-illness-why/
http://www.nybooks.com/articles/archives/2011/jul/14/illusions-of-psychiatry/
Among criticisms of Dr. Angell: Because she is not a psychiatrist, she could not possibly understand the science (or lack of it) of the discipline.
Wow Mickey, you’ve done it again. This is one of your more excellent rants. I’m once again grateful for your choice of what to do in your so-called “retirement.”
Right now iit looks like Drupal is the top blogging platform out
there right now. (from what I’ve read) Is that what you are using oon your blog?