I’m obviously not writing about this because I’m conflicted about the Black Box Warning. I’ve seen enough adolescent patients with the Akathisia syndrome from SSRIs to know it’s a real thing. And I know of completed suicides that I am convinced were SSRI induced. In addition, I am underwhelmed with the claimed efficacy of SSRIs in adolescents in Clinical Trials [I think I’ve read them all in the course of researching for this blog]. I would and have prescribed SSRIs to adolescents in situations where both the teen and some responsible adult will listen to the warnings and agree to being closely observed. The few cases where I’ve done that have been with habitual compulsive behaviors [bulemia, cutting, etc] with success. So I am perfectly fine about the Black Box Warning staying exactly like it is. Good job FDA…
I am writing about this once again because of the confusion of tongues that swirls around this issue. The one solid fact that emerged from the population studies is that the prescription rate of antidepressants either leveled out or fell [instead of continuing to increase] in response to the Warning. In Lu et al, this was true for adolescents, young adults, and older adults – even though that initial warning only pertained to the adolescents.
In the two articles in PSYCHIATRICNEWS [boxes black are back I…], Dr. Darrel Regier proposed that the reason for the fall-off in prescribing had to do with the widespread press coverage of the warning, scaring away doctors and patients alike [particularly primary care doctors who were prescribing the majority of antidepressants]. Regier proposed that the primary care doctors couldn’t follow the patients as closely as recommended, and were afraid of getting sued. He went further, saying that the drop in prescribing was not matched by referral for some other treatment modality [eg CBT], presuming that meant that depressed kids just weren’t being treated – a point echoed by Dr. Michael Thase in the article. Child Psychiatrist Dr. David Fassler [former APA Board member] felt that the press coverage implied that the antidepressants increased the suicide rate, something unintended by the FDA – a point backed up by Dr. Thomas Laughren, team leader of the Psychiatric Drug Group within the FDA during the 2004 FDA hearings.
All of this speculation about the psychology of the primary care physicians strikes me as hyperbole. If I were to wax eloquent about Drs. Regier’s and Fassler’s own inner workings, I expect they would break out singing some evidence-based medicine anthem in three part harmony [and accuse me of being a loose cannon]. And they sure don’t paint a very flattering portrait of primary care doctors – fear of lawsuits, basing clinical decisions on newspaper reports, turning away depressed adolescents "untreated." And further, they’re assuming that the abrupt halt to the escalating antidepressant prescription rate was a bad thing, rather than something perfectly reasonable – slowing down an avalanche.
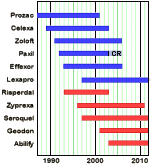 The time leading up to the 2004 Black Box Warning was the heyday of psychopharmacology when drugs continued to flow from the mythical PHARMA pipeline. Direct-to-Consumer ads for antidepressants blanketed the media. Drug reps detailing psychoactive drugs and KOLs speaker’s bureaus were focusing on primary care physicians, specifically because of the much broader market than that reached by psychiatrists. Rather than see the de-escalation of antidepressant prescriptions as ignoring depressed teens, it seems much more plausible to suppose that the Black Box Warning appropriately neutralized the hype that had bombarded the general practitioners in those days – leading to more rational prescribing.
The time leading up to the 2004 Black Box Warning was the heyday of psychopharmacology when drugs continued to flow from the mythical PHARMA pipeline. Direct-to-Consumer ads for antidepressants blanketed the media. Drug reps detailing psychoactive drugs and KOLs speaker’s bureaus were focusing on primary care physicians, specifically because of the much broader market than that reached by psychiatrists. Rather than see the de-escalation of antidepressant prescriptions as ignoring depressed teens, it seems much more plausible to suppose that the Black Box Warning appropriately neutralized the hype that had bombarded the general practitioners in those days – leading to more rational prescribing.
And so to the confusion of tongues…
-
The arguments in the two articles are not primarily against the content of the Black Box Warning – the reported signal for suicidal thoughts or behavior in RCTs of adolescents treated with SSRIs or the case reports of suicides presented to the FDA Hearing. These arguments are focused on the decrease in prescription of SSRIs that followed actually adding the Black Box Warning – a reproducible finding in multiple studies – and suggest that the quantity and quality of the media reporting at the time inappropriately scared clinicians and patients alike; leading to a fall in prescription rates; meaning that many depressed adolescents were being deprived of necessary treatment or were not even being brought for treatment; meaning that they were therefore vulnerable to depressive suicide.
-
The Randomized Clinical Trials of these drugs in adolescents have been the subject of intense scrutiny and many meta-analyses of both efficacy and adverse effects, specifically suicidality. Most of them have been reviewed in this blog along the way. The RCTs are industry funded, conducted by Clinical Research Organizations, and several are clearly ghost-written by agents working for the industry sponsor. A 2012 extensive Cochrane Collaboration Systematic Review concluded:by Hetrick SE, McKenzie JE, Cox GR, Simmons MB, and Merry SNCochrane Database of Systematic Reviews. 2012 Issue 11. Art. No.: CD004851.
The Abstract[abstracted]
BACKGROUND: Depressive disorders are common in young people and are associated with significant negative impacts. Newer generation antidepressants, particularly selective serotonin reuptake inhibitors (SSRIs), are often used, however evidence of their effectiveness in children and adolescents is not clear. Furthermore, there have been warnings against their use in this population due to concerns about increased risk of suicidal ideation and behaviour.OBJECTIVES: To determine the efficacy and adverse outcomes, including definitive suicidal behaviour and suicidal ideation, of newer generation antidepressants compared with placebo in the treatment of depressive disorders in children and adolescents.SEARCH METHODS:…SELECTION CRITERIA:…DATA COLLECTION AND ANALYSIS:…MAIN RESULTS: Nineteen trials of a range of newer antidepressants compared with placebo, containing 3335 participants, were included. The trials excluded young people at high risk of suicide and many co-morbid conditions and the participants are likely to be less unwell than those seen in clinical practice. We judged none of these trials to be at low risk of bias, with limited information about many aspects of risk of bias, high drop out rates and issues regarding measurement instruments and the clinical usefulness of outcomes, which were often variously defined across trials. Overall, there was evidence that those treated with an antidepressant had lower depression severity scores and higher rates of response/remission than those on placebo. However, the size of these effects was small with a reduction in depression symptoms of 3.51 on a scale from 17 to 113 (14 trials; N = 2490; MD -3.51; 95% confidence interval (CI) -4.55 to -2.47). Remission rates increased from 380 per 1000 to 448 per 1000 for those treated with an antidepressant. There was evidence of an increased risk (58%) of suicide-related outcome for those on antidepressants compared with a placebo (17 trials; N = 3229; RR 1.58; 95% CI 1.02 to 2.45). This equates to an increased risk in a group with a median baseline risk from 25 in 1000 to 40 in 1000. Where rates of adverse events were reported, this was higher for those prescribed an antidepressant. There was no evidence that the magnitude of intervention effects (compared with placebo) were modified by individual drug class.AUTHORS’ CONCLUSIONS: Caution is required in interpreting the results given the methodological limitations of the included trials in terms of internal and external validity. Further, the size and clinical meaningfulness of statistically significant results are uncertain. However, given the risks of untreated depression in terms of completed suicide and impacts on functioning, if a decision to use medication is agreed, then fluoxetine might be the medication of first choice given guideline recommendations. Clinicians need to keep in mind that there is evidence of an increased risk of suicide-related outcomes in those treated with antidepressant medications.from the Review:
A U T H O R S ’ C O N C L U S I O N SImplications for practiceThe evidence for the effectiveness of newer generation antidepressants compared with placebo in the treatment of depressive disorder in children and adolescents is not compelling; the overall effects of antidepressants compared with placebo were not modified by drug. The methodological shortcomings of the trials make it difficult to interpret outcome data on the efficacy of newer generation antidepressant medications. This is a particularly unsatisfactory since large numbers of children and adolescents have participated in trials, and we are still unable to answer the important clinical question of whether antidepressant medications are effective in treating depressive disorders. The search for treatments that reliably lead to good clinical outcomes must continue. Even when there is evidence that newer generation antidepressants reduce depression symptom severity, it is unclear whether the difference in effect between antidepressants and placebo reflects a difference that is of clinical importance to patients…I would say this review is, if anything, too forgiving…
My borrowed title [the confusion of tongues] refers to two communications [1. and 2.] that pass on the street as strangers with neither mutual recognition nor resolution. The scenario in 1. describes a vital treatment which, if missed, may have dire consequences. Whereas, the evidence in 2. suggests that the same treatment for the same problem is borderline effective, if at all, and, if used, may have the same dire consequences. The Black Box Warning being challenged is backed by independent meta-analyses and numerous case reports. The opposition to the Black Box Warning proposes that the physicians and patients who responded to it by failing to continue an escalating usage pattern were swayed by the initial media response and are neglecting real medical and psychiatric needs out of fear, yet no credible evidence has been mustered to support that hypothesis after a decade of persistent trying. The argument [1.] still rests on unsubstantiated speculations about the motivations of a large, heterogeneous group of physicians and guesses about the original intentions of the FDA, rather than scientific evidence. And the burden of both commercial and ideological bias is clearly carried by those opposing the Black Box Warning.
I like your example.
A poor follow on is that in any population we will see certain people exhibit certain problems, heart, cancer, weight, and mental health issues. This becomes our potential market size.
A good product will reach a certain market penetration without marketing as those involved become aware of it. Sales then take over, commercial interest, to push for more market penetration, or in the case of pharma, expanding the market beyond those originally determine to need the product.
Today we see pharma trying to set protocols for the treatment of various illnesses with the now added concept that if you have this, you have that. This allows for a multiplier effect as patients become more and more medicated. A very old sales concept is it is easier to sell an existing customer than create a new one, so we have people taking multiple meds often for the same condition.
I am troubled by the reliance on hard numbers, as I do not feel this takes into account the number of people who have, and are leading disrupted lives, due to their medication. This concept for me moves across all of medicine as pushing BP to very low levels may produce dizziness and a possible fall while trying to stand. Low LDL may aggravate dementia as this slow starving of the brain leads to additional problems.
SSRI’s have the additional problem of possibly producing side effects in very short periods of time taking all of those involved by surprise. A Black Box warning is a caution, one that should be taken seriously.
Steve Lucas
As you say, Mickey, doctors treat individuals, and that’s what matters, especially where drug reactions are concerned. I really do wish that persons had to undergo a thorough physical and counseling before seeing a psychiatrist about “depression”, save those time that they really should be hospitalized and carefully monitored.
A hopeless life can drive people to suicide and teens tend to be impulsive. They are struggling to form an identity and find their place in a world in which they have little experience. Many, if not most, have thoughts about death as part of a natural progression in laying claim to their own lives. Most are surrounded by their fellow teenagers all day and are sorely lacking in sufficient guidance from adults with more nuanced perspectives on life. Some are living in squalid and/or abusive/neglectful situations and are lost and feel helpless.
I’m thinking that there’s a strong relationship between suicidal ideation and feelings of helplessness. And, of course, there are any number of other reasons for a person to feel or be suicidal. I wonder about the reliability of checklists to determine suicide risk in anyone. Is there a separate checklist for teens?
It’s very hard, no doubt, to lose a patient to suicide. Vicarious trauma and feelings of guilt are understandable. Psychiatrists have a suicide rate four times higher than the general population. I suspect that because of these two conditions that suicide is a very painful and emotional issue for most people working in the mental health field and dealing with the suicidal and maybe suicidal, and let’s just err on the side of suicidal patients.
There will always be people who commit suicide regardless of measures to prevent it, and people who impulsively commit suicide without any seeming warning signs. It’s a tough issue— very tough— but knee jerk reactions to black box warnings are not helping.
Wiley,
“I’m thinking that there’s a strong relationship between suicidal ideation and feelings of helplessness”
One of the tragedies of the “new psychiatry” is that we seemed to have jetissoned our history. Freud had proposed that emotions are biological signals from the interior – as in anxiety as a signal of danger. In the 1950s, Edward Bibring proposed that depessive affect is a signal of “helplessness” as you propose. This is a very useful clinical construct that can often move things closer to the central problem by exploring “helpless about what?” it’s hard to “help” or “get help” without knowing the “what” – which is often outside awareness……
Steve,
“I am troubled by the reliance on hard numbers…”
Amen!
It may be useful also to include the feature of hopelessness in this discussion of suicide. It is not coterminous with helplessness and it also is a powerful driver of suicidality. Jerome Frank focused on helplessness in his famous treatise on demoralization – the syndrome of giving up coping efforts through the belief that nothing one does will make a difference. See here for a summary discussion. Hopelessness has a different slant on the dysphoria – it is the cognitive bias that nothing anybody else does will make a difference either. So we might say all hopeless patients are also demoralized but not all helpless patients are hopeless, and that the hopelessness is the proximate trigger for suicidality. After all, demoralized patients can be quite reactive in their mood and behavior to positive events or interventions that cut through their Gordian knot of helplessness.
Back to the matter of youth suicidality, by far the highest rates of completed suicide are seen in Native American/Alaskan youth, both males and females. See here. This profile underlines the salience of cultural and social/economic factors in the development of helplessness and hopelessness.
Yes, Dr. Carrol, and I would like to add that, especially in children and teens, that hopelessness may be, for all practical purposes, well informed. I think the saying that “suicide is a permanent solution to a temporary problem” discounts a lot of horrible realities that have no apparent solution and no apparent exit in time to prevent a downward spiral that a large percentage of people would have a very difficult time pulling themselves out of. I think the first three years of development has a profound effect on whether or not a person can find the strength and forbearance to rescue themselves; but then again, there are situations that make well-adjusted adults break, like the loss of a child.
Life is hard sometimes for most people, and hard most of the time for too many. Children and teens who need hope, may not need a diagnosis, so much as an adult who hears them and offers perspective and assistance. I think one of the problems with psychiatry is that it tries to deal with social problems as biological problems. Sure, a drug may very well help to pull a person out of an emotional storm physiologically; but it isn’t a solution to the problems that created the hopelessness, and helplessness. And maybe social problems should be screened for so that people suffering from lives that are hard to bear can be sent to someone who can help a person navigate the bullies in their lives and deprivations.
Yes. And it goes without saying that, especially in primary care settings, a good many patients given antidepressant drugs have a demoralization problem rather than a major depression problem. This applies to youth as well as adults. They can expect little drug-attributable benefit while being exposed to all the potential harms. There is no entry for demoralization in the Index of DSM-5. That said, the differential diagnosis is not always a slam dunk, especially with a brief contact, so many primary care physicians end up using antidepressant drugs pragmatically in the misguided belief that they may not do a whole lot of good but that they probably won’t do much harm. Most of the time that works out OK but there is an expectable base rate of very bad surprises. At least the black box warning serves to remove complacency here.
It sounds to me, Dr. Carrol like you and your colleagues aren’t representative of the treatment that poor people get, and that many, many psychiatrists are no more attentive towards their patients and prescribing habits than GPs. It’s just entirely too easy to be prescribed psychoactive drugs with little thought and next to no warnings— not even being asked if there is someone in your life who knows you very well who can look for odd changes in mood and mental states.
Also, antidepressants are being prescribed for pain and sleep disturbance to who knows what avail. I’m down to 65 mg from 150 mg of amitriptyline daily and the pain is dropping with the dosage. None of my neurologists even hinted at the fact that it doesn’t work on nerve pain for most people, much less that it can make the pain worse. So far, hormone replacements and Icy Hot have been wonders. I don’t even bother with ibuprofen now.
There is insufficient information and study on the effects and effectiveness of most of the psychoactive drugs, and I do believe that the pharmaceutical industry should be banned from testing their own drugs, and the random, double-blind study should be put in its place, which doesn’t appear to me to be “the gold standard.” We need more long-term observational studies and in-depth studies of drugs we’ve been using for the past twenty years— I am totally with Ben Goldacre on that score.
Oh, and the psychoactive drug that messed me up more than any other is baclofen. Anything that passes the blood-brain barrier needs to be taken seriously and accompanied by a lot of solid information.
Wylie, when you drop an attitude bomb like your last comment it derails the conversation… it doesn’t move the conversation forward. We have no idea what your basis is – except for attitude – for airily smearing whole classes of professionals.
“Attitude bomb?” I was flatly stating a fact.
A neighbor’s adolescent son is now in the hospital recovering from a suicide attempt via Wellbutrin overdose. Of course, Wellbutrin is not approved for pediatric use.
He experienced rhabdomylolysis, endangering his kidneys and liver, which while he’s in the pediatric ICU has kept additional drugs out of the picture.
His mom doesn’t think he was suicidal. She says he was out with his friends prior to the overdose.
He is about to be placed into 14 days of involuntary psychiatric commitment.
Was this a Wellbutrin-induced suicide attempt? Given the black-box warning, would anyone in the hospital even stop to think of this?
The best thing that can happen to him now is that the condition of his liver and kidneys might keep the hospital psychiatrists from flooding him with multiple drugs in large doses. Even so, I expect him to come out on an antidepressant, an antipsychotic, and a benzo.
In all of this, I am trying to figure out how this process might persuade a terrified adolescent that the world is not a threatening place. It sure isn’t convincing to me.
The domain of psychiatry hasn’t yet reached the stage of ethnic cleansing and genocide that we saw in Yugoslavia after Tito’s death, but it is well on the way.
And how dare the layperson state that individual psychiatrists have had anything to do with this.