An explanatory randomised controlled trial testing the effects of targeting worry in patients with persistent persecutory delusions: the Worry Intervention Trial [WIT].Editors: Freeman D, Dunn G, Startup H, and Kingdon DLancet. 2015 2[4]:305-313.NCBI Bookshelf: Queen’s Printer and Controller of HMSO 2015.
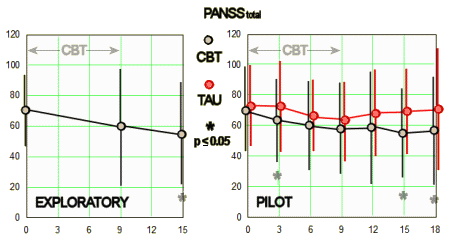
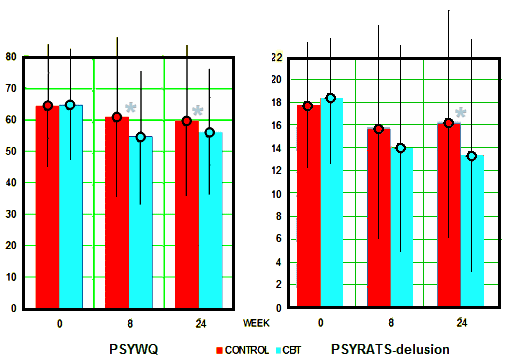
BACKGROUND: Persecutory delusions are a key experience in psychosis, at the severe end of a paranoia continuum in the population. Treatments require significant improvement. Our approach is to translate recent advances in understanding delusions into efficacious treatment. In our research we have found to be an important factor in the occurrence of persecutory delusions. Worry brings implausible ideas to mind, keeps them there and makes the experience distressing. Reducing worry should lead to reductions in persecutory delusions.OBJECTIVE: The objective was to test the clinical efficacy of a brief cognitive–behavioural intervention for worry for patients with persistent persecutory delusions and determine how the treatment might reduce delusions. Embedded within the trial were theoretical studies to improve the understanding of worry in psychosis…MAIN OUTCOME MEASURES: The main outcomes measures were of worry [Penn State Worry Questionnaire; PSWQ] and persecutory delusions [Psychotic Symptom Rating Scales; PSYRATS]. Secondary outcome measures were paranoia, overall psychiatric symptoms, psychological well-being, rumination and a patient-chosen outcome.RESULTS: In total, 95% of the patients provided primary outcome follow-up data. For the primary outcomes, in an intention-to-treat analysis, when compared with treatment as usual, the therapy led to highly significant reductions in both worry [PSWQ: 6.35, 95% confidence interval [CI] 3.30 to 9.40; p < 0.001] and the persecutory delusions [PSYRATS: 2.08, 95% CI 0.64 to 3.51; p = 0.005]. The intervention also led to significant improvements in all of the secondary outcomes. All gains were maintained. A planned mediation analysis indicated that change in worry explained 66% of the change in the delusions. We also found that patients without intervention report a passive relationship with worry, feeling unable to do anything about it; worry brings on depersonalisation experiences; and the patient group has very low levels of psychological well-being.CONCLUSIONS: This was the first large randomised controlled trial specifically focused on the treatment of persecutory delusions. Long-standing delusions were significantly reduced by a brief CBT intervention targeted at worry. The intervention also improved well-being and overall levels of psychiatric problems. An evaluation of the intervention in routine clinical setting is now indicated. We envisage developing the intervention booklets for online and app delivery so that the intervention, with health professional support, has the possibility for greater self-management.
Daniel Freeman and colleagues report the results from thei r trial that investigated the clinical effects of an intervention targeting worry in patients with non-affective psychosis. The authors accurately write in their Introduction that treatments for psychotic conditions, such as schizophrenia, need substantial improvement. The first-line treatment of schizophrenia—ie, antipsychotics—can suppress delusions and hallucinations, but patients still suffer from other symptoms such as negative symptoms, and often report adverse side-effects from the medication [eg, apathy, neurological side-effects, serious weight gain, and sexual dysfunction]. The percentage of non-compliance with medication in patients with schizophrenia is as high as 40–50%, and 74% of patients discontinue their medication within 18 months. Furthermore, Wunderink and colleagues report that dose reduction or discontinuation of antipsychotics during the early stages of remitted first-episode psychosis is associated with superior long-term [7 years] recovery rates [40·4%] compared with the rates achieved with antipsychotic maintenance treatment [17·6%]. Additionally, Morrison and colleagues reported that cognitive therapy significantly reduced psychiatric symptoms and seems to be a safe and acceptable alternative for people with schizophrenia and related disorders who have chosen not to take antipsychotic medication. In consideration of low patient compliance with antipsychotics, evidence for improved long-term functional recovery with dose reduction or discontinuation of antipsychotic medication, and the promising results from trials of psychological treatments, intervention options for patients with a psychotic disorder are clearly needed that are effective, have fewer side-effects, and are more acceptable to some patients than antipsychotics.
11.1.1 Effectiveness of cognitive behaviour therapy There is a consistent evidence base suggesting that many people find CBTp helpful. Other forms of therapy can also be helpful, but so far it is CBTp that has been most intensively researched. There have now been several meta-analyses [studies using a statistical technique that allows findings from various trials to be averaged out] looking at its effectiveness. Although they each yield slightly different estimates, there is general consensus that on average, people gain around as much benefit from CBT as they do from taking psychiatric medication…The National Institute for Health and Care Excellence [NICE] considers the evidence strong enough to recommend that everyone with a diagnosis of schizophrenia should be offered CBT. NICE recommends that people should be offered at least 16 one-to-one sessions over a minimum of six months. However, this is far from being the case everywhere: indeed the Schizophrenia Commission found that only one in ten people who could benefit from it have access to good CBTp. We view this with grave concern – indeed, it has been described as scandalous…
11.10 Conclusions There is now overwhelming evidence that psychological approaches can be very helpful for people who experience psychosis. However, there remains a wide variation in what is available in different places. Even the most successful approaches, such as early intervention and family work, are often not available, and nine out of ten of those who could benefit have no access to CBT. There is a pressing need for all services to come up to the standard of the best and to offer people genuine choices. Perhaps most importantly, we need a culture change in services such that the psychological understanding described in this report informs every conversation and every decision…
There was the phenomenal work of Anthony Morrison, who is the first researcher to empirically show that psychotherapy can be effective with individuals diagnosed with schizophrenia, even when they choose to not take psychotropics. Although many know this intuitively, the scientific community is not really interested in intuition; for him to show this repeatedly through empirical data is profound.
Sorry, the comment form is closed at this time.