[recent releases not shown]
Among other things, one major change from the psychiatry I began with and the modern era was that I didn’t know which company produced which drug – or for that matter, which ones were on or off patent. I thought of the TCAs [Tricyclic Antidepressants] and the MAOIs [Monamine Oxidase Inhibitors] as primarily drugs for patients with Major Depression [what we called Major Depression back then meaning Melancholia, Manic Depressive Illness with a Depressive Episode, etc] and not for the outpatients where my own focus had landed. I don’t remember discussing them for children or adolescents. In my six month fellowship on an adolescent treatment unit, no kid was on antidepressants. I certainly recall talking about "kids being depressed," but never about them "having" a depressive illness. Recently, on an impulse, I found an old $0.01 copy of the late 1960s GAP [Group for the Advancement of Psychiatry] Psychopathological Disorders of Childhood we used and ordered it. It was as I recalled. The only mention of depression was in a listing of symptoms, but no diagnostic entity.
So I’m pretty sure that the existence of the then newer antidepressants created the diagnostic entity «Depression» in children and adolescents, and I’m even more sure that the hype that built around the drugs perpetuated the diagnosis «Major Depressive Disorder» in Adults. As things developed, the phrase «Treatment Resistant Depression» [with an acronym of its own – TRD] found wide usage in both kids and adults, as if it was itself also a diagnostic entity. I can’t right off think about other such situations, places where a treatment had such a profound effect on the creation and shaping of a diagnosis. I also wonder if there has ever been a single drug class that has been so heavily studied or had so much energy, time, or money spent trying to magnify a weak effect [sequencing, combining, augmenting, "personalizing", etc].
Since finally finishing the Study 329 RIAT project, I’ve been thinking about what else this Antidepressant Era in psychiatry might have to tell us for the future – assuming it’s finally drawing to a close. PHARMA seems to have genuinely flown the coop, moving away from CNS research for the most part. I hope, on psychiatry’s side, that free of the influences of PHARMA and KOLs, these drugs can be evaluated for their true worth and indications. We’re all so locked in to the polarized rhetoric that it may be a while before all the meta-analyses and retrospectives might offer some clarity. But I think that there’s perhaps a larger contribution that can be made to Medicine in general.
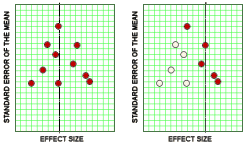
I had no idea that such a thing could happen, that the tools of scientific investigation could be so regularly perverted in plain sight. For example, that by withholding negative studies, one could actually create the illusion of a clinically relevant medication from a compound with a trivial effect. It makes perfect sense if you’ve seen it before. I just never would’ve thought to look.
Paroxetine resulted in significantly greater rates of response (defined as Hamilton Rating Scale for Depression [HAM-D] score <8) compared with placebo in the last observation carried forward population. Response rates were higher for paroxetine (76%; P=.02), imiprarmine (64%), and placebo (58%) among those patients who completed the 8-week trial. There was no statistically significant difference between paroxetine or imipramine and placebo on the HAM-D total score at end point. However, there was a significantly greater increase in the Clinical Global Impression (CGI) improvement scores for the paroxetine group compared with the placebo group.
In every specialty, a lot of the clinical side of medical training is learning to see a lot of patients in a practice day, process a ton of information, and get to the point where you almost automatically hear bells go off when some small piece of information comes your way that says, "stop, look, and listen" – some symptom that doesn’t fit, a hint that this cough is the early symptom of tumor instead of a cold, this rash is going to turn into a Stevens-Johnson syndrome in an hour, this back pain is an aneurysm about to dissect. Over these last few years of reading the psychiatric Clinical Trial literature, I’m beginning to hear those same bells when I scan through a Clinical Trial journal article. And I wish my training for reading these articles had been as rigorous as my bedside and consulting room training.
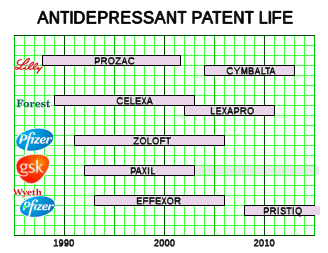
As peculiar as it might sound, I think that a big segment of the literature [particularly the industry funded Clinical Trial literature] that came out of the antidepressant era spanning the time in that top figure needs to be formally re-evaluated, not just to get a more accurate picture of these drugs, but also to familiarize all of us to the subtle ways it can be distorted – something like clinical training in journal reading. It’s certainly a treasure trove of tricks that ride just this side of fraud. While I’ve yet to find one of these studies where the data has been directly changed, I can’t think of any, off-hand, that played it totally straight in the analysis/presentation/conclusion realm either. We’ve always said doctors should be taught critical reading. It’s obvious that we’re woefully off the mark in that area when it comes to Clinical Trials. This kind of shenanigans isn’t just a problem in psychiatry. It’s medicine-wide. But psychiatry sure has the biggest library of examples on the block. We might as well find a way to use those papers to some decent purpose.
Mickey,
Good article here; as usual you’re right on about the problems with hiding most negative studies, magically twisting other (mostly) negative studies into positives, and adding response measures into the study later on.
When I read these, as an outsider, it is still amazing that such focus is put on one class of intervention (medication) usually over short time frames (of weeks or a few months). But it must make sense in the totally profit-driven, shareholder-beholden, next-quarter focused environment that these companies operate in. Otherwise these drugs wouldn’t continue to be overused nor their supposed benefits misrepresented.
I wonder what it would take to generate fairer studies and more longer term studies, some of them also including comparisons to non-drug psychological interventions. Probably it would take a lot more government control and regulation of these companies, but that is something that would be fiercely resisted.
Edward,
Your point leads to many topics. These Clinical Trial articles are really for FDA Approval, and the FDA mandate has always been about safety. Efficacy was a 1962 add-on that was designed to keep inert snake oils off the market. The onus on proving usefulness long term has been on medicine itself, not the FDA. There are lots of ways that gets done traditionally, and it is one of the functions academic medicine has always taken on. Review articles, long term studies, etc. So you’re pointing to something important. The alliance between academic medicine and PHARMA seems to have interferred with the “watchdog” function of academia. These KOLs in academic medicine aren’t focusing on keeping practitioners appraised. That’s actually why they’re so powerful. We’ve looked to them for guidance, long after leaving our own training. PHARMA’s invasion of CME [continuing medical education] is another place where that may be in play. Doctor Carroll was trying to explain that earlier to Sally [here]. These short term trials were never intended to be the final word on anything. Just a way to make sure that the medicine was, in fact, medicine. Making sure it is “good medicine” is something else entirely…
And “treatment-resistant depression”!!! It is defined by unsuccessful — and possibly iatrogenic — drug treatment. Even the label suggests a fallacy.
“….benign sentences that are anything but benign [that example will become much clearer in a couple of weeks].” — Are you referring to the Study 329 re-analysis? I can hardly wait.
Mickey,
I’ve followed you for years, and appreciate all the analytical work you’ve done. I won’t get on my soapbox, but when you say This kind of shenanigans isn’t just a problem in psychiatry. It’s medicine-wide. , I scream a hearty “AMEN.”
These sorts of shenanigans are indeed medicine-wide. You may remember I spoke of the approval of rDNA insulin, where the primary metric used to garner approval was that “it lowered blood glucose just like natural animal insulins.” We (the Type 1 population) are still waiting for the promised safety studies, which somehow seem to have been shoved to the back burner as PR has successfully morphed T1 and T2 diabetes, implying they are more or less the same disease. With the number of T2, and the huge profits to be garnered there, the ‘safety and efficacy of new insulins’ (as far as I can tell) is still (30 years later) not being evaluated.
(Like I said, I’ll cede my soapbox now.)
Melody
Just curious – do you really think that there are *no* children/adolescents with major depression? I knew someone who was 15, withdrew, stopped eating, ran incessantly to try to boost mood, cried, stopped being able to concentrate, and got slightly paranoid. There’s clearly an epidemic of over-prescribing. I just wonder whether there aren’t some cases where it might be appropriate–but only under the care of a skilled child psychiatrist.
While I take your point, I would say that she has a symptomatic depression. That doesn’t preclude trying medication under the conditions you describe. I’ll admit to being kind of ideological here in that I’m arguing against the entity Depression, not the symptom depression. In a 5 year stint at a child and adolescent clinic, I saw kids like you describe, but they were depressed for a reason and responded to approaches that addressed the reason – usually things that involved both family and outside forces. A few were medicated “under watch.” It may have helped a few – it’s hard to say.
I’m conflicted talking about this myself because I don’t think that adults with milder depression, the kind of people we see in practice, have an entity Depression either. My main reason for thinking that is subjective. Those patients respond to psychotherapy, the “talk therapy” of old. So I’m admitting that my psychoanalytic background could be [and maybe should be] considered a COI. In the adults, medications often help those with more severe depressive symptoms – the kind that interfere with function. So I think of the SSRIs as symptomatic medications and prescribe them accordingly.
I might add that in days gone by, we thought of depressive symptoms as being connected with helplessness, or loss, or anger. Such thinking is out of fashion in public places, but in the privacy of a “talk therapy,” it’s as valid and useful a way to think as it ever was…
Thank you, as ever, for that very rational approach, Mickey.
15-year-olds experience a lot of hormonal changes that may affect their moods and behavior.
We have a bizarre idea that “normality” is being cheerful and productive all the time. Not so, although the myth suits the purpose of a society that requires its worker bees to be constantly busy.
1bom & EastCoaster,
I would be extremely interested on thoughts around a specific corollary to your discussion, namely whether there exists pediatric Melancholia. Not whether it is “common”, or even as “common” as in adults, but whether or not it, at least in some form, can exist.
My preliminary impression is that during the era where Melancholia’s unique position was better appreciated, there was unfortunately a bias (perhaps related in part to views within some psychoanalytic schools of thought?) against the idea that such entities could be present in children. And, that during the more recent era when the latter bias has faded, that unfortunately so too has faded the appreciation of Melancholia (vs the all encompassing garbage bag label of MDD).
I would find an exploration of Pediatric Melancholia fascinating.
1BOM: I think you are being ideological, or over-generalizing, about the issue of adolescent Depression. I agree that psycho-social circumstances are the main source of despair for children and adolescents, and that many of the depressive syndromes at that age are reactive. That said, classic Manic-Depression does exist in adolescence; post-psychotic depression also exists, and various substance induced depressive syndromes. Reactive depression can be very severe and debilitating, to a degree where psychotherapy or change of problematic living environments fail to help.
[I am a child and adolescent psychiatrist working in an in-patient unit, and so I get to see the extreme cases].
http://online.liebertpub.com/doi/pdf/10.1089/104454603322572552
http://1boringoldman.com/index.php/2011/07/22/tuning-the-quartet/#comment-214257
http://1boringoldman.com/index.php/2011/07/22/tuning-the-quartet/#comment-214257
I am not sure who are the child psychiatrists who are studying capital D depression in children (NOT MDD) and who are working with the rigor and respect for clinical trial data that Dr. Carroll describes. I’m not sure why many of the mentees described above (e.g., Ryan, Brent, Birmaher) don’t seem to have done so.
Gad Mayer & 1boringyoungman,
Teach us something here. Always willing to learn…
Yeah, I want to hear about all that psychotherapy being done on inpatient units these days, and how insurers are so willing and able to add hospital day stay coverage so patients can work on framing and coping skills.
Oh, my bad, I should clarify that I am not talking about framing how to take the meds and cope with the side effects…
Is this correct? It’s Wagner’s sentences.
1. Paroxetine resulted in significantly greater rates of response (defined as Hamilton Rating Scale for Depression [HAM-D] score <8) compared with placebo in the last observation carried forward population.
(Mania?)
2. Response rates were higher for paroxetine (76%; P=.02), imiprarmine [sic] (64%), and placebo (58%) among those patients who completed the 8-week trial.
High than what? I guess it means that after 8 weeks in the study, people in a given group scored higher than did people in the same group who did not complete the study. If some drop-outs were for adverse events and side effects, that's to be expected.
That's two meaningless statistically significant "advantages" of 8 weeks on paroxetine. versus non or fewer.
So:
HAM-D scores fell below 8 in a higher percent of people who didn't want to take, or could not take paroxetine for 8 weeks than among untreated people. (But they didn't stick around for more.)
HAM-D scores fell below 8 in a higher percent of people who managed to take paroxetine for 8 weeks than among people who didn't.
Any early advantage of paroxetine over placebo was lost after 8 weeks, and the advantage could have been hypomania or mania.
The insidious thing about psych drugs is that adverse events are often psychiatric. The user becomes immoral, irresponsible, or outright manic or psychotic. Any of these can cost a marriage, parental rights, a career (think medicine, teaching, or law), or life savings, as well as lifelong friends and well-earned social standing.
If the drugs made users’ ears fall off there would be huge court awards for the earless.
But drug-induced behavioural changes are hard to prove, especially if the patient was depressed or anxious at the outset.
That is tragic toll of manipulating study design and data. The harms can be life-wrecking and there is no recourse.
It’s now sort of bubbling up that the drugs remodel the hardware of the brain. It’s not just intoxication that alters behavior and emotion, it’s (in my opinion) brain damage. There’s been no chance for users to give informed consent to have their brains re-designed. They were only told about shifting chemical balances. This should be the lawsuit of the Cenozoic era.
The conclusion of this post is a good place to start-
“And speaking of purpose. I gave two small examples. One was not publishing negative studies. The other was carefully cherry picking things to say that put a positive spin on a decidedly negative study. Those are both wrong on purpose – deliberate attempts to deceive. There’s no statute of limitations on deliberate deceit, AKA lying. Our literature on Clinical Trials is riddled with deliberate deceit, and it’s time to start naming it for what it really is. This story needs a heading that fits.”
Don’t we already know that fraud- lying to sell your product, is a crime?
I think the hesitancy to call this what it is- a crime against humanity, in the truest sense, is a matter of sizing up the giant– and then wondering:
How can we put the blindfold back on Lady Justice … ?
1boringyoungman: “I am not sure who are the child psychiatrists who are studying capital D depression in children (NOT MDD) and who are working with the rigor and respect for clinical trial data that Dr. Carroll describes.”
I don’t have much to add, except to (apocryphally) quote Willie Sutton, who, when asked why he robs banks, said: “Because that’s where the money is.”