When March Madness time comes around, I always remember a time when it wasn’t about Basketball for me – during the decade when I was a Psychiatric Residency Training Director. That may sound like an honorific, but that’s not how it was. I was only a year beyond my own residency and wasn’t exactly recruited, I was conscripted amid a crisis when my predecessor abruptly quit. But "we need you to fill in" lasted for a long time. And during those years, March Madness referred to Match Week – the week in which we found out what residents were or were not coming for next year. A few years ago, I had a nostalgia attack and made a graph of the history of Match Week in psychiatry [fuzzy math…]. As you can see, 1978 wasn’t a time when psychiatry was high on the list – filling only about half the positions offered. So Match Week was a frantic period because there was much ado thereafter with the flow into psychiatry from outside the Match to negotiate.
Also for 1978, it was a circus. It was at the end if Deinstitutionalization, the end of the Community Mental Health Movement, just after the Viet Nam War, and a peak time for the ideological and guild battles in mental health. We often think of the modern era in psychiatry beginning in 1980 with the DSM-III’s publication, and in a way that’s true. But at the same time, it was the end of a whole lot of other things – very loud things. Actually, the graph accurately reflects how it felt through that first post-DSM-III decade. Things just seemed to calm down.
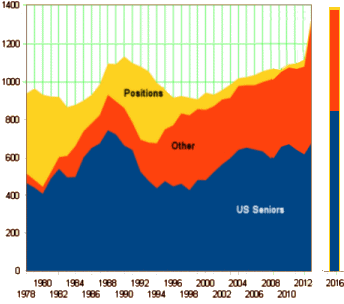
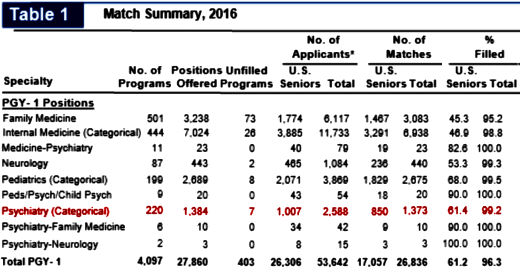
The dip from around 1988 until 2004 spans the period when I started a practice until I retired, so I was otherwise occupied, ergo I know nothing about the why? of the dip. Here are some selections and comparisons from the info about the 2016 match that came out yesterday [this was Match Week], and I added 2016 to the graph above:
The specialty choices of medical students is a broad topic, but it usually reflects something about the state of the specialty. The medical students are influenced a lot by their contact with attending physicians and residents they meet on their clinical rotations. And 2016 looks like business as usual [in fact, I’m a little surprised to see no effect from the turmoil one might’ve predicted from reading our various blogs].
Sandra, you had asked a question earlier:
http://1boringoldman.com/index.php/2016/03/25/the-agenda/#comment-263804
“I had two main messages in my BMJ paper about the Maudsley debate, which are my personal views after having gone through the science: psychiatric drugs are the third leading cause of death; and we would have a healthier and more long-lived population if we only used 2% of the drugs we currently use. Tovey et al. felt I went too far with this recommendation. I believe that my impending book (4) will fully justify my assertions.”
http://www.bmj.com/content/350/bmj.h2435/rr-14
“We could stop almost all psychotropic drug use without deleterious effect, says Peter C Gøtzsche, questioning trial designs that underplay harms and overplay benefits.””Psychiatric drugs are responsible for the deaths of more than half a million people aged 65 and older each year in the Western world, as I show below.1 Their benefits would need to be colossal to justify this, but they are minimal.”
Maybe Allen was thinking of a quote from Gøtzsche’s work favorably on a number of occasions.
I was struck by this phrase in the CE program at MIA:
“A review of the unbiased research on the effectiveness and risks of psychiatric medications by Nordic Cochrane director, Dr. Peter Gøtzsche of Denmark.”
http://madinamericacontinuinged.org/courses/why-few-patients-benefit-from-psychiatric-medications/
I know that many (you, 1bom, Bernard Carroll) have spoken to financial biases. Do you agree that the science indicates that psychiatric medications are the third leading cause of death annually in the Western World? Do you agree that we could stop almost all psychiatric medications without deleterious effect? Do you view as Gøtzsche as coming from an unbiased position?
I mean, it does seem difficult to view Gøtzsche’s position as anything other than stating that an unbiased review of the clinical science is that psychiatrists as a whole are killing a very large number of people with psychiatric medication and providing practically no benefit with those medications.
“Gøtzsche is neither crackpot nor zealot. He’s a scientist who gives his life to something of value.”
http://1boringoldman.com/index.php/2013/11/25/a-major-force/
If Gotzsche is not a crackpot, not even rising to the level of a zealot, is his unbiased review of the clinical science on the relative harms and benefits of psychiatric medications as a whole essentially correct? That they kill half a million people a year with practically no benefit?
To ask a more provocative question than usual: If Gøtzsche is not grossly incorrect, then isn’t focusing on trying to reclaim psychiatric practice from the last 20-30 years of pharma intrusion, trying to emphasize n of 1 practice and the individual needs of patients with psychosis or ADHD, a bit like fiddling while Rome burns? When as a profession we’d be killing that many people a year? When having doctors stop prescribing psychiatric drugs entirely would save five million lives in the coming decade?
Interestingly, I cannot recall seeing Drs. Carroll or Psycritic comment on Gøtzsche’s overall message. Don’t know what to make of that.
As a corollary: Gøtzsche may feel that we were killing people on a smaller scale in the 60s, 70s, and 80s with psychiatric medications, but I haven’t seen anything that suggests he thinks that we were not, on balance, almost entirely doing harm with those medications back then either.
If what you say about Dr. Gotsche is accurate then it seems overstated to me. There are recent population level data that indicate antipsychotic drugs are associated with clear reductions of overall mortality as well as suicide rates in patients with schizophrenia diagnoses. Likewise, I have estimated that any antidepressant drug-provoked suicides in depressed youth are offset by a reduction of depression-related suicides. I don’t disagree that psychotropic drugs are often used inappropriately, but we wouldn’t want to throw out the babies with the bathwater.
Here is a better link for my commentary on antidepressants and youth suicide.
Back to the topic of the post: the least healthy groups in the Table are Family Medicine and Internal Medicine. These are the very groups who prescribe most of the psychotropic drugs on a population basis. They also are the groups most prone to view antidepressant and antipsychotic drugs as broad spectrum agents for which careful diagnosis is unimportant.
Dr. Carroll,
What I said about Dr. is based on his writings here in the BMJ, if you have the interest:
http://www.bmj.com/content/350/bmj.h2435
http://www.bmj.com/content/350/bmj.h2435/rr-14
The message that an “unbiased” review of the clinical science is that practically all psychiatric medications should cease to be prescribed and that they kill millions seems clearly stated. If he is not considered even overzealous, of such a message is not felt to require a strong challenge, then it is hard to imagine that even those physicians (psychiatrists AND primary care) who have deep concerns about over-use of psychiatric medications (including in primary care) will find common cause. We seem to be in dire need of less ideologically driven pieces in our clinical literature (from the likes of Gibbons, Thase,…etc). One of the joys of reading 1bom and tie writing is that the presence of a clinically driven and critical intellect. That remains sharp even if se of what you are reading falls in line with your beliefs. I point many colleagues to each of your writings. When I have been asked why what read like extremist screeds about psychiatric medications from Gotzsche, dressed in the trappings of EBM, don’t seem to get challenged as sharply… I don’t really know. Don’t know how other physicians (psychiatrists or primary care) canals common cause if Gotzsche’s position doesn’t even represent zealotry. If I have created straw men out of what Gotzsche has actually said then my sincere apologies. I find myself very drawn to some of his arguments. It simply feels that there is either very serious flaws to his analyses, or that psychiatric prescriptions should simply stop. Do feel that the serious biases/flaws in his analyses should be addressed and/or it should be addressed why his message to end prescription of all psychotropics is not being embraced.
.
Because of his analyses are not deeply flawed/biased in some way then why would one not embrace his message to pretty much end the prescription of any psychiatric drugs?
“Back to the topic of the post: the least healthy groups in the Table are Family Medicine and Internal Medicine. These are the very groups who prescribe most of the psychotropic drugs on a population basis. They also are the groups most prone to view antidepressant and antipsychotic drugs as broad spectrum agents for which careful diagnosis is unimportant.”
That’s why I listed them. I remember my Internal Medicine days and how I thought of medications back then. There was a lot more of the Algorithms/Guidelines kind of thinking. «If you see this, give this». «If you see that, then give that». My concern is that psychiatrists have increasingly moved [or been moved] in that direction eg med checks, therapist psychiatrist splits, Integrative or Collaborative Care, etc. My other concern is that the Internists, Family Practitioners, Primary Care Docs, and to some extent, the brief-visit psychiatrist are all in the same boat – having only one modality of treatment to offer [“If your only tool is a hammer, everything looks like a nail”]. I wouldn’t have wanted to tak up prescribing psychiatric meds in my Internist days.
After a long period of not prescribing much medication because of the specific nature of my practice, I started working in a “clinic,” something I hadn’t done in years. Before, I was seeing patients weekly for full sessions, and so I heard all about the effects of the medication. I realized in a “clinic,” it would be different, so I bought all the recent texts, planning to “bone up” on the medications. They were disappointing to a fault, at least for me. They were filled with science and biochemical info, but not what I was looking for – side effects, doses, indications, duration of treatment, dangers, case studies. More than anything, I wanted case studies. I enjoy science as much if not more than the average person, but it was the clinical stuff that was missing.
I had to learn about akathisia by causing it, and withdrawal syndromes, and the metabolic syndrome, etc. I hadn’t expected that. And even though it was three or four years after the black box warning, it wasn’t in the text books. I tried the review articles and though they were slightly better, the emphasis is on slightly. What I’m getting at is the comment “I don’t disagree that psychotropic drugs are often used inappropriately, but we wouldn’t want to throw out the babies with the bathwater.”. I agree. If we regulated medications that had side effects and toxicity by throwing them out, we wouldn’t have much to work with. As David Healy often says, “all drugs are poisons.”
It’s not the drugs that are the problem. They’re just chemical compounds. It’s how the drugs are used that matters, and our literature is the place where we have traditionally learned about them from others instead of just relying on our own experience. My experience doesn’t fit with Dr. Gøtzsche’s, but he’s not to be discounted. Our drugs vary a lot in both efficacy and safety and they need to be used carefully and cautiously. There are times when they can be quite helpful, and times when they’re the opposite. My sermon wouldn’t aim at getting rid of them, but more towards getting to know them much more intimately, and about returning to the now rarely used case report format to describe their actions. I only see one patient at a time, and I’d like to see our literature heading back that way.
There is one place, however, where I really do want to throw out the whole bathtub – Direct to Consumer advertising. Those ads create expectations for efficacy and safety that directly interfere with the practice of medicine…
The quote in the Francis article was not attributed to Gotzsche, it was attributed to Whitaker. My understanding of putting quotes around a phrase is that it indicates the words are directly attributed to the person named.
As for my own views on psychiatric medications, I have made my views clear on the antipsychotic drugs in multiple blogs.
My views on the SSRI’s are largely in agreement with Dr. Nardo but in general I think their benefits are generally inflated and their risks understated by many who prescribe them with great regularity.
SS,
Sorry for my not having been clearer. Allen Frances was mistaken in attributing the quote to Whitaker and has now appended a correction and apology to that effect to the post. I meant only to say that the quote sounded more like something that Gotzsche might have said, but it may very well have not been said by him either.
.
I do agree with Frances that biases come in many forms, not simply financial, and that lack of financial COI does not equal unbiased. I do not discount Dr. Gotzsche, but my bias is that his assessments of the potential risk/benefits of the totality of psychiatric medication prescribed is driven in no small part by factors other than an unbiased reading of the clinical trial literature. I also hold the bias that views based almost solely on that literature, and divorced from clinical experience, does not necessarily trump clinical experience.
.
I find your Slow Psychiatry reflections an intriguing conceptualization BTW. Thank you for sharing them.
If you read these case histories from a wide cross-section of people taking psychiatric drugs http://survivingantidepressants.org/index.php?/forum/3-introductions-and-updates/ , it’s perfectly obvious the drugs are overprescribed by both psychiatrists and non-psychiatrists and adverse effects are poorly recognized by all doctors.