THE COLLABORATIVE CARE MODELAMERICAN PSYCHIATRIC ASSOCIATIONACADEMY OF PSYCHOSOMATIC MEDICINESpring 2016There is expert consensus that all effective Collaborative Care Models share four core elements: [1] team-driven, [2] population-focused, [3] measurement-guided, and [4] evidence-based. These four elements, when combined, can allow for a fifth guiding principal to emerge; accountability and quality improvement. Table 1 reviews the core elements of Collaborative Care implementation. Collaborative Care is team-driven, led by a PCP with support from a "care manager" [CM] and consultation from a psychiatrist who provides treatment recommendations for patients who are not achieving clinical goals. Other mental health professionals can contribute well to the Collaborative Care Model. Collaborative Care is population-focused, using a registry to monitor treatment engagement and response to care. Collaborative Care is measurement-guided with a consistent dedication to patient-reported outcomes and utilizes evidence-based approaches to achieve those outcomes. Additionally, Collaborative Care is patient-centered with proactive outreach to engage, activate, promote self-management and treatment adherence, and coordinate services.
Table 1: Essential Elements of Collaborative Care Team-Driven: A multidisciplinary group of healthcare delivery professionals providing care in a coordinated fashion and empowered to work at the top of their professional training. Population-Focused: The Collaborative Care team is responsible for the provision of care and health outcomes of a defined population of patients Measurement-Guided: The team uses systematic, disease-specific, patient-reported outcome measures (e.g., symptom rating scales) to drive dinical decision-making. Evidence-Based: The team adapts scientifically proven treatments within an individual clinical context to achieve improved health outcomes.
John has recently moved out of his house, and he and his wife are separating. He is staying with a friend in town…
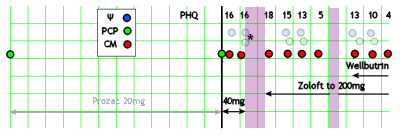
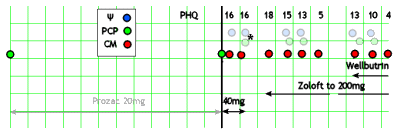
After a month on the higher dose of Prozac, the patient stops it because of jitters. They’re following him with the PHQ-9 and it goes up. The Psychiatrist suggests changing to Zoloft and has a phone conversation with the PCP about titration [the only direct contact between the Psychiatrist and the PCP recorded]. The patient doesn’t fill the Rx, and a month later, he’s worse. Contacted by the CM, he finally starts the Zoloft and the dose is gradually increased. After several months, the patient is feeling better and he and his wife are "fighting less." 5½ months after the initial contact, he’s back with his wife and feels fine [PHQ-9 is 5]. But two weeks later, he stops the Zoloft, and some of symptoms return and persist, in spite of restarting the Zoloft at a maximum dose. The psychiatrist suggests adding Wellbutrin and later increases the dose. At 9½ months from first contact, he is better and his PHQ is 4.
-
The psychiatrist never saw the patient, and as best I could tell only had one direct contact with the PCP. If the PCP had contact along the way when changing the medications around, it wasn’t apparent. It appears that contact was through the CM [though surely that’s not right with changing drugs and titrating doses?].
-
A PHQ-9 and some comorbidity screening don’t a diagnosis make [did they actually make a diagnosis?].
-
A PHQ-9 is hardly a precise clinimetric. I’d prefer asking, and I’m pretty sure patients prefer being asked.
-
There are two instances where a high dose SSRI is stopped with no taper. Both suspect for withdrawal [particularly the first] but were interpreted as worsening!
-
What about "John has recently moved out of his house, and he and his wife are separating. He is staying with a friend in town..." Have we just forgotten that a loss like that can cause all of these symptoms? What were the details? Who left who? Is there a clinician in the house?!
-
Given that he got ill when they separated and got better when he moved back in, so I doubt that the Zoloft had much to do with anything [except maybe withdrawal]. It could he that he was just plenty glad to be home…
Robert Whitaker, one of psychiatry’s major critics had this to say about where he thought psychiatry might head in the future [see still around…]:
… So I don’t believe it will be possible for psychiatry to change unless it identifies a new function that would be marketable, so to speak. Psychiatry needs to identify a change that would be consistent with its interests as a guild. The one faint possibility I see – and this may seem counterintuitive – is for psychiatry to become the profession that provides a critical view of psychiatric drugs. Family doctors do most of the prescribing of psychiatric drugs today, without any real sense of their risks and benefits, and so psychiatrists could stake out a role as being the experts who know how to use the drugs in a very selective, cautious manner, and the experts who know how to incorporate such drug treatment into a holistic, integrated form of care. If the public sees the drugs as quite problematic, as medications that can serve a purpose – but only if prescribed in a very nuanced way – then it will want to turn to physicians who understand well the problems with the drugs and their limitations. That is what I think must happen for psychiatry to change. Psychiatry must see a financial benefit from a proposed change, one consistent with guild interests.
John J.
John J. is a 48-year-old white male visiting his PCP, Dr. Stevens, for a follow-up visit for managing hypertension. During the visit, John’s PHQ-9 score is taken and found to be 16, in the moderate range for major depression. John was treated by Dr. Stevens 12 months ago for depression and remains on fluoxetine 20 mg daily, to which he had a fair initial response. This is John’s first PHQ-9, part of the new Collaborative Care protocol instituted by Dr. Stevens’s clinic.
Dr. Stevens discusses the test results briefly with John during their clinic appointment and introduces him to Ms. Cook, a CM/behavioral health specialist with the clinic’s Collaborative Care team. Ms. Cook is immediately available in the clinic to meet patients coming and going from appointments at the request of the PCP or other clinic staff. John agrees to speak with Ms. Cook after the appointment, and Ms. Cook runs through a few patient screens for behavioral health and substance use conditions that are often comorbid with major depressive disorder. John screens negatively for alcohol use or a history of mania. Ms. Cook discovers that John has recently moved out of his house, and he and his wife are separating. He is staying with a friend in town, and it has been hard for him to make it to work consistently. He often goes to bed late and sleeps in, missing his alarm in the morning, and eventually calls in sick. Ms. Cook shares some of this initial information with Dr. Stevens after their appointment, and Dr. Stevens increases John’s fluoxetine to 40 mg daily. She also engages him in a behavioral activation strategy to improve his mood that includes getting together with his friend Joe over the weekend.
Three days later, Ms. Cook has her weekly meeting with Dr. Brown, the consulting psychiatrist. They discuss John, the new addition to Ms. Cook’s caseload. Dr. Brown acknowledges the PHQ-9 score and the fluoxetine increase and reminds Ms. Cook of additional brief intervention techniques she has reviewed in the past with other patients. Five weeks later, during their caseload review, Dr. Brown notices John’s PHQ-9 score is unchanged. Ms. Cook notes that he stopped taking the fluoxetine the week before because of some ongoing jitteriness. Dr. Brown recommends switching to sertraline instead, and Ms. Cook conveys the recommendation to Dr. Stevens by flagging him in the electronic health record. Dr. Stevens reviews John’s other medications the following day and writes a prescription for sertraline after Ms. Cook has called John to discuss the recommendations of the consulting psychiatrist. John agrees to try the sertraline. Ms. Cook reviews the side effects with John and offers her contact information in addition to Dr. Stevens’s office if he has any problems with the medication. Dr. Stevens phones Dr. Brown and asks about the titration schedule of sertraline and starting dosage to confirm his management is appropriate. They agree to continue with increases in this medication with a target PHQ-9 of less than 5 if possible.
Five weeks after his last appointment, John remains depressed. He did not return Dr. Stevens’s last call regarding some recent lab results, and he no-showed one appointment. During their weekly caseload review, John is eighth on Ms. Cook’s list of 58 patients when sorted by PHQ-9 score severity which leads to a case review. Their registry of patients also has flagged John’s PHQ-9 as overdue and above their target. As she and Dr. Brown are reviewing all the patients, they review John’s score and with the information in the registry are able to quickly recall his latest treatment plan, including the sertraline recommendations. Dr. Stevens did write the prescription, but Ms. Cook is unsure what happened after that. She attempted to call John about 1 week after the sertraline was prescribed and left him a message that wasn’t returned. Ms. Cook and Dr. Brown agree that John needs increased outreach given his recent depression and lack of engagement, and Ms. Cook takes on this task over the next week. They then move on to Sue after spending about 5 minutes discussing John…
The following day, Ms. Cook writes a letter from the clinic to John offering assistance and begins to call more frequently. Three days later, John calls back, and he discloses that he never picked up the sertraline and was not sure he was worth the attention of the team. He reports that he didn’t want to feel like a failure again or let anyone down. John’s PHQ-9 score over the phone is 18, and Ms. Cook screens John for suicidal ideation, which is negative. She provides some education around depressive symptoms, the role of the team, and their desire to help him feel better. John agrees to pick up the sertraline from the pharmacy and check-in with Ms. Cook before the weekend to report on how he’s tolerating it.
John, the patient, calls Ms. Cook, the CM, on Friday and reports that he picked up the sertraline and is taking it without side effects but doesn’t feel much different after 2 days. Ms. Cook reassures John that this is not unusual, and that he needs to stick with the medication for 4-6 weeks at the right dose sometimes before his mood may change. They make a plan to check in once a week. In 4 weeks, John’s PHQ-9 score has gone from an 18 to a 15, and he is tolerating the sertraline without any problems. Dr. Brown, the consulting psychiatrist, recommends they titrate the dose to a higher level and continue to monitor John’s response. Dr. Stevens, the PCP, writes a new prescription for John; Ms. Cook confirms that he picks it up at the pharmacy and takes it; and after another 4 weeks, his PHQ-9 is 13. John reports that he is feeling better and has applied for a new job. He and his wife are fighting less, and they are talking about having him move back in. In spite of these gains, however, Ms. Cook discusses John’s remaining symptoms of prominent guilt and negative self-worth and poor quality sleep, energy, and concentration coupled to overeating—all of which contribute to his current score. They formulate a plan to begin more regular exercise. Because his PHQ-9 is still above 5, Dr. Brown’s advice is to continue to titrate the sertraline to the maximum daily dosage, noting his steady improvements.
Four weeks later, John’s PHQ-9 score is 5. He reports that he feels like his old self again, has moved back in with his wife, is exercising more regularly now, and starting to lose some excess weight. Two months after John achieved early remission from his depression, Ms. Cook calls him for a routine check-in. He notes that he stopped taking the sertraline for a couple of weeks right after their last conversation and had a relapse of some of his symptoms. His PHQ-9 score has jumped from 5 to 13, and John is feeling embarrassed and shameful.
He resumed his sertraline at 200 mg about a month ago but still struggles with energy and has stopped his workout routine. Dr. Brown suggests that they augment the sertraline with bupropion, and Dr. Stevens writes the prescription for John. One month later, John’s PHQ-9 score is 10, and Ms. Cook engages him with Behavioral Activation focused on his exercise regimen again. They discuss the cycle of inaction, guilt, and depression, and John agrees to experiment with a different workout regimen and assess his mood. Dr. Stevens automatically adjusts his bupropion to a higher level since he is tolerating it well, and 1 month later John’s PHQ-9 score is 4.
Collobo-care implies that your mental status examination is no better than any other professional in the chain. Who is comfortable with that?
I thought people went into pathology, not psychiatry if they didn’t want to interview live patients.
Note the all the catchphrase managerial BS speak in this article.
The APA seems to be interested in this and psychiatric residencies at the same time. I don’t know why because the former renders the latter useless.
If this won’t convince psychiatrists to drop the APA I don’t know what will. An organization fighting hard to make you obsolete.
No one ever takes time to talk to this patient, which is terrible. And certainly no one suggests therapy to him. I am appalled by this model and wonder about what kind of person will be attracted to practicing this way.
Dr. Fuller, I agree and what is galling is that if anyone talked like this article does about acceptable standards of care 25 years ago, they’d be thrown out of the doctor’s lounge or case conference.
It’s all about APA politicos loving the group health aims of Obamacare, and trying to shoehorn the MOST individual-based specialty into a population health model. It is absolutely fatally flawed but it’s their secular religion, and that usually wins over logic.
Wow. They were actually publishing that case report as something to emulate? Did they actually bill for such useless activity?
The patient most likely had adjustment disorder with depressed mood and couple’s counseling would probably have helped more than anything.
They did a couple of screens for alcohol abuse??? I can’t tell you how many patients have revealed their substance use only after quite a few visits and told me they simply lie on the screening forms. Why anyone trust someone who is either staring into the computer or who has a scribe in the room recording your responses?
“It’s all about APA politicos loving the group health aims of Obamacare, and trying to shoehorn the MOST individual-based specialty into a population health model. It is absolutely fatally flawed but it’s their secular religion, and that usually wins over logic.”
Dr. O’Brien, I disagree. I would suggest that politically minded individuals in APA and AACAP are focused on leveraging sources of money/power. Those were the motivations that often drove engagement with pharma that at times were to the detriment of the needs of front line psychiatrists. Those same motivations, and sometimes very same individuals, drive the kind of engagement with the ACA that is to the detriment of the needs of front line psychiatrists. The ideology of the day is in service of the money/power that can be tapped. Whether it is Faustian alliances with Pharma, Device Makers, Neutraceutical manufacturers, Neuroscience Manhattan Projects, Managed Care, ACA, whatever, they are largely facets of a similar problem. If you look at some of the central players in destructive engagement with Pharma, they are the same people now talking screening, staging, population health. At least this is true within child psychiatry.
Sorry, I also meant to add this:
“Collobo-care implies that your mental status examination is no better than any other professional in the chain. Who is comfortable with that?”
Amen
Reading that account of John J. made my skin crawl. Would anyone actually want to be treated like that? A couple of questionnaires, instant prescription of pills, rushed contacts?
The flaws in this approach are colossal. There is no real understanding of John. No one sits down to take an actual history. There is no understanding of the childhood trauma he may or may not have experienced, despite all the research from Dr. Felitti and the CDC on the huge role that childhood trauma plays in the etiology of depression. There is no discussion of the marital conflict, or how it can be resolved and the relationship saved. There is no discussion with John about his preferences for treatment, whether he thinks that therapy would be more helpful than pills, and whether he wants to meet with a couples therapist. There is certainly no information given to John that pills have multiple side-effects, are only marginally better than placebo (if at all), double the risk of developing diabetes, or any other attempt at informed consent. There is simply “What are your PHQ-9 scores, here is a pill, if you do not like it, take another one, and do some simplistic behavioral activation.”
This is not caring for John as a human being, listening to his story, and involving him in his treatment. It is taking a lump of flesh, whizzing it down the conveyor belt, where it is scanned, prodded, rescanned, stamped, and spat out the other end.
Great post Eric. On a related note, can you imagine the outcry if a surgeon operated on a patient on a non-emergency basis without talking to the patient and getting a history under a collaborative care model? But yet, it is ok to do this to people with “mental health issues.”
Disgusting!
horrorshow
“Dr. O’Brien, I disagree. I would suggest that politically minded individuals in APA and AACAP are focused on leveraging sources of money/power. Those were the motivations that often drove engagement with pharma that at times were to the detriment of the needs of front line psychiatrists. Those same motivations, and sometimes very same individuals, drive the kind of engagement with the ACA that is to the detriment of the needs of front line psychiatrists.”
They are not mutually exclusive and I think it’s both factors driving this. It’s actually a less cognitively dissonant when your distorted ideology is highly profitable a la Jon Gruber.
It’s so nice to be able to virtue signal at faculty cocktail parties without having to do with the actual fallout of failed ideas. Good intentions are all that matter.