The Dan Markingson case is one of those that asks us all to re-examine our beliefs. Such cases can be a screen on which to project our pre-existing thoughts or it can be a new page. Whichever way you take it – the true drama of his suicide, the pictures of his childhood posted on the Internet, the anguish of his mother, the struggles of his champions – all add a layer of reality to the issues often seen from a greater distance. Tueday morning, I worked in a busy clinic seeing patients, and this case was sitting on the side of my mind. I had been trying to focus on what aspect was the most compelling to me. I knew it wasn’t all the major controversies that immediately come to mind, things we could all list. Carl Elliot does a fine job of cataloging them in The Deadly Corruption of Clinical Trials. And it wasn’t the absurdities that I [and everyone else] mentioned; allowing a patient declared incompetent to suddenly become competent to sign on to a trial; putting someone whose mind was filled with the kind of thoughts listed in an earlier post [the rightest of causes…] on a blinded, fixed dose of medication; moving him to a halfway house when there’s no evidence that he was halfway anywhere; ignoring his mother’s concerns; putting him in a study measuring how long people stay on a medication when he was essentially sentenced to keep taking it; etc. Those things are obvious.
Driving home, I was thinking about the snippets that had stayed with me from reading about Dan again yesterday. One was an AstraZeneca email in Carl’s article that grabbed my attention when I first saw it [selling seroquel I: background…]:

Two plus years ago I read that in horror [now, it comes as no surprise at all]. Another thing that lingered was the clip in the video where the clinical coordinator said she "‘didn’t do anything that was wrong or against the law.’ She said Mary Weiss was very controlling. ‘You don’t just kick someone out of a study because the mother wants it to happen.’ Kenny said Dan was doing well. ‘The guy had pretty many stressors going on. Mom was very much interfering with things.’ Kenny said that the fact that Dan committed suicide near Mother’s Day ‘was a really strong message.’" And then there was this remark from the University’s Senior Director of Communication about Scientific American writer Judy Stone, "I looked her up and can’t tell if she’s a whacko or not. I get nervous about anyone who would pay attention to Carl." But this was the loudest thing, "In his deposition, Olson said he saw Dan approximately six times from the date he was admitted in November until he committed suicide in May" followed by "In late April 2004, as Dan’s stay of commitment was about to expire, Olson recommended extending it for another six months — the duration of the CAFE study. He noted that Dan still had ‘little insight into his mental disorder’ and might ‘place himself at risk of harm if he were to terminate his treatment’.’"
At the halfway house, Dan often stayed in his room for days. On March 26, 2004 nearly four months after his discharge from Fairview, his thoughts were still "delusional and grandiose," according to a social worker’s note. An occupational-therapy report from April 30 detailed Dan’s condition: "Personal appearance disheveled. Isolated and withdrawn. Poor insight and self-awareness." Entries in a personal journal that Dan kept during this period don’t show any obvious changes, suggesting that he was improving little, if at all…
There are levels of the approach to this mental illness that I thought were best conceptualized in the era of the community mental health movement in terms of prevention. Primary prevention is anything that one does to prevent the development of illness. Don’t smoke. Get immunizations. etc. In the case of psychosis, Patrick McGorry in Australia and others are attempting to identify these patients prior to a psychotic break. It’s a laudable endeavor that’s not ready for prime time. And there’s controversy [as always] about what one would do if you actually could do that. But that’s not to say that it’s not valuable research.
Secondary prevention is efforts to minimize the impact of illness once it appears. With an acute psychotic break, modern treatment involves the use of antipsychotic medication, sometimes protective custody, and psychosocial interventions with an eye always on the future. The issue of protective custody is primarily in the hands of the legal system. And while the use of medication is the subject of endless armchair debates, it’s pretty standard fare. And it’s a big part of the debate about the case at hand about Dan Markingson.
Tertiary prevention focuses on prevention of recurrence and the prevention of deterioration. When people with psychosis have either a course including recurrent psychotic illness or persistent signs of illness, should they stay on medication all the time, intermittently, not at all? Big controversies, and a factor in the debate are the side effects and potential irreversible long term effects of the drugs. That’s why we were all so hopeful when the atypical antipsychotics appeared: prevention of recurrence? prevention of deterioration? With no down side? That was not to be. And we knew that by the time Dan’s illness came along. So did AstraZeneca – about their own drug Seroquel. They knew it from their own Study 15 that they had already buried:
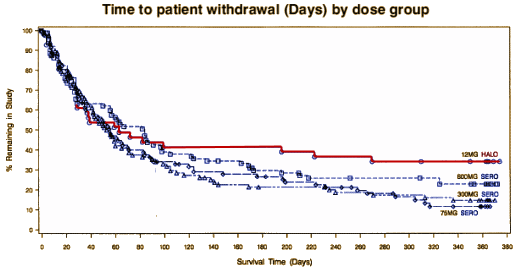
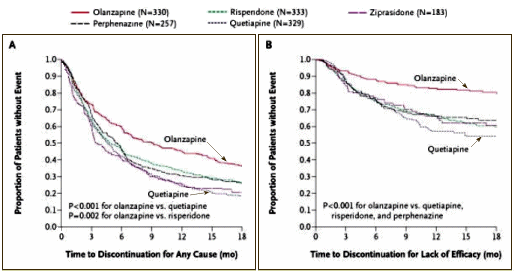
Clearly, the patients preferred Haldol over Seroquel. It’s clear as a bell. And AstraZeneca knew CATIE was coming and they weren’t going to look good…
At the halfway house, Dan often stayed in his room for days. On March 26, 2004 nearly four months after his discharge from Fairview, his thoughts were still "delusional and grandiose," according to a social worker’s note. An occupational-therapy report from April 30 detailed Dan’s condition: "Personal appearance disheveled. Isolated and withdrawn. Poor insight and self-awareness."
"In late April 2004" … "He noted that Dan still had ‘little insight into his mental disorder’ and might ‘place himself at risk of harm if he were to terminate his treatment’."
-
The CAFE Study was driven by commercial interests rather than to gain medical knowledge.
-
It was a maintenance study for patients who had responded to medications. Dan had been admitted several days before with a florid psychosis of several months’ duration. There is no evidence that he responded to treatment. There was nothing "maintenance" about his case.
-
He was a success story for the trial because he hadn’t stopped the medication. That was a complete sham, because he couldn’t stop the medication under threat of commitment.
-
His clinical condition certainly didn’t improve over the ensuing six months. If anything, he was deteriorating.
Psychiatrists and psychiatry take a lot of hits from a lot of places – some deserved, some not so deserved. But the bottom line if you are a psychiatrist is that you become genuinely engaged with the case at hand and you bring everything possible to bear to see that the patient has the best shot at the best recovery that can be achieved, even in the face of persisting disability. This case didn’t even come close to that standard. Dan was pretty disturbed and his recovery was anything but guaranteed, but the care he got didn’t approximate his best shot – not even a good shot. He spent 6 moths languishing in a halfway house on a weak-sister medication that was having, at best, a sub-optimal effect. And he succumbed to a violent psychotic suicide in plain view, a testimony to the inadequacy of the treatment. Such things can happen in the best of circumstances, but this was the nowhere close to the best of circumstances – a patient under care who was neglected.
The term burn-out has become part of our daily conversational lingo. It means that a person who has been doing a difficult job has lost whatever extra drive it takes to keep them at the task. The term actually originated in describing the people who work with chronic psychotic patients. It’s hard work, to say the least, and the rewards are intangible – preventing deterioration, sticking with people through relapses, disillusionment with outcomes. When burnout comes, you can feel it, and the right thing to do is move on. You gave what you had until you couldn’t do it anymore. Good for you. Now go do something else. The alternative is to stay around and develop a kind of hardened indifference you can spot from twenty yards. Most people reading this who are in a mental health field know exactly what I’m talking about from seeing it, and perhaps even living it. But some people are able to keep going without ever burning out. They are amazing – the real saints among us, in my humble opinion.
Was the half-way house dedicated to the study or was it just your average half-way house stocked with ex-cons, sociopaths, addicts, and child sexual abusers, and thieves? I lived in a half-way house on my savings until I got a job in this city. With all my mental faculties intact, I had to stay on my toes and one of my scrips was still ripped off. It’s not a good environment for vulnerable people who can’t care for themselves.
We have enough evidence to indicate that many factors influence the outcomes of what you describe as primary, secondary and tertiary prevention. There are the obvious, such as having meaningful relationships, family support, housing, , as well as the less obvious: whether past trauma is acknowledged and worked through, access to psychotherapy, the opportunity to have a meaningful role in society, hope for a better future and being able to fit one’s belief system into something acceptable to society (various spiritual belief-systems for example)
Having said that, what that strikes me about this tragedy is that it once again highlights how a focus on solely biological factors (which are after all the major sources of profit) leads research to largely ignore the other factors altogether. As you say, Dan’s well being as an individual, his fundamental needs as a person, were almost entirely ignored, because the sole factor of interest was drug compliance 9or whatever the term of choice is these days.
I’ve just returned from the international Hearing Voices Congress, where over 700 peers, survivors, mental health workers, psychiatrists and neuroscience researchers met to discuss how these factors can be considered TOGETHER, so that the best outcomes can be achieved without losing sight of the sufferer as an individual.
I was inspired to see talks hosted, chaired and organised by capable, articulate and charming people who – despite experiencing great distress and recieving traumatic and inhuman psychiatric treatment – had found various ways to overcome their problems and lead rich and rewarding lives.
So here’s to an acknowledgment of the multi-faceted nature of human flourishing. There is no better antidote to the cyclopean view that is being foisted on us by pharmaceutical companies for their own benefit, but not the benefit of their patients.
Wiley- In response to your question regarding the type of facility Dan was living in, the answer is it’s called a Rule36 group home here in Minnesota. And the Rule 36 is suppose to designate it as a dual MI and CD facility. When Dan Markingson was hospitalized his mother requested that a CD assessment be done by the hospital. It was, and it was recommended that he also receive CD therapy as well as treatment for his mental psychosis. However, Dan never received any CD therapy as his treating psychiatrist ignored the evaluation as he feared it would have interfered with his participation in the drug study. Just another set of eyes or ears that might have questioned Dan’s ability to participate. Same thing with Dan’s “day treatment,” he was scheduled to participate in a county program run through a very good private center just minutes from where he lived at the group home. His psychiatrist changed all that as soon as he became aware of it, and had Dan travel 15 miles to the University’s program that he oversaw. Ethics? There were/are no ethics anywhere with the U-MN.
Thanks for this series on this important case. In your first blog, you alluded to the controversy stirred up when we venture into the fraught area of involuntary treatment. This is clearly the most challenging topic for me. I have tried to address this openly.
http://www.madinamerica.com/2012/05/coercion/
If I do the thought experiment of considering that I am psychotic in the way Dan Markinson. If I am under the care of Dr. Nardo, I am comfortable with some forms of involuntary treatment. But when I think about being under the care of any random psychiatrist who happened to be on call that fateful day, I am chilled.