|
NOTE: I have a Conflict of Interest about this report. It’s from the NIMH funded RAISE Study [Recovery After an Initial Schizophrenia Episode]. My conflict is that I have two interests. First, I’m really interested in this particular study on the impact of psychosocial treatment on these First Episode Patients. But second, I’m exhausted with academic researchers with extensive industry connections – suspicious of almost everything they publish. John Kane is such a person. Here are a few comments about his extensive industry connections – prelapse: but there’s more…. I was particularly put off by his comments about COI in an interview here. He is the Principle Investigator for this NIMH RAISE study…
|
In spite of the persistent divisive rhetoric, there seems to be a developing consensus about the treatment of psychotic mental illness [schizophrenia]. The notion that the only treatment is antipsychotic medication "for life" has been laid to rest [largely through the efforts of Robert Whitaker and his colleagues at Mad in America]. Most agree that the medication is indicated for acute psychosis, but controversy persists about maintenance [in general, independent of the advice given, the patients themselves don’t continue to take it long term]. There’s a developing consensus that ongoing care for these patients from a mental health system or provider is essential, over and beyond the issue of medication. The form of that ongoing care is unclear, and the subject of heated debate. Most hope for some way to identify these patients before a psychotic break [but worry that it will lead to overmedication]. There is a concern, mainly in the lay population, that these patients are dangerous. Likewise, there is a concern almost everywhere that chronic psychotic patients are inappropriately housed in jails and prisons. With that as an introduction, yesterday we read this in the New York Times:
New York Timesby BENEDICT CAREYOCT. 20, 2015More than two million people in the United States have a diagnosis of schizophrenia, and the treatment for most of them mainly involves strong doses of antipsychotic drugs that blunt hallucinations and delusions but can come with unbearable side effects, like severe weight gain or debilitating tremors.
Now, results of a landmark government-funded study call that approach into question. The findings, from by far the most rigorous trial to date conducted in the United States, concluded that schizophrenia patients who received smaller doses of antipsychotic medication and a bigger emphasis on one-on-one talk therapy and family support made greater strides in recovery over the first two years of treatment than patients who got the usual drug-focused care.
The report, to be published on Tuesday in The American Journal of Psychiatry and funded by the National Institute of Mental Health, comes as Congress debates mental health reform and as interest in the effectiveness of treatments grows amid a debate over the possible role of mental illness in mass shootings…
2-Year Outcomes From the NIMH RAISE Early Treatment Programby John M. Kane, M.D., Delbert G. Robinson, M.D., Nina R. Schooler, Ph.D., Kim T. Mueser, Ph.D., David L. Penn, Ph.D., Robert A. Rosenheck, M.D., Jean Addington, Ph.D., Mary F. Brunette, M.D., Christoph U. Correll, M.D., Sue E. Estroff, Ph.D., Patricia Marcy, B.S.N., James Robinson, M.Ed., Piper S. Meyer-Kalos, Ph.D., L.P., Jennifer D. Gottlieb, Ph.D., Shirley M. Glynn, Ph.D., David W. Lynde, M.S.W., Ronny Pipes, M.A., L.P.C.-S., Benji T. Kurian, M.D., M.P.H., Alexander L. Miller, M.D., Susan T. Azrin, Ph.D., Amy B. Goldstein, Ph.D., Joanne B. Severe, M.S., Haiqun Lin, M.D., Ph.D., Kyaw J. Sint, M.P.H., Majnu John, Ph.D., and Robert K. Heinssen, Ph.D., A.B.P.P.American Journal of Psychiatry. Published on-line Oct 20, 2015.Clinical Trial: NCT01321177
Objective: The primary aim of this study was to compare the impact of NAVIGATE, a comprehensive, multidisciplinary, team-based treatment approach for first-episode psychosis designed for implementation in the U.S. health care system, with community care on quality of life.Method: Thirty-four clinics in 21 states were randomly assigned to NAVIGATE or community care. Diagnosis, duration of untreated psychosis, and clinical outcomes were assessed via live, two-way video by remote, centralized raters masked to study design and treatment. Participants [mean age, 23] with schizophrenia and related disorders and ≤6 months of antipsychotic treatment [N=404] were enrolled and followed for ≥2 years. The primary outcome was the total score of the Heinrichs-Carpenter Quality of Life Scale, a measure that includes sense of purpose, motivation, emotional and social interactions, role functioning, and engagement in regular activities.Results: The 223 recipients of NAVIGATE remained in treatment longer, experienced greater improvement in quality of life and psychopathology, and experienced greater involvement in work and school compared with 181 participants in community care. The median duration of untreated psychosis was 74 weeks. NAVIGATE participants with duration of untreated psychosis of <74 weeks had greater improvement in quality of life and psychopathology compared with those with longer duration of untreated psychosis and those in community care. Rates of hospitalization were relatively low compared with other first-episode psychosis clinical trials and did not differ between groups.Conclusions: Comprehensive care for first-episode psychosis can be implemented in U.S. community clinics and improves functional and clinical outcomes. Effects are more pronounced for those with shorter duration of untreated psychosis.
background, rationale, and study design.by Kane JM, Schooler NR, Marcy P, Correll CU, Brunette MF, Mueser KT, Rosenheck RA, Addington J, Estroff SE, Robinson J, Penn DL, and Robinson DG.Journal of Clinical Psychiatry. 2015 76[3]:240-246.
OBJECTIVE: The premise of the National Institute of Mental Health Recovery After an Initial Schizophrenia Episode Early Treatment Program [RAISE-ETP] is to combine state-of-the-art pharmacologic and psychosocial treatments delivered by a well-trained, multidisciplinary team in order to significantly improve the functional outcome and quality of life for first-episode psychosis patients. The study is being conducted in non-academic [ie, real-world] treatment settings, using primarily extant reimbursement mechanisms…
So why the long introduction? It’s because when I looked at Dr. Kane et al’s paper, I could find little relationship to the AJP paper and Benedict Carey’s New York Times article [or for that matter, any of the other media reports]. Carey had reported lower antipsychotic doses, but the paper says nothing about medications. Cary’s article mentioned one-to-one talk therapy but I found not much about that in this report. What I did find first off were graphs of the answers to quality assurance questionnaires:
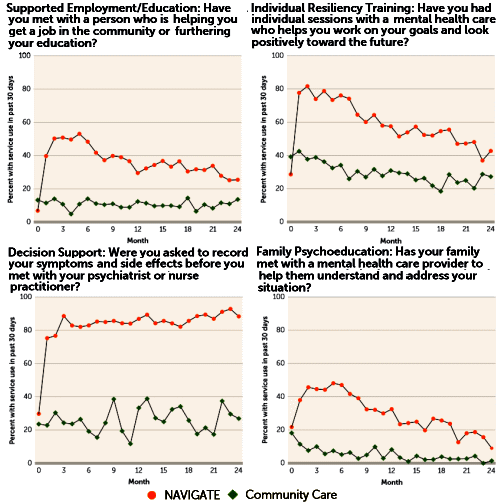
And then there was this showing some modest improvements in the NAVIGATE group [though the metrics seem odd and fairly distant from the data – statistical testing of only the treatment×time interaction???]:
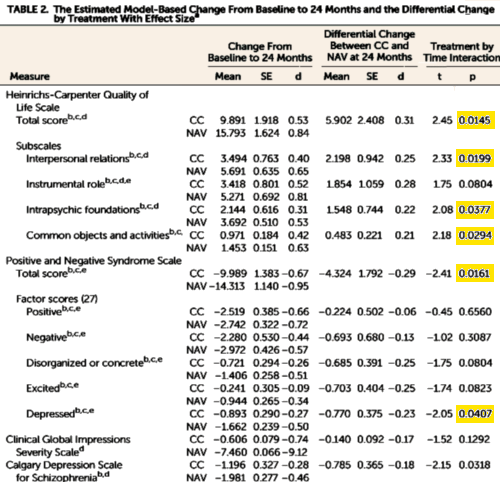
This issue of the Journal includes a report on the primary outcomes from the Recovery After an Initial Schizophrenia Episode [RAISE] Early Treatment Program clinical trial. …RAISE was not a test of a breakthrough intervention or high-tech diagnostic but a trial of adapting and optimizing currently known, evidence-based practices. The RAISE question was simple and urgent: Will a comprehensive, person-centered, team-based approach for first-episode psychosis improve outcomes? For RAISE, the outcomes measured were quality of life, participation in school or work, and symptomatic improvement. The setting was “ real world ”— 34 community mental health centers in 21 states.This issue of the The study compared the efficacy of an experimental intervention, called NAVIGATE, with standard community care for people with first-episode psychosis. NAVIGATE consisted of four evidence-based interventions: personalized medication management, family psychoeducation, resilience-focused individual therapy, and supported employment and education. The component interventions were offered as a package, with the addition of a team leader who coordinated services and served as a primary point of contact for individuals and their families. The NAVIGATE programs also involved a proactive focus on engagement. In contrast to standard community care, these multiple components were offered within a shared decision-making framework and implemented according to patient preference.
Just as the dramatic improvements for treatment of acute lymphoblastic leukemia reflected incremental gains over time, the results for NAVIGATE take a palpable step toward markedly better outcomes for young people following first-episode psychosis. A measure of quality of life improved modestly more in the NAVIGATE group than in the standard community care group over 24 months [effect size = 0.31], and the NAVIGATE group had lower levels of symptoms as measured by the Positive and Negative Syndrome Scale [effect size = 0.29]. Participants in the NAVIGATE group stayed in treatment longer than the standard community care group [a median of 23 months compared with a median of 17 months]. In contrast to some earlier studies of first- episode psychosis , the intervention did not decrease hospitalization probably because the rates of hospitalization were relatively low in both groups [over the 2 years of treatment, 34% of the NAVIGATE group and 37% of the standard community care group were hospitalized for psychiatric indications].
One of the most remarkable aspects of this study was the substantial moderation of the treatment effect by the duration of untreated psychosis. The median duration of untreated psychosis in the entire sample was 74 weeks — a clear indication of the need to identify young people with mental illness at much earlier stages and to get them into effective treatment more rapidly. Those with a duration of untreated psychosis of less than the median of 74 weeks responded far better to the NAVIGATE intervention than those with a longer duration of untreated psychosis at baseline. Indeed, the overall effects of NAVIGATE were largely driven by the robust response [the effect size was 0.54 for the quality of life measure and was 0.42 for overall symptoms] from those with shorter duration of untreated psychosis. These results demonstrate the importance of early detection, early engagement, and integrated care following the onset of psychosis…
VICE NEWSBy Colleen CurryOct 21, 2015A landmark study into the treatment of newly diagnosed schizophrenics has found that talk therapy combined with medication can be more effective in treating symptoms than just strong doses of drugs. The findings, which emphasize the success of therapy and how unusual it is for schizophrenics to be treated with it, could help shift the way health insurers in the United States cover mental health treatment costs.
Researchers spent four years studying more than 200 newly diagnosed schizophrenics. Half of the subjects were treated solely with medication, while the other half received a lower-dose medication combined with individual therapy, coaching sessions in the workplace or school, and family counseling.
The study involved patients at 34 treatment centers in 21 states. The results, released Tuesday in the American Journal of Psychiatry, found that individuals in the early stages of schizophrenia were better off receiving lower-doses of antipsychotics in conjunction with therapy. The National Alliance of Mental Illness (NAMI) praised the study and said it would be used as part of the organization’s push to broaden access to services for the mentally ill…
The study’s release coincided with hearings on Capitol Hill for mental reform amid a bipartisan push to improve mental health treatment, partially due to the increase in mass shootings in which mental illness is thought to have played a role.
Washington PostBy Lenny BernsteinOctober 20, 2015Quickly identifying people who have suffered a first schizophrenic episode and treating them with coordinated, sustained services sharply boosts their chances of leading productive lives, according to a major study being published Tuesday. And the treatment can be provided in a typical community mental health setting, the researchers concluded…
The study, called Recovery After an Initial Schizophrenia Episode (RAISE), found that people who are provided years of “coordinated specialty care” in community clinics had a greater quality of life, more involvement in work and school, and less ongoing pathology than others who received typical care.
Although this approach is more expensive and labor-intensive, the researchers suggest that it may be cost-effective in the long run. The approach includes psychotherapy, medication, supported employment and education, help for families of the mentally ill person, and case management. Much of the effort can be funded under insurance and government reimbursement policies, the researchers note.
The study confirms previous research results that the most critical element of treatment may be starting it as quickly as possible after a first psychotic episode. It found “a substantial difference” in effect for patients who began treatment less than 74 weeks after their first symptoms — the median length of time that people in the study went untreated after the onset of psychosis.
“Doing the right thing — and doing the right thing at the right time — that’s the key finding,” said Robert Heinssen, director of the division of services and intervention research at the National Institute of Mental Health, which funded the $25 million, six-year study. “That is guiding our efforts going forward. That has become the north star of where we’re going”…
Cost remains a challenge, because some of the services offered by the comprehensive care model are not reimbursed under traditional fee-for-service arrangements, Kane and his colleagues said. Last week, though, three federal agencies issued guidance to help states design benefit packages for treatment of first-episode psychosis using Medicaid and mental health block-grant funds.
In sum: Patients with schizophrenia do better if they get comprehensive services, and they do better if they are treated early in the course of their illness. And now we officially know what we all knew.
But after reading and reading, I’m afraid my reaction is a bit more critical than that. I suspect that the published paper casts the study is the best possible light [or better], and that the untouched data is less glowing. The NIMH track record with naturalistic studies isn’t so hot [as in STAR*D]. And from what I’ve highlighted above, it’s obvious that this paper in linked to a campaign for more mental health funding [which is more than fine by me]. So to the dilemma. I support the conclusions and their implications, but am suspicious that a closer look at RAISE would raise lots of questions. Like I said at the outset…
|
NOTE: I have a Conflict of Interest about this report….
|
Mad in Americaby by Justin KarterOctober 21, 2015NIMH: Director’s Blogby By Thomas InselOctober 20, 2015NIH: Director’s Blogby Dr. Francis CollinsOctober 20, 2015
They certainly try to put the best face on their results through selective reporting and selective analyses. They give dimensional change measures (Table 2 that you reproduced above) but they do not present analyses for the main outcome measures at endpoint. It is clear from Figure 2 that there is no significant difference between groups in the primary outcome measure or in the PANSS total scores at 6, 12, 18 or 24 months. Overall, on inspecting Figure 2 one has to consider possible regression to the mean. In addition, the authors do not state the usual categorical response measures that one finds in, say, the Wunderink reports. They also do not state the 2-year relapse rates or the differential drug dosing information, as you pointed out.
They also seem to finesse the issue of duration of untreated psychosis (DUP). It seems probable from Figure 3 that there was no difference between groups in the slope of improvement over time on the primary outcome measure for those with DUP greater than the median of 74 weeks, but that information is not clearly stated in the Abstract. I think you are correct to see an agenda at work here.
Thanks for validating my paranoia, guys.
I love to see the eagerness with which the news of this study has been embraced. People are starving for some sort of approach to “psychiatric illness” (whatever that may be) that is marginally human, and that might take an interest in the prospect of a life worth living. However, I don’t trust the study itself, and want to see the details.
My biggest question: If John Kane is so sold on the prospects for less physically and mentally damaging “chemotherapy” and more communication, then why has he signed on to direct the PRELAPSE Study for Otsuka? That study will randomly select several hundred young people going through a first psychotic episode and assign them to monthly (fairly high dose) depot injections of Abilify for TWO YEARS. The two studies would appear to lead in exactly opposite directions. And anyone who believes the sales pitch for the RAISE study should be horrified by the PRELAPSE study, it seems to me.
What gives, Doctor Kane?
A further thought – this report reads more like a demonstration project in health services research than a study in experimental therapeutics. From that perspective, to accentuate the positive serves the goal of increased funding. But, spin is still spin, and spending more dollars on interventions for which the evidence is marginal does not serve patients in the long run.
It’s too bad they couldn’t do an Open Dialogue Approach where the client has a choice about whether or not to take neuroleptics, and the families are engaged in a dialogue that discusses symptoms but without attributing them explicitly to a disease process / brain illness. But I guess in the United States, with drug companies are the masters of the psychiatrists who run this study, such a leap is impossible at present, considering that positive results from a no-medication non-disease model approach would threaten billions of dollars in profit.
I think this RAISE study does have some positive elements. They only gave people a relatively limited amount of social support (this wasn’t intensive psychotherapy), and reduced medication a moderate amount, and even these changes resulted in somewhat of a positive trend. So it suggests that further research should be done with lower or no medication, and with increased, possibly longer psychotherapy or family support.
As Mickey said, the trends of more therapy and less drugs helping shown in this study are pretty obvious and not really news, except to uninformed lowpeople.
Edward, anything constructive in your comment above is undermined by this: “But I guess in the United States, with drug companies are the masters of the psychiatrists who run this study, such a leap is impossible at present, considering that positive results from a no-medication non-disease model approach would threaten billions of dollars in profit.” It’s tedious, it’s repetitive, and it’s tendentious. Help yourself – drop the dripping sarcasm.
Bernard,
I wasn’t addressing my comment to you, but can understand why an old retired psychiatrist might not like it. And many people I know would find quite a bit of truth in the idea that drug companies dominate and distort psychiatric research in the USA, and that non-medical model approaches would threaten their income.
I find some of your comments offputting, but I don’t call you out on them anymore; I just ignore them or find the humor in them. This is the internet, and you’re entitled to your opinion.
And I’m not going to change how I am… Deal with it.