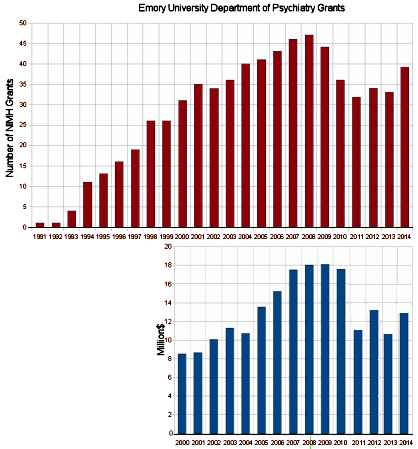
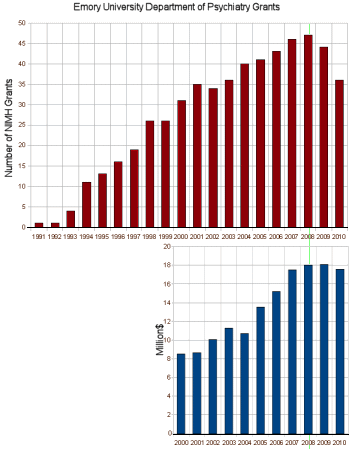
September 27, 2010I’ve spent no small amount of time raling about the invasion of the Pharmaceutical Industry into Academic Medicine, specifically at Emory University where I trained and worked for some time. The Chairman, Dr. Charles Nemeroff, was relieved of his Chair in 2008 because of repeated Conflict of Interest violations. Since then, he has moved on to become the Chairman at the Miller School of Medicine in Miami. You might wonder why Miami would recruit a tarnished person, or why Emory put up with his antics so long. That question has an answer. Dr. Nemeroff came to Emory in 1991. At that time, the Department at Emory had no National Institute of Mental Health Grants. In the NIH/NIMH database, the funding amounts for grants only goes back 10 years, so I’ve shown the total number of grants above for the whole period and added the total funding below for the last decade:
Dr. Nemeroff came in 1991, and stepped down under a cloud of allegations in the Fall of 2008. By that year, the Department was bringing in 18 Million Dollars yearly from NIMH Grants [up from zero when he came]. And that only includes NIMH Government Grants. While I have no access to the amounts, there was also plenty of Pharmaceutical Industry money coming Emory’s way as well during those years through Dr. Nemeroff’s efforts.
Unless you’ve been in Academic Medicine, you would have no way of knowing how medical education actually works. There is very little Institutional Support from the Universities. Much of the teaching is done by volunteer clinicians [unpaid]. In most medical specialties, the departments support themselves by delivering services – hospitals, clinics, etc. In psychiatry, we just don’t generate money like the rest of medicine – don’t even come close. In the 1950s and particularly 1960s, there was heavy government funding to support the Community Mental Health services flowering at the time. So departments of psychiatry were heavily invested in and supported by public medicine. In the 1970s, those resources were waning fast, and with Reagan’s election in 1980, they virtually disappeared. Managed Care was slashing psychiatric services at the same time [also a resource for psychiatry departments]. Those were my days in academic medicine, and we were operating hand to mouth [on our best days].
Is it a Darwin 101 problem or is it rather a matter of perverse incentives? When I was a department chair I liked to remind the faculty that it was their department, not mine, and that quality mattered. More than once I dissuaded faculty members from pursuing easy money from NIMH, because it came with unwelcome strings attached and it would have distracted them from their more serious purposes. It would also have compromised their independence as clinical scientists. Among all those Emory grants you charted were out and out boondoggles that contributed nothing incisive to the advancement of clinical science.
If you’d like to check out what Dr. Carroll is talking about, go to the NIH RePORTER and fill out these three fields on the Query Form there:
Put emory in Organization. Put psychiatry in Department. Select either all or a specific year in Fiscal Year (FY): Then select SUBMIT QUERY. On the results page click FY in the header to sort by year [toggles ascending and descending]. Then checkout other universities. Watch out for the RePORTER. Once you figure out how to use it, it can become addicting…
Hi,
This is not a political comment on this particular post. I have been following your blog for a while now, I always study your posts and think of them and take them in, to the best of my understanding. I do not have any medical training.
I have recently reinstated neuroleptic drugs for extreme protracted withdrawal syndrome. To put it simply. I did this at the advise of friends on survivingantidepressants.org.
It seems to me you are someone who has extensive knowledge of neuroleptic drugs. My plan is to with draw extremely slowly. The problem I have is that one of the drugs I need to withdraw from in Seroquel. This is a very expensive drug and I am currently unable to work. I can go onto state but they do not supply Seroquel, but rather a generic. I am not sure which generic at this stage, they will let me know soon.
My psychiatrist does not really believe in withdrawals, but he has been willing to listen. He suggested Truvalin as a substitute. I was wondering if perhaps you could help me see if that really is the same drug, etc, or if there are any other generics, or perhaps if you could point me in the direction of someone who could help me with this.
I am extremely sensitive to any changes at this point, taking it one day at a time.
I thank you deeply for reading my message and hope to hear from you soon. I also thank you for your blog and for trying to get the message out there about these neuroleptics and their effects, as well as the deeply rooted problems with our society and medical health paradigm.
Wishing you warm regards,
TJ
Whilel I find your Darwinian analogy interesting, I think this situation is more so the insidious nature that corruption and narcissism / anti social agenda does to decay the prior healthy boundaries that academic medicine should maintain.
Once again, posts like this just reinforce to me that profit and care are completely incongruent. also, more and more academic leadership is so tainted and misguided at the very least, it’s only a matter of time before people should be held to felony charges.
dear TJ,
i’m not a doctor and i would recommend that you very very very very VERY VERY VERY VERY (i cannot say this enough times) carefully analyze ANYTHING someone tells you, whether it is on this site or not.
one thing i will mention, aside from my reservations regarding the initial argument for putting you on medication (i’m not convinced this ‘syndrome’ you’ve been diagnosed with is legitimate), i recommend that you ‘taper off’ any drugs you feel uncomfortable with.
tapering off means you continue your regular dosage, and then begin to incrementally-decrease it over the ensuing weeks. if you’re taking two capsules, for example, you’d start taking one for a week (maybe even two if you’ve taken them a while).
you may need your doctor to prescribe different dosages to ensure that you’re not going from one large capsule to nothing, as this can have some adverse effects.
for any neurological drug, i cannot stress enough how important the SLOW and PROGRESSIVE reduction of the dosage is key to reducign symptoms.
whether you should be even taking seroquel for this alleged extreme protracted withdrawal syndrome is another topic i’ll leave to the accredited psychiatrists here (i’m not even in medical school, go figure).
I wonder if Dr Carroll has a typo in his comment. NIMH money has never been easy and does not come with strings attached and it is inconceivable to me that a department chairman would ever dissuade a faculty member from applying for NIMH funding. My understanding from talking to people who were in the department at Duke during Dr Carroll’s well regarded term as chair and director of the clinical research center was that there was a very strong emphasis on obtaining NIMH funding. PHARMA money is a different story and that money back in the SSRI era was relatively easy and did come with strings attached.
If neuroscience and biopharma uber alles has become 90% of psychiatric residency because of the influence of NIHM and pharma, you have to wonder if there are better alternatives with the objective of getting a comprehensive eduction in psychiatry. Like maybe doing a flex internship (so you can prescribe) then getting a Ph.D. in quant psychology or whatever you’re interested in. It’s not so far fetched. Consider where most analysts come from today vs. in 1960.
I’ve commented elsewhere that I’d much rather hear a discussion between two older psychoanalysts over whether a short term improvement is due to transference cure vs. flight into health vs. a tedious Powerpoint lecture explaining why the latest me too drug is better than all the rest. Even when the analysts are wrong, they’re more interesting and more unpredictable.
Hi, Dr. Garlow… no, there was no typo. Certain kinds of NIMH funding were easy to obtain if faculty members were willing to sign on to low-quality top-down mega-projects conceived and micro-managed by NIMH staff. But the money would have come with the consequences I mentioned above. Several faculty members were courted by NIMH staffers to join up and they struggled with this kind of decision until I told them to follow their own, independent scientific instincts.
correct dr carroll,
it’s high in number but extremely dismal on facilitating the scientific content and/or discovery.
and they spend so much money on beaurocracy that you’re left with peanuts.
to what dr garlow was saying:
i agree that in *theory* the NIMH funding should be the most premium funding.currently however, the way it is being used is not. not only is this area difficult, but it requires an appreciation for solving the problem.
isn’t that the way it should be though? problem is, someone is straight eatin’ funding that probably belongs to a more deserving psychiatrist. this is a big issue.
this malaise is the reason (imo) the field of neurology and psychiatry both lack the direction.
we live in a world of medical overspecialization to support the beaurocracy dr carroll spoke of.
eventually this crony pyramid reveals who’s really taking the funding. that, i’ll let you guys figure out.
seems like it’s the same people every time. and why not? ‘what are you going to do about it?’ 😉
gagan sidhu, thank you for reinforcing the need for gradual tapering in response to TJ’s question.
However, many patients find a decrease of 50% (one capsule a day rather than two) is far too precipitous. Sandy Steingard has found that, when it comes to neuroleptics, a decrease of 25% every few months is tolerable, but she still finds some individuals cannot tolerate that steep of a decrease.
Because as peer support we cannot provide any kind of drug safety net, survivingantidepressants.org advises a very conservative taper of 10% per month, see http://survivingantidepressants.org/index.php?/topic/1024-why-taper-by-10-of-my-dosage/ to incur the least risk of withdrawal syndrome for the most people.
Individuals may still suffer withdrawal syndrome when other, even similar, drugs are substituted; cross-tapering is preferable to cold switches for drug changes.