There is so much divisiveness in discussions of matters that have to do with Mental Health and Mental Illness that it’s sometimes difficult to separate the wheat from the chaff. There’s a strong backlash to the medicalization of psychiatry, the heavy use of medications, the DSM-III etc. diagnostic system, and the claim/implication that all mental illness has some biological basis. On the other side there are claims that psychological counseling focusing on trauma and recovery will clear up most problems now called mental illness. It’s kind of hard to find much to read that doesn’t have some sort of rhetorical bias, visible in the first several paragraphs.
Back in my days on the wards as the de-Institutionalization of mental hospitals was winding down, it would’ve been pretty hard for anyone to maintain a belief that things were going very smoothly. Our admission units were full of people, many psychotic, and hospital beds were evaporating like a sno-cone dropped on hot pavement. At seminars and meetings, the topic was often punctuated by the Szasz meme of that day about the Myth of Mental Illness, and then back to work at the Grady Hospital Emergency room where things didn’t feel a bit mythical at all. Nobody I knew wanted to re-open any huge mental hospitals again. We just wanted short term beds to stabilize patients, and that didn’t mean just medicate, it meant trying to find a source of food and shelter that worked – a social placement, a life. The flow and the dwindling resources worked against that goal, resulting in the revolving door hospitalizations, very high rates of recidivism, and homeless people on the streets and sleeping under the bridges. The back-up promised by the Community Mental Health Movement seemed to be disappearing. The police that had to deal with these patients were fed up and vocal about it when they brought someone in for the second time in a week because the last hospitalization was so brief.
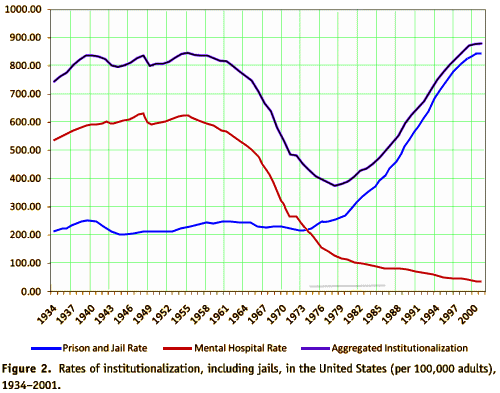
by Prins SJCommunity Mental Health Journal. 2011 47[6]:716-722.
Abstract: Although there is broad consensus that people with serious mental illnesses [SMI] are overrepresented in correctional settings, there is less agreement about the policy trends that may have created this situation. Some researchers and policymakers posit a direct link between deinstitutionalization and increased rates of SMI in jails and prisons, a phenomenon described as transinstitutionalization. Others offer evidence that challenges this hypothesis and suggest that it may be a reductionist explanation. This paper reviews claims from both sides of the debate, and concludes that merely increasing access to state psychiatric hospital beds would likely not reduce the number of people with SMI in jails and prisons. A more nuanced approach is recommended for explaining why people with SMI become involved in the criminal justice system and why developing effective strategies to divert them out of jails and prisons and into community-based treatment is needed to improve both their mental health and criminal justice outcomes.
Discussion In the debate summarized above, proponents of the transinstitutionalization hypothesis may be mistakenly drawing a causal connection between two merely correlated trends: the decline in availability of state psychiatric hospital beds and the rise in prevalence of SMI in jails and prisons. More specifically, they may [a] misinterpret deinstitutionalization as a flood of individuals who were released from state psychiatric hospitals only to be arrested and incarcerated, [b] conflate evidence that people released from psychiatric hospitals often require re-hospitalization with evidence that jails and prisons are serving that function [c] erroneously assume that people who require inpatient services are clinically and demographically similar to people with SMI who wind up in jails and prisons and [d] underestimate the effectiveness of high quality community-based treatment. The evidence against the transinstitutionalization hypothesis is compelling because [a] most people released from state psychiatric hospitals do not appear to end up incarcerated, [b] the characteristics of people with SMI in jails and prisons differ from both the characteristics of people who were deinstitutionalized and the past decades’ increasingly forensic state psychiatric hospital population, and [c] many agree that community-based treatment works for the majority of people with SMI.This is not to say, however, that conclusive evidence currently exists on either side of the debate. More rigorous analysis to clearly define the causal relationship between deinstitutionalization and the overrepresentation of people with SMI in jails and prisons is certainly warranted [for example, retrospectively matching archival inpatient, arrest, and incarceration records]. The arguments presented above should also not imply that the cases for and against increased access to inpatient services are irreconcilable. Indeed, the most important takeaway from this debate may be a fact that is often overlooked by policymakers working to address this issue: people with mental illnesses are not a homogenous population. Increased access to acute and intermediate psychiatric beds may, in fact, be necessary for a small but high-risk, high-cost group of people with severe mental illnesses who cycle through emergency rooms and the criminal justice system without obtaining the treatment they need [Pasic et al. 2005 ]. For these individuals, shortages of 24-hour hospital care [and for this group and others with SMI, affordable housing more broadly] are indeed a problem.
Nevertheless, increased access to inpatient services may not be an optimal focus for a multi-systemic criminal justice/mental health policy strategy. The ramifications of casting too wide an inpatient net would not only be expensive, but would move away from the goal of full community integration of people with mental illnesses that is the hallmark of the rights and recovery movement [New Freedom Commission on Mental Health 2003 ]. Pragmatically, it might be argued, that reinstitutionalizing people with SMI who become involved in the criminal justice system is the lesser of evils, since treatment conditions in psychiatric hospitals are bound to be better than those in jails and prisons. This reasoning, however, addresses one problem by creating a new [but familiar] one, and avoids tackling the issues at the heart of the matter.
Broadly speaking, the popular account of current mental health policy is correct: people with SMI are being ‘‘locked up’’ in jails and prisons as was the case 200 years ago. Understanding why this is happening, however, is important for developing strategies to appropriately divert people with SMI out of jails and prisons and into the treatment they need to become productive members of their communities. The history of deinstitutionalization provides an intuitive but reductionist narrative about the reasons why people with SMI are overrepresented in correctional settings. At the very least, policymakers and researchers should treat the transinstitutionalization hypothesis with caution and not as a presupposition. Failure to approach this issue with the nuance it requires may unwittingly imply expen- sive interventions that will benefit only a fraction of the population at issue. For the large remainder of people with SMI in jails and prisons, other causes of their involvement with the criminal justice system should not be ignored. In this regard, shifts in philosophy and ideology behind the concept of deinstitutionalization are still relevant. For the majority of this group, the key to staying out of hospitals, jails, and prisons may be a place to live, a job or some income support, a meaningful relationship or social network, quality healthcare, or linkage to treatment instead of frequent arrest for substance use disorders — fundamental needs that can best be redressed in the community, not psychiatric or correctional institutions.
by Seth J. Prins, M.P.H.Psychiatric Services. 2014 65:862-872.
Objective: People with mental illnesses are understood to be over-represented in the U.S. criminal justice system, and accurate prevalence estimates in corrections settings are crucial for planning and implementing preventive and diversionary policies and programs. Despite consistent scholarly attention to mental illness in corrections facilities, only two federal self-report surveys are typically cited, and they may not represent the extent of relevant data. This systematic review was conducted to develop a broader picture of mental illness prevalence in U.S. state prisons and to identify methodological challenges to obtaining accurate and consistent estimates.Methods: MEDLINE, PsycINFO, the National Criminal Justice Reference Service, Social Services Abstracts, Social Work Abstracts, and Sociological Abstracts were searched. Studies were included if they were published between 1989 and 2013, focused on U.S. state prisons, reported prevalence of diagnoses and symptoms of DSM axis I disorders, and identified screening and assessment strategies.Conclusions: Definitions of mental illnesses, sampling strategies, and case ascertainment strategies likely contributed to inconsistency in findings. Other reasons for study heterogeneity are discussed, and implications for public health are explored.
-
Ditton P: Mental Health and Treatment of Inmates and Probationers. Washington, DC, US Bureau of Justice Statistics, 1999.
-
James DJ, Glaze LE: Mental Health Problems of Prison and Jail Inmates. Washington, DC, US Bureau of Justice Statistics, 2006.
Self-reports? I’m sure a lot of very dangerous people would rather be in a mental ward than in prison. In Maximum Security prisons, I have no doubt that many are made unwell mentally by isolation and 24/7 lighting; but I think it best to err on the side of dangerous persons not being put into a mental ward with very vulnerable people.
And, I think we do need to allow people who suffer from psychosis and who are overwhelmed and very vulnerable to have a stay sufficient to stabilize them and we need to provide them with some support that would help them stay more stable without treating them like they must be mentally ill every minute of every day, and could blow up, at any time. Providing housing without making it conditional on compliance, seems to be working in some places.
No matter how mentally ill a person is, they’re not crazy all the time, whether they’re taking medication or not. It’s important to recognize that when they’re lucid and treat them as being such, when they are.
I must admit to still being confused as to the yes or no, 0 or 1 concept regarding medication. There seems to be no middle ground where short term or low dose appropriate medicating is considered, nor is the option of a controlled environment being made available as a half way between jail/prison or an institution.
What seems to be the driver is cost. Housing and providing counseling is expensive, med checks are cheap. Add in the myth that all people can become productive members of society and you have a fantasy that will, and is, creating real hardship in the community.
We see the results in those living under bridges, in the woods, lining up at the churches for meals and food. They disrupt the lives not only of family, but also society in general. We have the bleed over in that programs to help handicapped adults in my community are being cut leaving one of the most vulnerable populations exposed to uncertainty.
One of the stupidest ideas I ever heard was our State wanted to close a home for handicapped adults. The concept being that family should be responsible. The problem was the parents of these adults were themselves moving into nursing homes. These folks had spent their entire lives taking care of their children and were now facing the uncertainty of what would happen to their children when they were no longer able to provide care.
We as a society need to understand that as a society we have a responsibility to those who are most vulnerable and provide the resources necessary to provide a basic level of care. I would venture to guess that a lot of money is being wasted that could be better spent on direct care that would be of benefit to everyone.
Steve Lucas
Wiley,
Well put. Wait til you see his results. Coming soon…
Since reading and responding to this post, I’ve been thinking about a woman I used to be acquainted with who probably did suffer from what could reasonably described as schizophrenia. She lived alone in an apartment in a building one of my caregiving clients lived in. I saw her there, and on a bus from time to time. She was always lucid when I talked to her, but sometimes she was more wispy and seemed more vulnerable than others.
She asked me, while she was visiting my client if I would consider helping her with her apartment. She was having a hard time keeping it in order and was clearly frustrated and unhappy with it. I told her I could not, but asked her to show me anyway, because maybe I could give her some advice, and I wanted to ask her what kind of options she had. Her apartment was disorderly and she needed it. She was living on disability with food stamps, but she was not eligible for any in-home caregiving— it was either on her own, or in a group home.
What I’ve seen in an adult foster home made me fear it and fear for others in it.
I don’t scare easily.
I do think that with as little as 6 or 8 hours of in-home help with cleaning, shopping, and cooking (and a little company) she would have been more capable and less likely to get overwhelmed or too lonely. Had my circumstances been different, and she were eligible, I would have gladly taken the job. But I have experience with mentally ill and mentally impaired people and am capable of staying calm and being calming. I also know when to exit, stage left. I would also have had no problem recommending she go to the hospital should she be incapable of basic self-care, emotionally distraught to the degree that she could not manage herself, or psychotic.
But how do you teach “unskilled workers” (it all takes skills) to be comfortable around the mentally ill and mature enough to deal with the unexpected in a calm, helpful, and appropriate way? It requires attentiveness and thinking on your feet. I didn’t see a lot of that when I was in a mental ward for the second time— quite a few of the staff seemed totally unaware of their affect and were uselessly emotional, reactionary, and sometimes paranoid. But the food was great, and it was nice to be fed for one week and not have to be responsible for anyone but myself. Two weeks was just sandbagging for V.A. money, stubbornness, and controlling behavior in my considered opinion; especially since they were not interested in discussing my actual problems.
A lot of people need just a little help most of the time, and a lot of help from time to time.
Sadly much of the care given to the homeless or those with marginal situations is given by the community they live in, by those they come in contact with, on a day to day basis. My small city’s urban center has declined to the point where rents are now cheap enough to attract galleries and other small businesses. One gallery owner I spoke with openly talks about the challenge of convincing suburban customers it is safe to come downtown.
She knows all the street people, as does the beat patrolman, who has their case workers phone number. The reality is it is faster to call the case worker than go through the system. Some street people are allowed in the gallery, some are not, and it is up to her to deal with them in whatever state they appear in at the moment.
My downtown church is currently dealing with a person that is coming in and disturbing the service. We are not equipped to deal with this person and they have discovered that making a fuss gets them what they want, food and money.
We do need a system where there is basic contact with these people. Going back many decades I was taught in a psychology class the importance of social contact. This seems to have been lost in our current system.
Steve Lucas
“..but I think it best to err on the side of dangerous persons not being put into a mental ward with very vulnerable people.”
Wiley and I rarely agree, but on this one right on the mark!
And the vulnerable aren’t just the patients, but the staff as well.