Posted on Saturday 5 December 2015
![]()
Occam’s razor, also known as Ockham’s razor, and sometimes expressed in Latin as lex parsimoniae [the law of parsimony, economy or succinctness], is a principle that generally recommends selecting from among competing hypotheses the one that makes the fewest new assumptions. The strict translation is "Plurality is not to be posited without necessity."
But I did decide that chasing this down would be worth the effort. It might take a while because this has obviously worked its way into government guidelines. So I’m going to table it for a time when I run out of other things to look into. In the meanwhile, I’m going to see how it worked its way into my clinic.
by Brett D. Thombs, PhD, James C. Coyne, PhD, Pim Cuijpers, PhD, Peter de Jonge, PhD, Simon Gilbody, DPhil, John P. A. Ioannidis, MD DSc, Blair T. Johnson, PhD, Scott B. Patten, MD PhD, Erick H. Turner, MD, and Roy C. Ziegelstein, MDCanadian Medical Association Journal. 2012 184[4]:413-418.…
Conclusion:
The prevalence of depression and the availability of easy-to-use screening instruments make it tempting to endorse widespread screening for the disease. However, screening in primary care is a resource-intensive endeavour, does not yet show evidence of benefit and would have unintended negative effects for some patients. Evidence from one simulation study using Canadian national data found that the overall burden of depression could be reduced by providing more consistent treatment to reduce symptoms and prevent relapse among people with recurrent disorders, but not by increasing treatment through screening.We hope that a rigorous review of current evidence will encourage the developers of future guidelines, including members of the Canadian Task Force on Preventive Health Care, to carefully consider their stance on screening for depression. We also hope that, consistent with the 2010 guidelines of the National Institute for Health and Clinical Excellence, such developers will conclude that evidence from well-conducted, randomized, controlled trials of the benefit of screening, in excess of its likely harms and costs, is needed before it can be recommended in primary care settings. Specifically, the benefits and harms of screening should be tested in a trial in which all patients identified as having depression should have access to the same integrated care for their condition, regardless of whether they are identified through screening in the intervention group or via physician recognition and referral in a control group. It is possible that such a trial would find that screening benefits patients to a degree that would justify the cost and the harms associated with the process. Until then, however, given the lack of evidence of benefit from screening and the concerns that we have described, it is not reasonable to simply assume that depression screening is good policy.
Key points
Canadian Task Force on Preventive Health CareCanadian Medical Association Journal. 2013 185[9]:775-782.…
Conclusion:
Our recommendations highlight the lack of evidence about the benefits and harms of routinely screening for depression in adults. In the absence of a demonstrated benefit of screening, and in consideration of the potential harms, we recommend not routinely screening for depression in primary care settings, either in adults at average risk or in those with characteristics that may increase their risk of depression. However, clinicians should be alert to the possibility of depression, especially in patients with characteristics that may increase their risk of depression, and should look for it when there are clinical clues, such as insomnia, low mood, anhedonia and suicidal thoughts.Summary of recommendations for clinicians and policy-makers:
Recommendations on screening for depression in primary care settings are provided for people 18 years of age or older who present at a primary care setting with no apparent symptoms of depression. These recommendations do not apply to people with known depression, with a history of depression or who are receiving treatment for depression.
by Roger C. Bland CM MB ChB, David L. Streiner PhDCanadian Medical Association Journal. 2013 185[9]:753-754.…
Key points
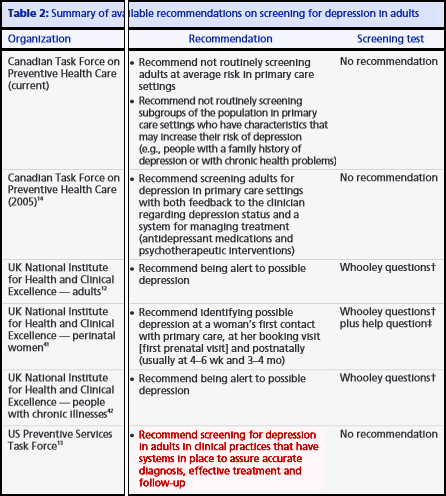
Summary for Canada, US, UK
table from the Canadian Task Force on Preventive Health Care 2013
Screening is not recommended. In the US, it says don’t screen unless you are in a system that can offer full services to evaluate, treat, and follow-up the results.
Centers for Medicare & Medicaid Services [CMS]Final DecisionOctober 14, 2011The Centers for Medicare & Medicaid Services [CMS] has determined that the evidence is adequate to conclude that screening for depression in adults, which is recommended with a grade of B by the U.S. Preventive Services Task Force [USPSTF], is reasonable and necessary for the prevention or early detection of illness or disability and is appropriate for individuals entitled to benefits under Part A or enrolled under Part B.
Therefore CMS will cover annual screening for depression for Medicare beneficiaries in primary care settings that have staff-assisted depression care supports in place to assure accurate diagnosis, effective treatment and follow-up. For the purposes of this decision memorandum:


 But thumbing through the blogs and news today, I kind of changed my mind. Here are three recent blurbs from Ed Silverman’s Pharmalot – companies who were clearly way over the line with their pricing. As an aside, they share something else kind of encouraging. In each case, somebody’s fighting back!…
But thumbing through the blogs and news today, I kind of changed my mind. Here are three recent blurbs from Ed Silverman’s Pharmalot – companies who were clearly way over the line with their pricing. As an aside, they share something else kind of encouraging. In each case, somebody’s fighting back!… “This will solve a big point of pain in health care costs,” said Dr. Steve Miller, the chief medical officer at Express Scripts. The decision comes amid ongoing controversy over Daraprim, which Turing last summer bought from another company and then boosted the price from $13.55 a pill to $750, a 5,000 percent increase. The price hike triggered a new round of scrutiny of pharmaceutical costs and transformed Shkreli — who used social media to deride his critics — into a poster boy for greed and outsized drug pricing…
“This will solve a big point of pain in health care costs,” said Dr. Steve Miller, the chief medical officer at Express Scripts. The decision comes amid ongoing controversy over Daraprim, which Turing last summer bought from another company and then boosted the price from $13.55 a pill to $750, a 5,000 percent increase. The price hike triggered a new round of scrutiny of pharmaceutical costs and transformed Shkreli — who used social media to deride his critics — into a poster boy for greed and outsized drug pricing… “The company knew its prices would put treatment out of reach for millions of Americans,” said Senator Ron Wyden, a Democrat from Oregon who, along with Iowa Republican Senator Chuck Grassley, discussed their probe at a media briefing. “If Gilead’s approach is the future of how blockbuster drugs are launched in America, it’s going to cost billions and billions of dollars to treat just a fraction of patients in America”…
“The company knew its prices would put treatment out of reach for millions of Americans,” said Senator Ron Wyden, a Democrat from Oregon who, along with Iowa Republican Senator Chuck Grassley, discussed their probe at a media briefing. “If Gilead’s approach is the future of how blockbuster drugs are launched in America, it’s going to cost billions and billions of dollars to treat just a fraction of patients in America”…
 The three companies mentioned above developed nothing. They got hold of their products and are only looking to reap a big profit. There’s not much else to say. And when I step back and think about it, this issue of the financial bottom line is the ultimate culprit in everything I find myself complaining about in modern medicine – the conflicts of interest, the jury-rigged clinical trials, the distortions of scientific evidence, the corrupted key opinion leaders, the outrageous pricing of drugs, etc.
The three companies mentioned above developed nothing. They got hold of their products and are only looking to reap a big profit. There’s not much else to say. And when I step back and think about it, this issue of the financial bottom line is the ultimate culprit in everything I find myself complaining about in modern medicine – the conflicts of interest, the jury-rigged clinical trials, the distortions of scientific evidence, the corrupted key opinion leaders, the outrageous pricing of drugs, etc. 


 But it seems to me like there’s always the rumbling of distant thunder. As physicians, we should be attuned to such early warnings. After all, there’s an important medical principle involved – Preventive Medicine. While talking about such things can begin to sound like early psychosis, the alternatives are too well known to ignore. Particularly dangerous are things that look innocent, maybe even like progressive reform to solve some contemporary problem, but later turn out to have been the proverbial wolf in sheep’s clothing.
But it seems to me like there’s always the rumbling of distant thunder. As physicians, we should be attuned to such early warnings. After all, there’s an important medical principle involved – Preventive Medicine. While talking about such things can begin to sound like early psychosis, the alternatives are too well known to ignore. Particularly dangerous are things that look innocent, maybe even like progressive reform to solve some contemporary problem, but later turn out to have been the proverbial wolf in sheep’s clothing.  It was such a good idea that the Texas Mental Health officials became evangelical, ultimately spreading the gospel to about a third of our states [with a bit of financial help from the manufacturers]. When it was all said and done, the Texas Medicaid program was all but bankrupt; it became clear that the Atypicals were neither more effective nor better tolerated than the older drugs; and they had some toxic side effects all their own.
It was such a good idea that the Texas Mental Health officials became evangelical, ultimately spreading the gospel to about a third of our states [with a bit of financial help from the manufacturers]. When it was all said and done, the Texas Medicaid program was all but bankrupt; it became clear that the Atypicals were neither more effective nor better tolerated than the older drugs; and they had some toxic side effects all their own. clinical effects was open-minded, exploratory, comprehensive, clinical observation…
clinical effects was open-minded, exploratory, comprehensive, clinical observation…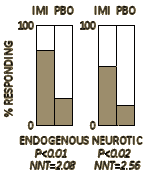 On the placebo, 6 did well and 22 badly. This is a highly significant difference, and, with Yates’s correction applied, P<0.01. Of the 42 cases of reactive depression 22 received imipramine and 20 the placebo. Of those given imipramine 13 were improved and 9 were not; while of the 20 controls 4 improved and 16 showed a poor result. This, too, is a significant result [P<0.02]. When improvement occurred it was nearly always evident by the end of the third week, sometimes as early as the fourth or fifth day. The mean was 9 to 10 days…
On the placebo, 6 did well and 22 badly. This is a highly significant difference, and, with Yates’s correction applied, P<0.01. Of the 42 cases of reactive depression 22 received imipramine and 20 the placebo. Of those given imipramine 13 were improved and 9 were not; while of the 20 controls 4 improved and 16 showed a poor result. This, too, is a significant result [P<0.02]. When improvement occurred it was nearly always evident by the end of the third week, sometimes as early as the fourth or fifth day. The mean was 9 to 10 days…